Clear Sky Science · en
Untargeted 1H NMR-based metabolomics unveils distinct circulating biochemical signatures between treatment-resistant and non-treatment-resistant schizophrenia patients: a pilot study
Why blood chemistry matters in difficult-to-treat psychosis
Many people with schizophrenia improve on standard medications, but about one in three continue to struggle with hallucinations, delusions and thinking problems despite trying several drugs. This study explores whether simple blood tests can reveal hidden chemical differences between patients who respond to treatment and those who do not, potentially paving the way for more personalized care and new therapies.
Two groups with the same diagnosis, but different outcomes
The researchers focused on 26 adults diagnosed with schizophrenia and divided them into two equal groups. One group responded to common antipsychotic medications, while the other had “treatment-resistant” schizophrenia, meaning their symptoms stayed troublesome despite at least two adequate drug trials and now required clozapine, the last-line antipsychotic. By comparing these two sets of patients, the team aimed to move beyond symptoms and brain scans and instead look for clues in the circulating chemicals carried in the blood.
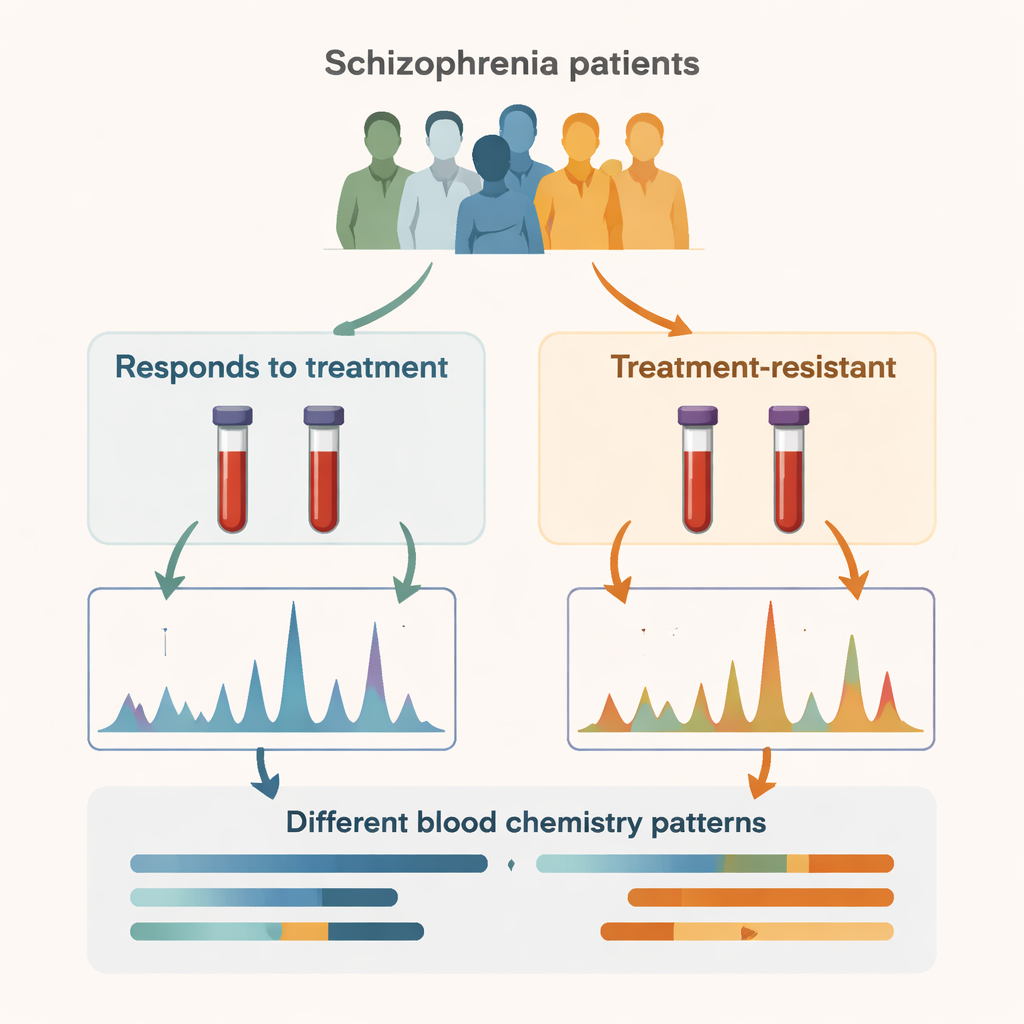
Reading the body’s chemical fingerprints
To do this, the scientists used a technique called proton nuclear magnetic resonance (1H NMR) metabolomics, which can measure dozens of small molecules in a blood sample at once. They identified 44 different metabolites in each person’s serum and then used advanced statistics to see whether overall patterns differed between the two groups. The resulting chemical “maps” clearly separated treatment-resistant from non–treatment-resistant patients, suggesting that the body-wide metabolism of these two groups is measurably distinct, even though they share the same broad psychiatric diagnosis.
