Clear Sky Science · en
Task-related differences in network connectivity and dynamics in people with severe opioid use disorder compared with healthy controls
Why this matters for the opioid crisis
Opioid addiction is often framed in terms of willpower or withdrawal, but at its core it is a disease of the brain. This study uses advanced brain scans to ask a practical question: how are the brain’s networks for reward, attention, and self-reflection wired differently in people with severe opioid use disorder who are on methadone, compared with healthy volunteers? The answers may help guide future brain-based treatments, such as noninvasive stimulation, that aim to reduce craving and relapse.
Looking inside the addicted brain
The researchers scanned 25 people with severe opioid use disorder receiving methadone and 22 healthy control participants while they performed two tasks inside an MRI scanner. In one task, participants anticipated winning or losing small amounts of money; in the other, they viewed drug-related images mixed with neutral pictures. Both tasks are well-established ways to probe how the brain responds to natural rewards (like money) and drug cues. Instead of just looking at which spots in the brain light up, the team focused on how whole networks of regions communicate with each other over time.
Networks that talk differently
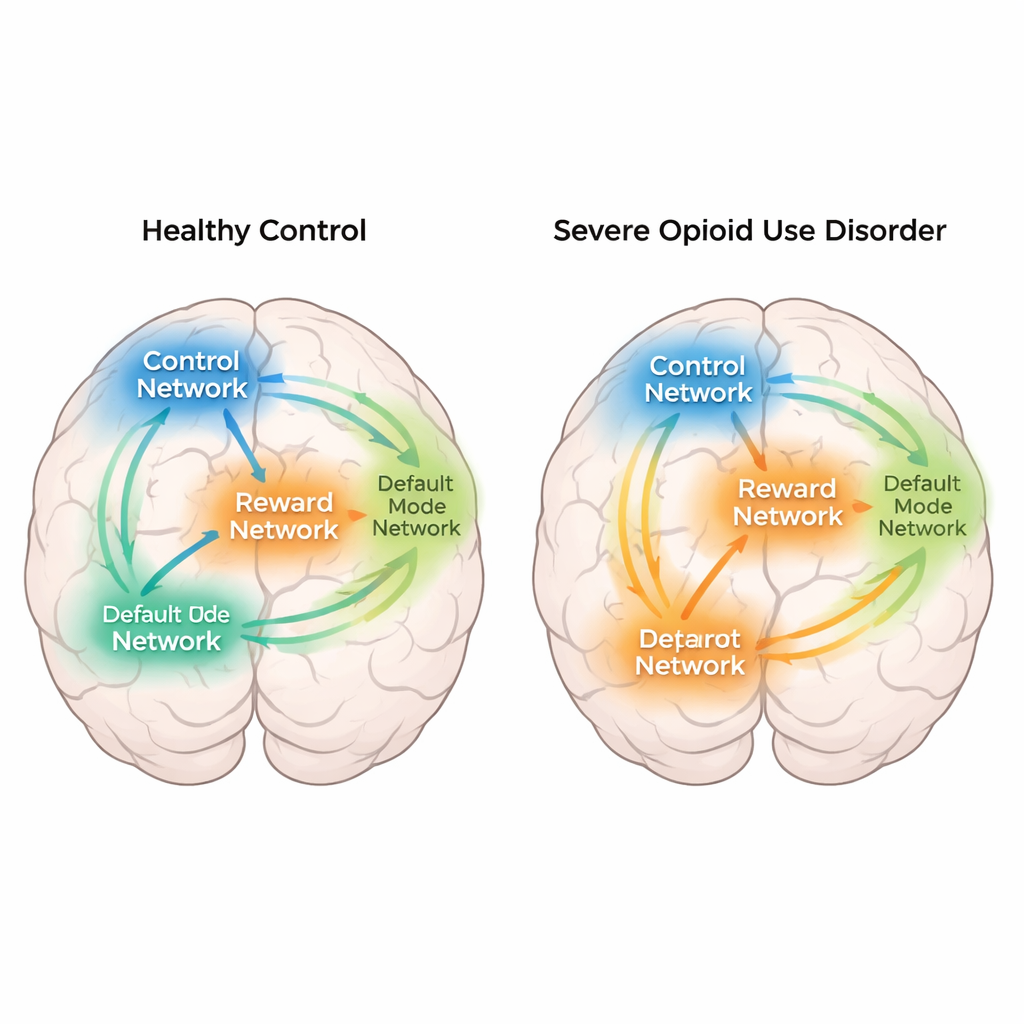
The study concentrated on several key brain networks: a reward network that includes the nucleus accumbens and related “ventromedial” regions; a control network that supports planning and self-control; attention and sensory networks that help us detect and respond to sights and sounds; and the default mode network, which is active when we daydream or think about ourselves. Using an information-theory measure called mutual information, the researchers quantified how strongly pairs of regions shared information during the tasks. Overall, people with opioid use disorder showed weaker connections across many networks than healthy participants, especially involving basic visual and movement areas. Yet when comparing reward or drug-related moments to neutral moments, the pattern flipped: people with opioid addiction showed stronger communication between the reward network and the control and default mode networks than healthy volunteers.
