Clear Sky Science · en
Dietary intake, quality, and assessment tools in individuals with problematic alcohol use: a scoping review and meta-analysis
Why Food Matters When Alcohol Becomes a Problem
When people think about alcohol use disorder, they usually picture its effects on the brain or liver, not on the dinner plate. Yet what and how people eat when they drink heavily can shape their health, their recovery, and even how strongly they crave alcohol. This article maps out what is known about the diets of people with serious alcohol problems, how good or poor their eating habits really are, and why traditional ways of judging nutrition may miss hidden risks.
Looking Across Decades of Research
The authors gathered and analyzed 41 studies from 16 countries, spanning more than fifty years, that reported what people with alcohol use disorder actually eat and drink. They separated findings into two broad phases: periods of heavy, ongoing drinking and periods of early abstinence, often during treatment. They also cataloged the tools used to measure diet, such as food diaries, recall interviews, and food frequency questionnaires. Despite this wide net, only a handful of studies looked at overall diet quality or whether diets matched national nutrition recommendations, revealing how fragmented this field of research still is.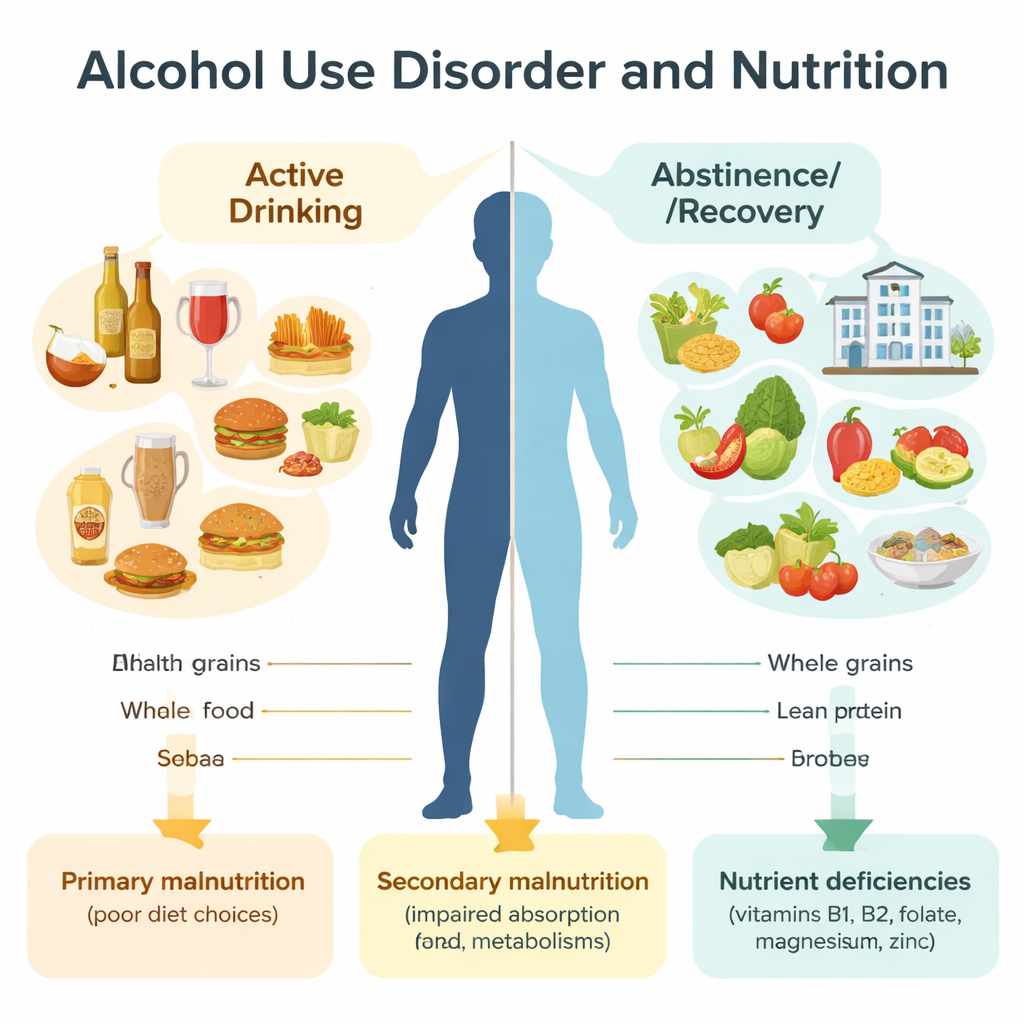
Calories, Alcohol, and the Illusion of “Normal” Nutrition
On paper, many people with alcohol use disorder appear to eat enough—or even more than enough—calories and major nutrients. During active drinking, the average person in these studies consumed about 2,900 calories per day, with roughly half of those calories coming from alcohol alone, the equivalent of around 15 standard drinks daily. Surprisingly, food and non-alcoholic drink intake stayed high instead of dropping to “make room” for alcohol. During abstinence, usually in structured inpatient settings, people still reported adequate calories and a fairly balanced mix of carbohydrates, protein, and fat, sometimes even exceeding the average intake seen in the general U.S. population.