Amino acids, brain signals and cell membranes
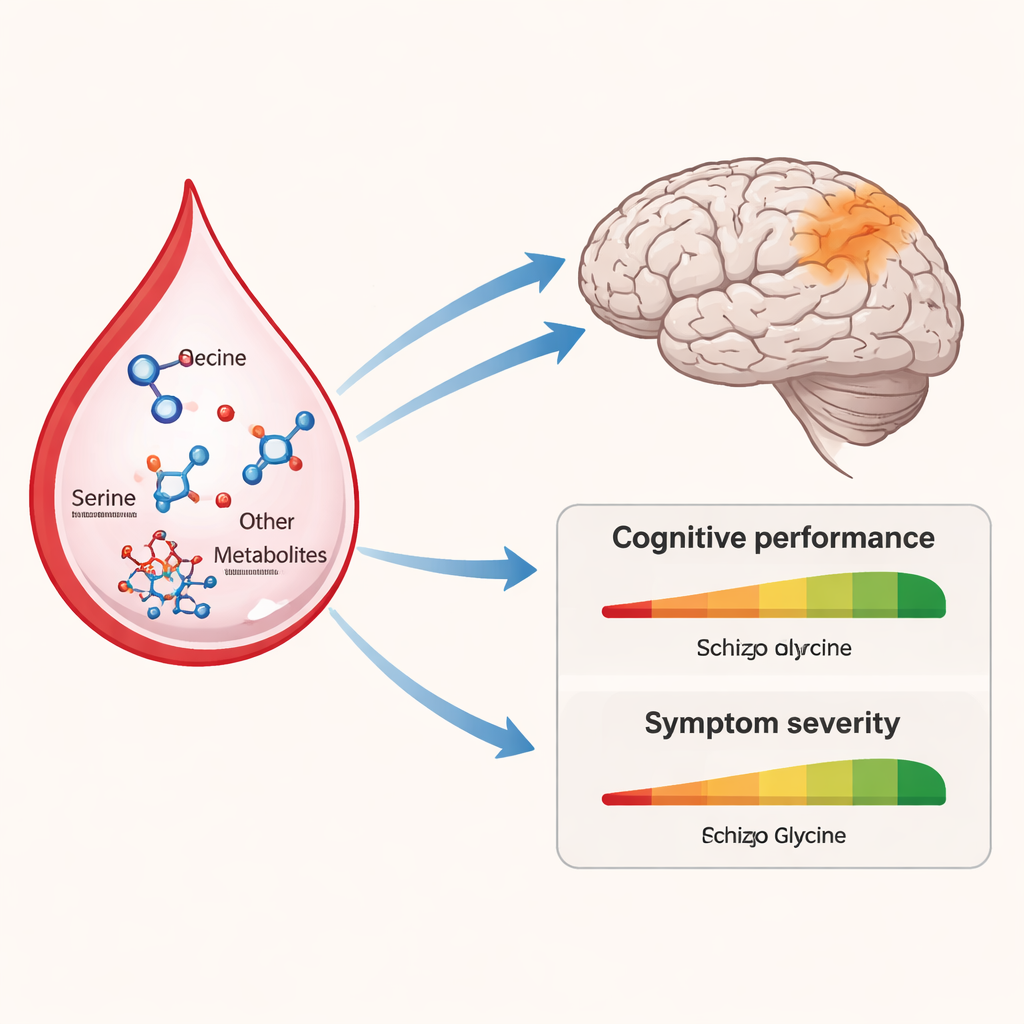
Among the many molecules examined, several amino acids stood out. Levels of serine and proline were lower, while glycine, glutamine, and some energy- and lipid-related metabolites such as formate, betaine and lactic acid tended to be higher in treatment-resistant patients. Follow-up pathway analysis indicated that these changes touch key biological routes: the serine–glycine system that feeds into NMDA-type glutamate receptors (important for learning and memory), and lipid pathways involved in building and maintaining cell membranes. In particular, serine changes pointed to disturbances in sphingolipid and phosphatidylethanolamine metabolism, two lipid families that influence how brain cells communicate and respond to inflammation.
Linking blood molecules to thinking and symptoms
Because serine and glycine directly influence NMDA receptors in the brain, the team performed a more targeted measurement using high-performance liquid chromatography to distinguish the two mirror forms of serine, called L-serine and D-serine. Overall levels of these amino acids did not differ statistically between groups once age was considered. However, when the researchers looked at behavior and cognition, a more nuanced picture emerged. Across all 26 patients, higher D-serine levels were linked to better “executive” abilities—skills such as planning, flexible thinking and problem solving. Within the treatment-resistant subgroup specifically, a higher ratio of D-serine to total serine tracked with better executive performance, and higher glycine was associated with fewer “disorganization” symptoms, such as confused speech and chaotic behavior. These relationships were not seen in the patients who responded well to standard treatment.
What this could mean for future care
Although this pilot study is small and cannot prove cause and effect, it shows that treatment-resistant schizophrenia has a distinct metabolic signature in blood and highlights serine and glycine pathways as possible hubs where systemic metabolism, NMDA receptor function and cognition intersect. For a layperson, this means that in hard-to-treat schizophrenia, the problem may not only lie in dopamine—a classic drug target—but also in broader chemical circuits that affect how brain cells use energy, build membranes and fine-tune critical signaling receptors. If confirmed in larger groups, blood-based markers such as serine-related measures could eventually help doctors identify at-risk patients earlier and guide the development of therapies that adjust these metabolic pathways to improve both symptoms and thinking skills.
Citation: Marino, C., Zhang, S., De Simone, G. et al. Untargeted 1H NMR-based metabolomics unveils distinct circulating biochemical signatures between treatment-resistant and non-treatment-resistant schizophrenia patients: a pilot study. Transl Psychiatry 16, 108 (2026). https://doi.org/10.1038/s41398-026-03853-6
Keywords: schizophrenia, treatment-resistant schizophrenia, metabolomics, serine glycine pathway, NMDA receptor