Clear Sky Science · en
Investigating neural impairments in psychotic disorders using electroencephalography and cortical spheroids
Peering into the roots of serious mental illness
Schizophrenia and bipolar disorder can dramatically disrupt people’s thoughts, emotions, and daily lives, yet the biological glitches that drive these illnesses are still being uncovered. This study brings together two powerful tools—brainwave recordings from living adults and tiny lab-grown “mini-brains” made from their own cells—to explore what goes wrong at the connections between brain cells and how those problems might begin very early in life.
How brainwaves reveal fragile connections
The researchers first recorded electrical activity from the scalp using electroencephalography (EEG) in ten people with schizophrenia or bipolar disorder and five healthy volunteers. They focused on a response called long-term potentiation–like (LTP-like) plasticity, which reflects how well the brain strengthens its responses to repeated visual stimulation, a basic ingredient of learning and memory. In the patient group, this plasticity faded more over time than in the healthy group, hinting that their brain circuits were less able to “tune up” their responses. Another EEG signal, mismatch negativity—which reflects how automatically the brain detects small changes in sound—did not differ between the small groups in this study, even though larger studies often find it reduced in such disorders. Together, these recordings suggest that at least some forms of synaptic adaptation are weakened in people with psychotic illnesses.
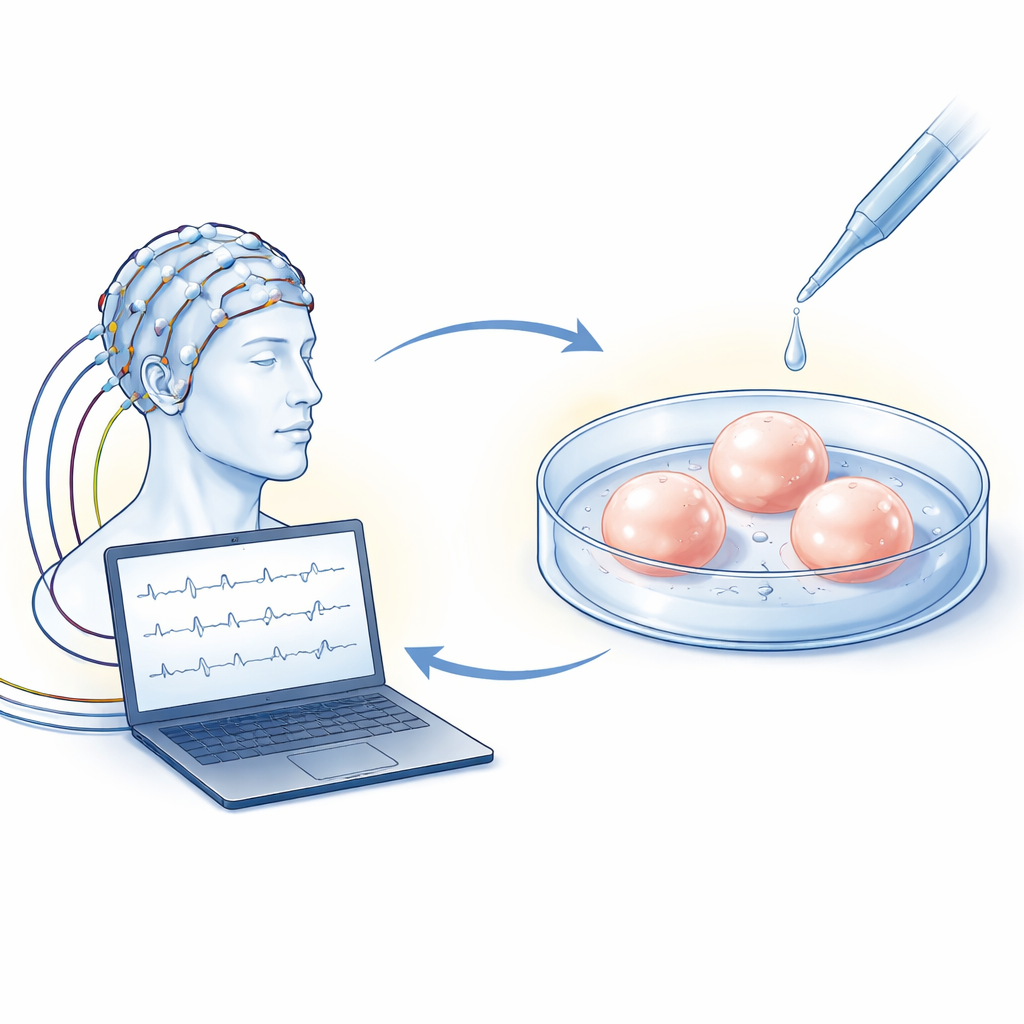
Growing mini-brains from skin cells
To look deeper, the team turned to human cortical spheroids, often called mini-brains. They reprogrammed skin cells from each participant into stem cells and then coaxed these to develop into three-dimensional clumps of brain tissue resembling the fetal cerebral cortex. These spheroids contained mostly excitatory nerve cells that talk to each other using the chemical messenger glutamate. Using tiny glass electrodes, the scientists measured how easily these cells fired electrical signals and passed currents to their neighbors. Neurons from people with bipolar disorder needed stronger input to fire, indicating they were less excitable. In spheroids from people with schizophrenia, the strength of spontaneous incoming signals was smaller, suggesting early changes in how nerve cells communicate within the network.
