Clear Sky Science · en
Postpartum Psychosis: could genetic vulnerability to insomnia or short sleep duration be protective?
Why Sleep and New Motherhood Matter
Becoming a parent often means sleepless nights, dramatic life changes, and intense emotions. For most women these challenges are exhausting but manageable. For a small number, however, the weeks after birth can bring a psychiatric emergency called postpartum psychosis, with confusion, extreme mood swings, and even hallucinations. This study asks a surprising question with real-world consequences: could having genes that make you prone to insomnia or short sleep actually protect some women with bipolar disorder from developing postpartum psychosis?
A Rare but Serious Condition
Postpartum psychosis affects roughly 1–2 in every 1,000 women who give birth, but the risk is far higher in women with bipolar disorder. Most episodes start suddenly in the first days or weeks after delivery and can involve mania, severe depression, or psychosis. Because suicide and infanticide are real risks, it is a medical emergency. Yet not all women with bipolar disorder become unwell after childbirth, and many women who do develop postpartum psychosis have no prior psychiatric diagnosis. Clinicians therefore struggle to predict who is most at risk and how to target preventative care.
Sleep, Stress, and Vulnerability
Pregnancy and early motherhood disrupt sleep for almost everyone. Short nights, broken sleep, and irregular schedules are the norm. Outside the perinatal period, sleep loss is known to trigger mania and psychosis in vulnerable people, and losing even one night of sleep can worsen symptoms in bipolar disorder. Earlier research suggested that women with bipolar disorder who are sensitive to sleep loss may be more likely to develop postpartum psychosis. Still, it remained unclear whether this link was simply about circumstances around childbirth or whether deeper biological vulnerabilities—encoded in our genes—might shape how a woman’s brain responds to disrupted sleep.
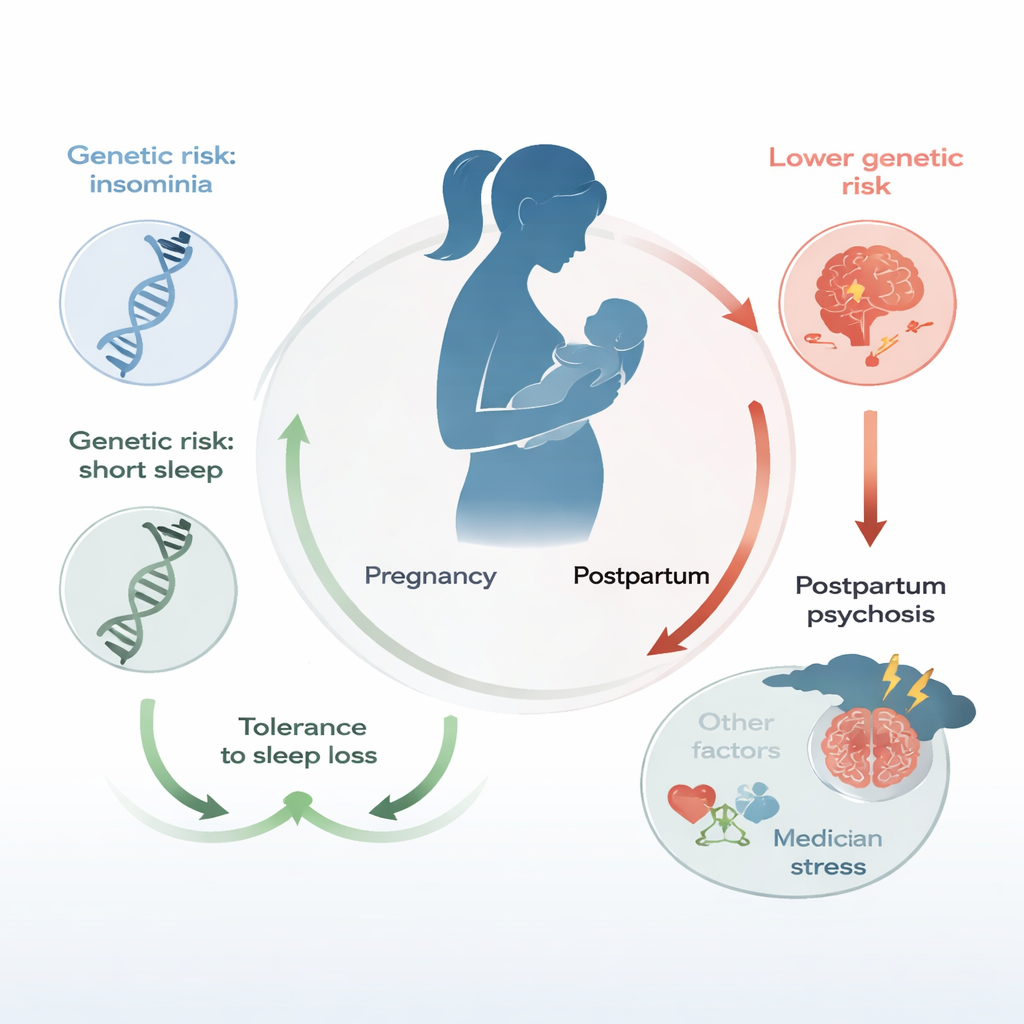
Using Genetic Clues from Sleep
The researchers studied 343 women of European ancestry with bipolar disorder who had given birth: 117 had experienced postpartum psychosis and 226 had not. They calculated “polygenic risk scores” for each woman, combining the small effects of many genetic variants linked to bipolar disorder, schizophrenia, and several sleep traits: insomnia, short sleep, long sleep, sleep efficiency, and total sleep duration. These scores are not diagnoses, but estimates of inherited tendency. The team then used statistical models to see whether higher or lower genetic risk for these traits was associated with the chance of developing postpartum psychosis after childbirth, while also accounting for bipolar subtype and ancestry.
A Counterintuitive Finding