When rewards and drug cues take center stage
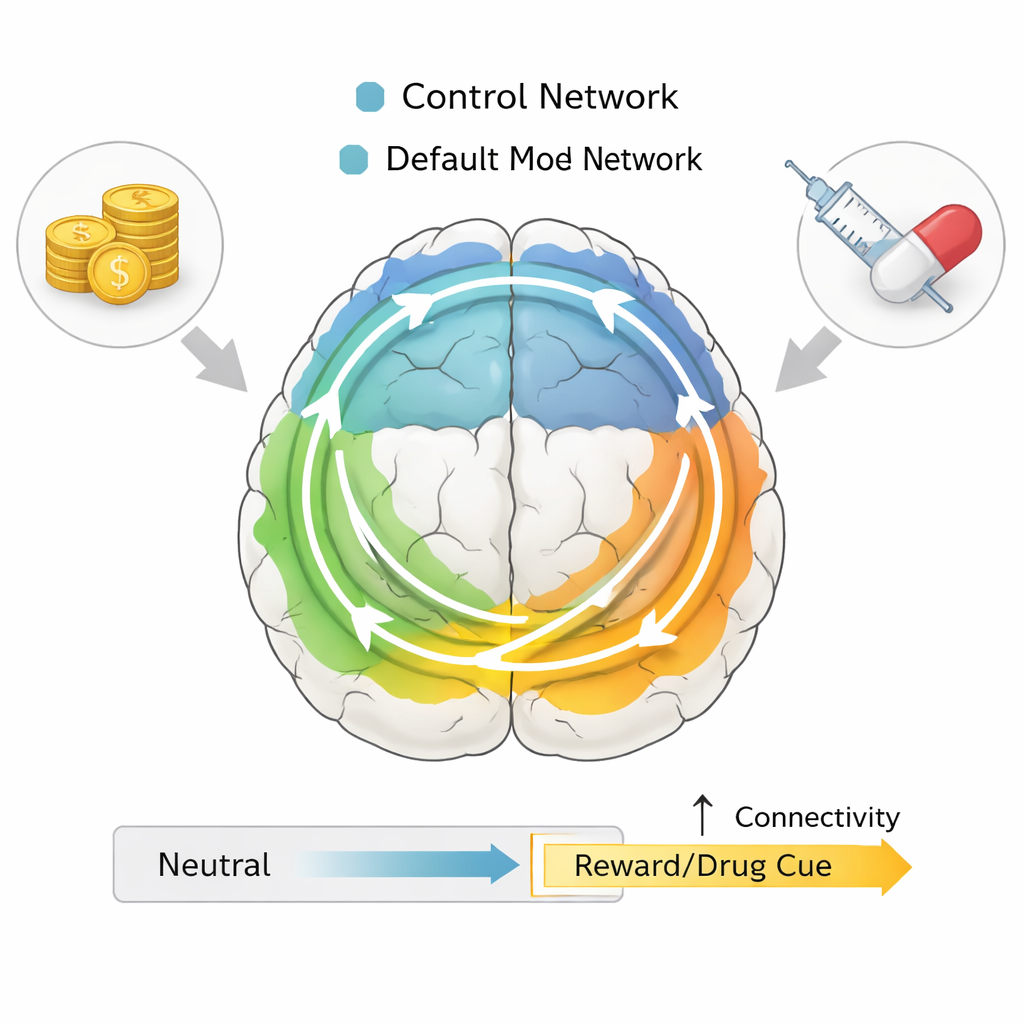
These task-specific changes suggest that people with opioid addiction may engage the brain differently when something important is at stake. During anticipation of monetary reward, their reward network became more tightly linked with self-focused and control regions, compared with neutral moments. A similar strengthening of connections appeared when they viewed drug-related images compared with neutral pictures. At the same time, healthy participants leaned more on visual, movement, and attention networks, consistent with a strategy focused on tracking targets and responses rather than on the emotional or motivational meaning of cues. In other words, the addicted brain seemed to tie reward, self-related thoughts, and control more tightly together exactly when rewards or drug cues appeared.
Shifting brain states over time
Beyond static connections, the team also examined how the brain’s networks took turns being “in charge” from moment to moment. During the money task, people with opioid use disorder spent more time in a default mode state and less time in a visual state than healthy volunteers. Their overall pattern of switching between states was also more complex and less predictable. This reinforces the idea that their brains may be more inwardly focused and less anchored to external sensory information during tasks that involve rewards. Interestingly, these differences in moment-to-moment dynamics were not seen during the drug-cue task, suggesting that context matters.
Chemical footprints and future treatments
The authors also asked whether the locations of these altered connections line up with where certain key brain receptors are found, using maps from previous PET imaging studies. They looked at μ-opioid receptors, which are directly affected by heroin and methadone, and dopamine D2 receptors, long linked to addiction and reward. They found a modest spatial overlap between areas rich in these receptors and regions showing connectivity differences, especially in the reward network, hinting that the chemical systems targeted by opioids may partly shape these network changes. For non-specialists, the take-home message is that severe opioid addiction is associated with a brain that is generally less well connected, but that becomes unusually tightly wired between reward, self-focused, and control systems when money or drug cues appear. Understanding these patterns could help design brain stimulation or other neuromodulation approaches that specifically target the miswired networks, with the long-term goal of reducing craving and making relapse less likely.
Citation: Kurtin, D.L., Herlinger, K., Hayes, A. et al. Task-related differences in network connectivity and dynamics in people with severe opioid use disorder compared with healthy controls. Transl Psychiatry 16, 111 (2026). https://doi.org/10.1038/s41398-026-03845-6
Keywords: opioid use disorder, brain networks, reward circuitry, functional connectivity, addiction neuroscience