Clear Sky Science · en
Maternal cariprazine exposure effects on lactating offspring sterol biosynthesis
Why this matters for nursing mothers and babies
As more women rely on modern medicines while pregnant and breastfeeding, an urgent question arises: how do these drugs affect a baby’s rapidly developing brain? This study looks at cariprazine, a widely used antipsychotic medication, and asks whether a mother’s treatment during breastfeeding can silently alter key brain-building chemistry in her nursing offspring.
From brain “building blocks” to potential weak spots
Cholesterol is often viewed as a dietary villain, but inside the body it is also a vital building block for every cell, especially in the brain. During early life, the infant brain makes large amounts of cholesterol through a multi-step chemical pathway. If this pathway is disrupted, intermediate molecules can build up and become harmful. In rare genetic conditions like Smith–Lemli–Opitz syndrome, a faulty enzyme in the last step of this pathway leads to serious developmental problems, in part because a fragile cholesterol-like molecule called 7-dehydrocholesterol (7-DHC) accumulates and easily turns into toxic oxidized products.
When a mental health drug meets infant nutrition
Cariprazine is a “third-generation” antipsychotic prescribed for conditions such as schizophrenia and bipolar disorder. It acts on brain signaling chemicals like dopamine and serotonin and has a very long-lasting active form that stays in the body for weeks. Less well known is that cariprazine also blocks the same last step in cholesterol production as the enzyme problem seen in Smith–Lemli–Opitz syndrome. This means it can raise levels of 7-DHC and related compounds. While previous animal work showed that cariprazine taken during pregnancy alters cholesterol chemistry in embryos, almost nothing was known about what happens when mothers take the drug while breastfeeding. 
A mouse model of breastfeeding exposure
To answer this, the researchers gave lactating mice a daily dose of cariprazine chosen to match a low human therapeutic dose. They worked with two types of mice: normal animals and animals carrying a single copy of a gene change that mimics the human cholesterol-synthesis disorder. Over the first ten days after birth, the mothers received injections of either cariprazine or a harmless salt solution, while their pups were exposed only through nursing. On day eleven, the team collected blood, liver, and brain samples from both mothers and pups and used sensitive mass-spectrometry methods to measure drug levels and key cholesterol-related molecules.
Drug in the milk, drug in the baby brain