Weakened glutamate transport and tired powerhouses
The team then stained the mini-brains for key proteins. One, called VGLUT1, packages glutamate into small sacs that are released at synapses. Both schizophrenia- and bipolar-derived spheroids showed fewer cells rich in VGLUT1 compared with controls, pointing to a shared deficit in the machinery that loads glutamate for release. Because sending signals is energy-hungry, the researchers also examined the tiny power plants of the cell—mitochondria—by measuring oxygen use and acid production in slices of the spheroids. Mini-brains from bipolar patients, especially those who do not respond well to lithium, had lower baseline oxygen consumption, a sign of reduced mitochondrial activity, while those from people with schizophrenia showed relatively normal energy measures in this small sample.
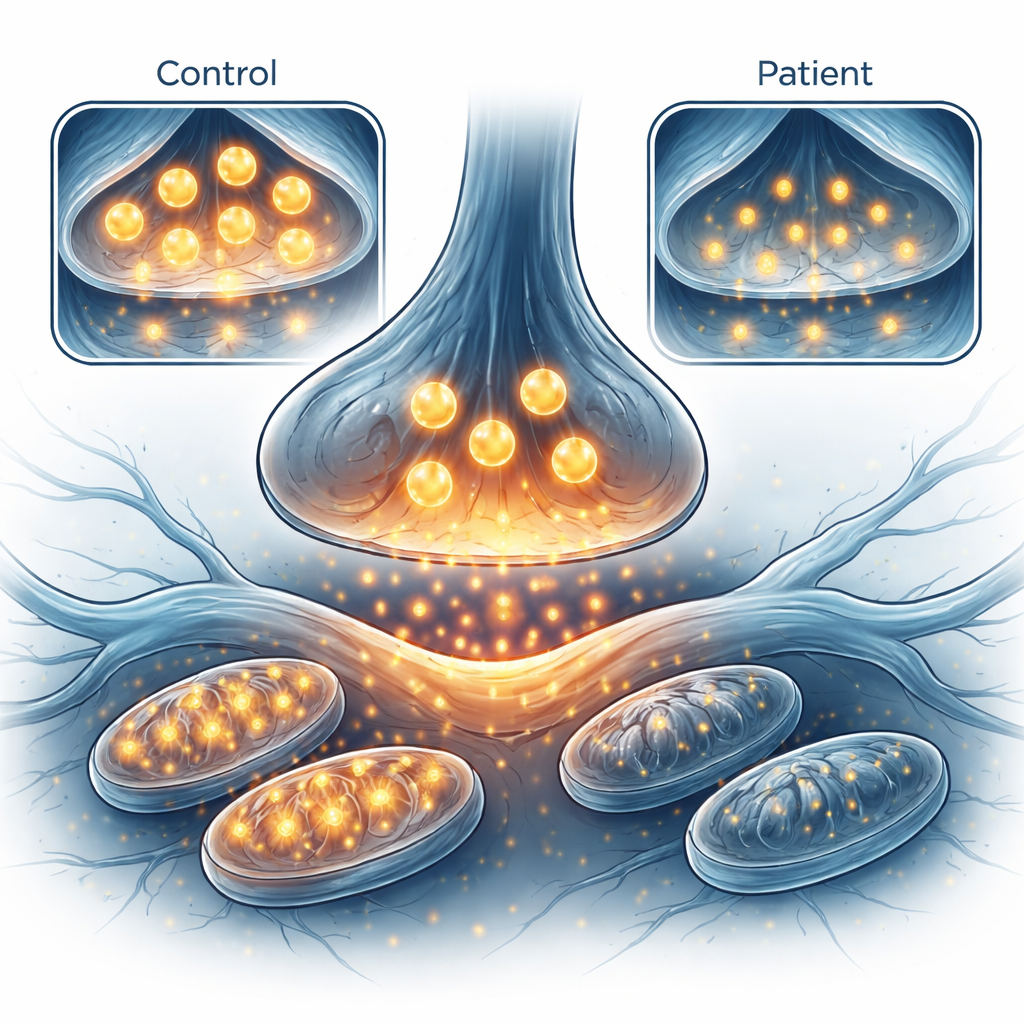
Linking brain signals to cell energy
Finally, the scientists asked whether differences in brainwaves were related to differences in the mini-brains grown from the same individuals. Across participants, those whose EEGs showed stronger LTP-like plasticity tended to have mini-brains with higher basal mitochondrial respiration, meaning more active energy production. There was also a hint that higher VGLUT1 levels tracked with better plasticity. Although these trends fell short of strict statistical cutoffs once multiple comparisons were taken into account, they support the idea that healthy synaptic strengthening depends on robust mitochondrial function and intact glutamate handling, and that these relationships may already be altered early in development in people who later develop psychosis.
What this means for understanding psychosis
For non-specialists, the message of this work is that serious mental illnesses like schizophrenia and bipolar disorder may share common, early-arising faults in how brain cells signal and power their activity. The mini-brains suggest that, long before symptoms appear, some neurons may release less glutamate and run on less efficient energy supplies, while EEG recordings show that the adult brain’s ability to fine-tune its responses is weakened. Though the study is small and the lab-grown tissue is still more like a developing brain than a mature one, combining live brain recordings with personalized mini-brains offers a promising window into the roots of psychosis and may eventually guide more targeted treatments aimed at restoring synaptic function and cellular energy.
Citation: Reis de Assis, D., Pentz, A.B., Requena Osete, J. et al. Investigating neural impairments in psychotic disorders using electroencephalography and cortical spheroids. Transl Psychiatry 16, 114 (2026). https://doi.org/10.1038/s41398-026-03863-4
Keywords: schizophrenia, bipolar disorder, brain organoids, synaptic plasticity, mitochondria