The most striking result was the opposite of what many might expect. Women with lower genetic risk for insomnia and short sleep were more likely to develop postpartum psychosis, while those with higher genetic risk for these sleep problems were less likely to do so. Women in the lowest tenth of genetic risk for insomnia or short sleep had about twice the risk of postpartum psychosis as women in the highest tenth. Genetic scores for long sleep, sleep efficiency, and overall sleep duration showed no clear link, nor did scores for bipolar disorder or schizophrenia. When the researchers combined information on bipolar subtype with the insomnia and short-sleep scores, their ability to distinguish women who would or would not develop postpartum psychosis improved compared with using bipolar subtype alone—though the prediction was still far from perfect.
What Might Explain This?
How could a genetic tendency toward insomnia or short sleep be protective? One possibility is that women who are biologically prone to poor sleep may, over many years, adapt psychologically to functioning while tired. By the time they reach pregnancy, the abrupt sleep loss that comes with caring for a newborn might feel less novel and less destabilizing to their mood. In contrast, women whose bodies and brains are used to longer or more stable sleep may be more shocked by sudden, severe sleep disruption after childbirth. This study’s deeper genetic analyses did not prove that insomnia or short sleep directly cause or prevent postpartum psychosis. Instead, the authors suggest that the same biological pathways that influence how we sleep may also help determine how resilient we are to the emotional and cognitive strain of sleep loss around childbirth.
What This Means for Families
For families and clinicians, the key message is not that insomnia is “good,” but that sleep history and genetic make-up may shape a woman’s vulnerability to postpartum psychosis in unexpected ways. The work shows that adding genetic information about sleep traits can modestly improve risk estimates for women with bipolar disorder, potentially guiding closer monitoring or early support in the future. However, these genetic scores are not yet accurate or generalizable enough for routine clinical use, and the study was limited to women of European ancestry with bipolar disorder. Rather than changing care today, the findings open a new line of research: understanding how lifelong sleep patterns and underlying biology interact with the upheaval of childbirth to trigger—or buffer against—severe mental illness.
Citation: Petrosellini, C., Eriksson, S.H., Meyer, N. et al. Postpartum Psychosis: could genetic vulnerability to insomnia or short sleep duration be protective?. Transl Psychiatry 16, 89 (2026). https://doi.org/10.1038/s41398-026-03856-3
Keywords: postpartum psychosis, bipolar disorder, sleep and mental health, genetic risk, insomnia