Hidden Shortfalls Behind a Normal Body Weight
Despite these seemingly reassuring numbers, nutrient shortages were common. Average body mass index for people in these studies fell in the normal range, which might suggest they are not malnourished. Yet many had low intakes or low body levels of key vitamins and minerals, especially B vitamins (like thiamine and folate), magnesium, and zinc. Alcohol can damage the stomach and intestines, disrupt liver function, and increase the loss of nutrients in urine, leading to what is called “secondary malnutrition” even when calorie intake looks normal. These deficiencies can worsen heart and liver disease, weaken the immune system, and contribute to memory problems, mood issues, and severe brain disorders such as Wernicke–Korsakoff syndrome if left untreated.
What We Don’t Measure, We Don’t See
Another major message from this review is how poorly diet quality has been tracked in people with alcohol use disorder. Only four studies used formal scoring systems or national guidelines to rate how healthy overall eating patterns were. Early work tended to check single nutrients against recommended levels, while newer studies are starting to use tools like the Healthy Eating Index or the Nova system that flags heavy reliance on ultra-processed foods. Results so far hint that people actively drinking may eat more highly processed, nutrient-poor foods, whereas those in inpatient treatment can achieve better-quality diets when healthier options are provided. However, the lack of consistent methods and validated tools tailored to this population makes it hard to compare studies or draw firm conclusions.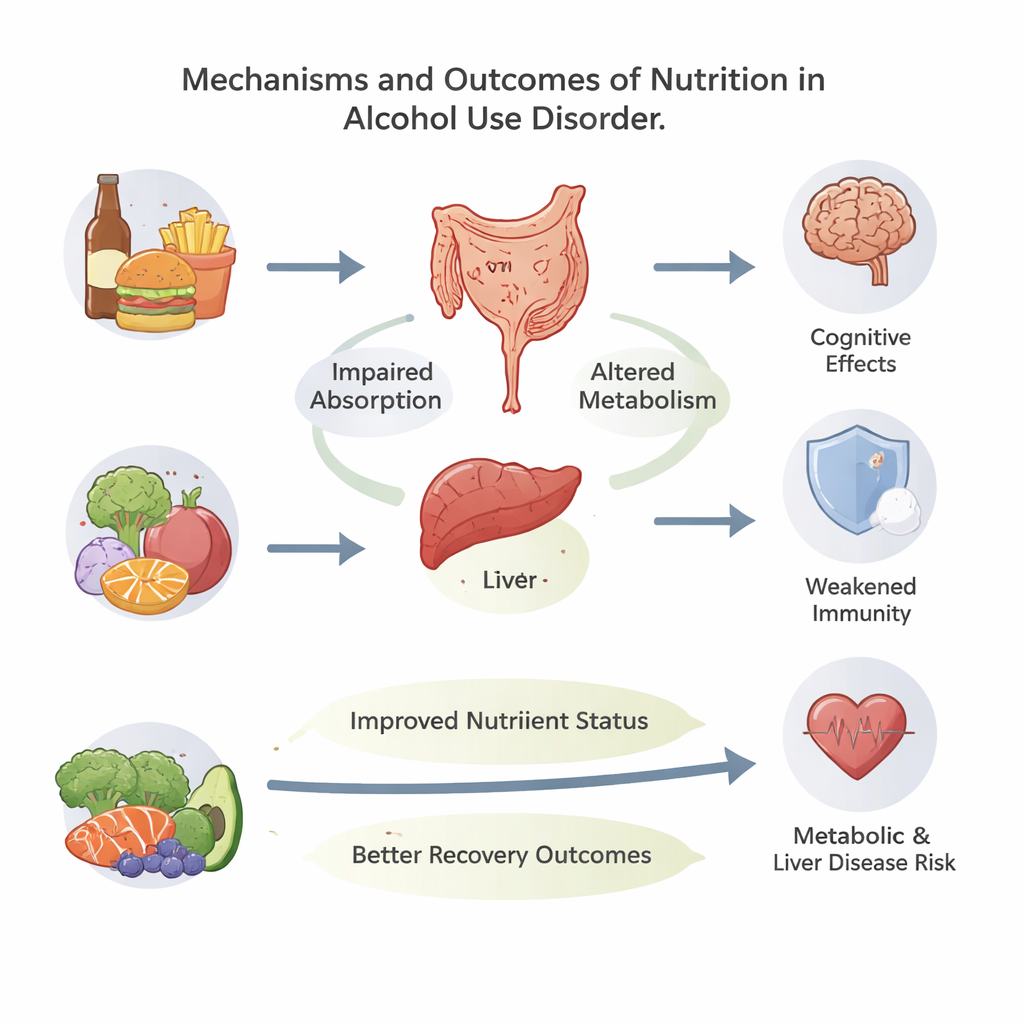
Bringing Nutrition Into Alcohol Treatment
For a layperson, the takeaway is that alcohol use disorder is not only a problem of drinking too much—it is also a problem of the body being starved of the right kinds of nutrients, even when weight and calorie counts look “fine.” Alcohol changes how the body handles food, so standard nutrition guidelines may not fully protect this group. The authors call for better, AUD-specific ways to measure diet, clearer reporting standards, and clinical guidelines that focus on the vitamins and minerals most likely to run low. Integrating nutrition science into addiction care—through better assessment, healthier food environments, and targeted supplementation—could improve health, ease symptoms, and support long-term recovery.
Citation: Barb, J.J., King, L.C., Nanda, S. et al. Dietary intake, quality, and assessment tools in individuals with problematic alcohol use: a scoping review and meta-analysis. Transl Psychiatry 16, 51 (2026). https://doi.org/10.1038/s41398-026-03842-9
Keywords: alcohol use disorder, nutrition, diet quality, micronutrient deficiency, malnutrition