The measurements revealed that cariprazine taken by the mother does indeed pass through milk into nursing offspring. Strikingly, although mothers had much higher drug levels than pups in their blood and livers, the concentration of cariprazine in the pups’ brains was similar to that in the mothers’ brains. In other words, standard blood or liver readings would have underrated how much of the drug was actually reaching the developing brain. In both normal and gene-altered pups, cariprazine exposure through breastfeeding consistently raised levels of 7-DHC and 8-DHC in the liver and brain, showing that the last step of cholesterol production was being blocked. These effects did not depend on the sex of the pups, and only modestly on their genetic background. 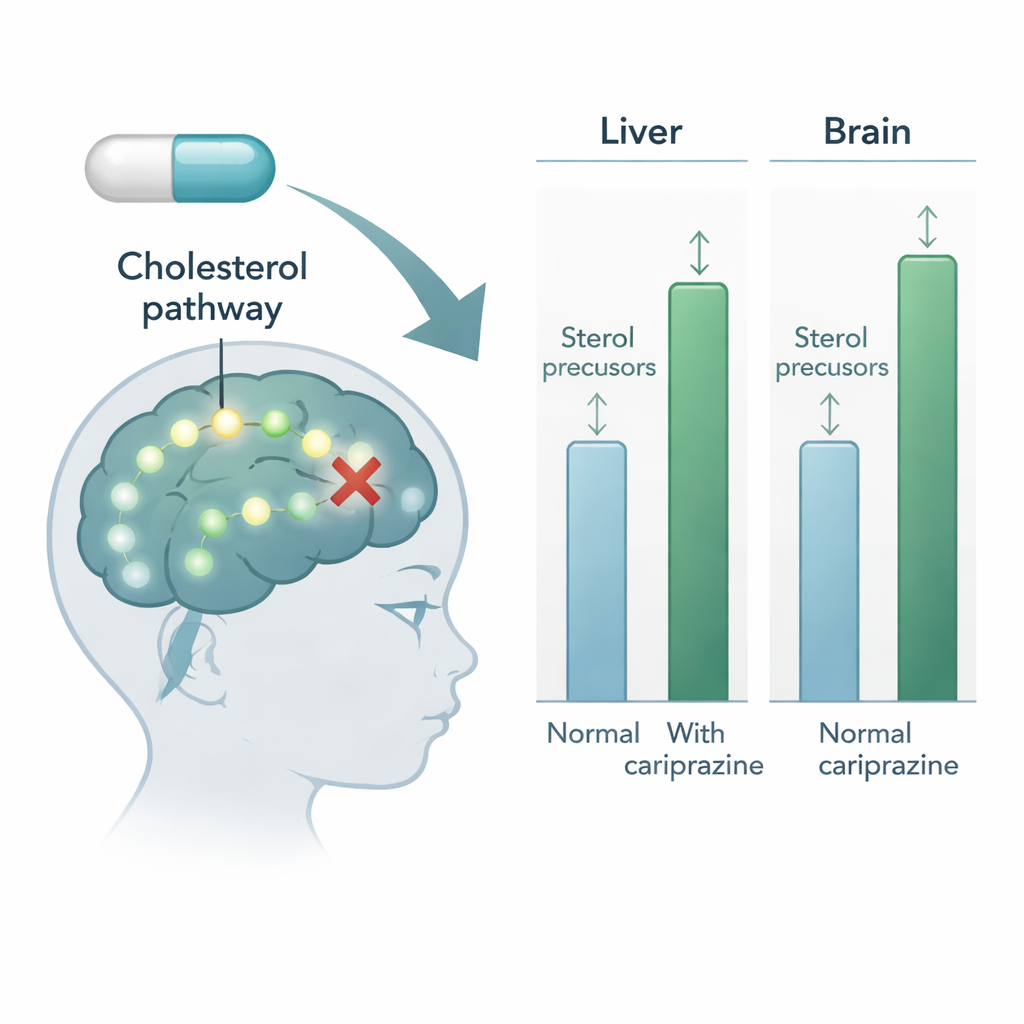
Broader concerns about combinations and hidden effects
Beyond cholesterol metabolism, the authors note that cariprazine and similar drugs can also affect mitochondria, the cell’s energy factories, and many brain signaling systems. They point out that more than half of postpartum women take at least one medication, and some take several that can each influence cholesterol chemistry. Other examples include certain antidepressants and cholesterol-lowering statins. When such drugs are combined, their effects on the infant’s sterol balance may reinforce one another, potentially increasing the risk of subtle, long-term changes in brain development that would not be obvious at birth.
What this means for real-world breastfeeding decisions
For lay readers, the core message is straightforward but important: in mice, cariprazine taken by nursing mothers reaches the brains of their offspring at meaningful levels and disrupts a key chemical pathway that builds and protects the developing brain. The study does not prove that the same thing happens in human babies, nor does it say that no mother should ever take needed psychiatric medication while breastfeeding. Instead, it raises a clear warning flag: this particular drug, especially when combined with others that affect cholesterol, may pose underappreciated risks during early life. Until careful human studies are done, the authors argue that clinicians and patients should weigh alternatives and use cariprazine cautiously in breastfeeding women.
Citation: Anderson, A.C., Sharma, K., Korade, Ž. et al. Maternal cariprazine exposure effects on lactating offspring sterol biosynthesis. Transl Psychiatry 16, 69 (2026). https://doi.org/10.1038/s41398-026-03850-9
Keywords: cariprazine, breastfeeding, cholesterol biosynthesis, infant brain development, antipsychotic medications