Clear Sky Science · en
Brain texture alterations predict subtle visual perceptual dysfunctions in recent onset psychosis and clinical high-risk state
When the World Looks Subtly “Off”
For some people at the very early stages of serious mental illness, the world doesn’t just feel different—it looks different. Lines may seem wavy, faces slightly distorted, or lights painfully bright. These subtle visual glitches, called visual dysfunctions, are easy to miss in a doctor’s office but can signal vulnerability to psychosis. This study asks a striking question: can tiny changes in brain structure, too small to see with the naked eye on a scan, help us detect and understand these early visual problems across different psychiatric conditions?
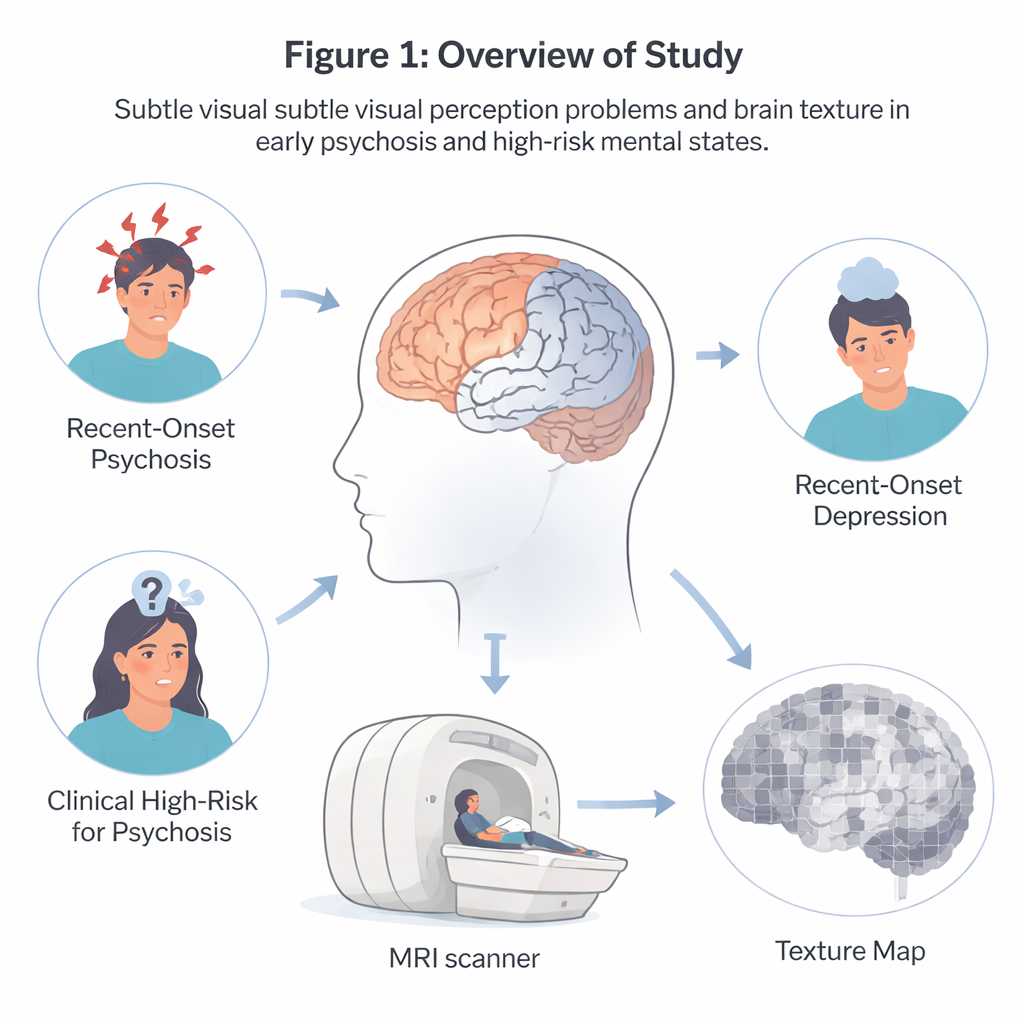
Seeing the Brain in Finer Detail
Traditional brain scans look for big, obvious changes, such as loss of brain tissue in certain regions. The researchers behind this work took a different approach. They treated MRI images more like photographs whose texture can be analyzed—whether an area looks smooth, patchy, regular, or irregular at a very fine scale. By measuring patterns of brightness across neighboring pixels, they built “texture maps” that capture how orderly or complex the brain tissue appears. This allowed them to look for hidden microstructural changes that might go unnoticed with standard volume-based methods.
Who Was Studied and Why
The team used data from a large European project called PRONIA, which follows young people aged 15 to 40 at early stages of mental illness. They focused on three groups: patients with recent-onset psychosis (people experiencing psychotic symptoms such as delusions or hallucinations for the first time), individuals at clinical high risk for psychosis (who have milder warning signs and may or may not develop a full psychotic disorder), and people with recent-onset depression. Within each group, some participants reported subtle visual distortions and some did not. Everyone had high-quality structural MRI scans. The core goal was to see whether brain texture features could distinguish those with visual problems from those without—and whether those patterns appeared similarly across the different diagnoses.
Patterns of Smoothness and Complexity
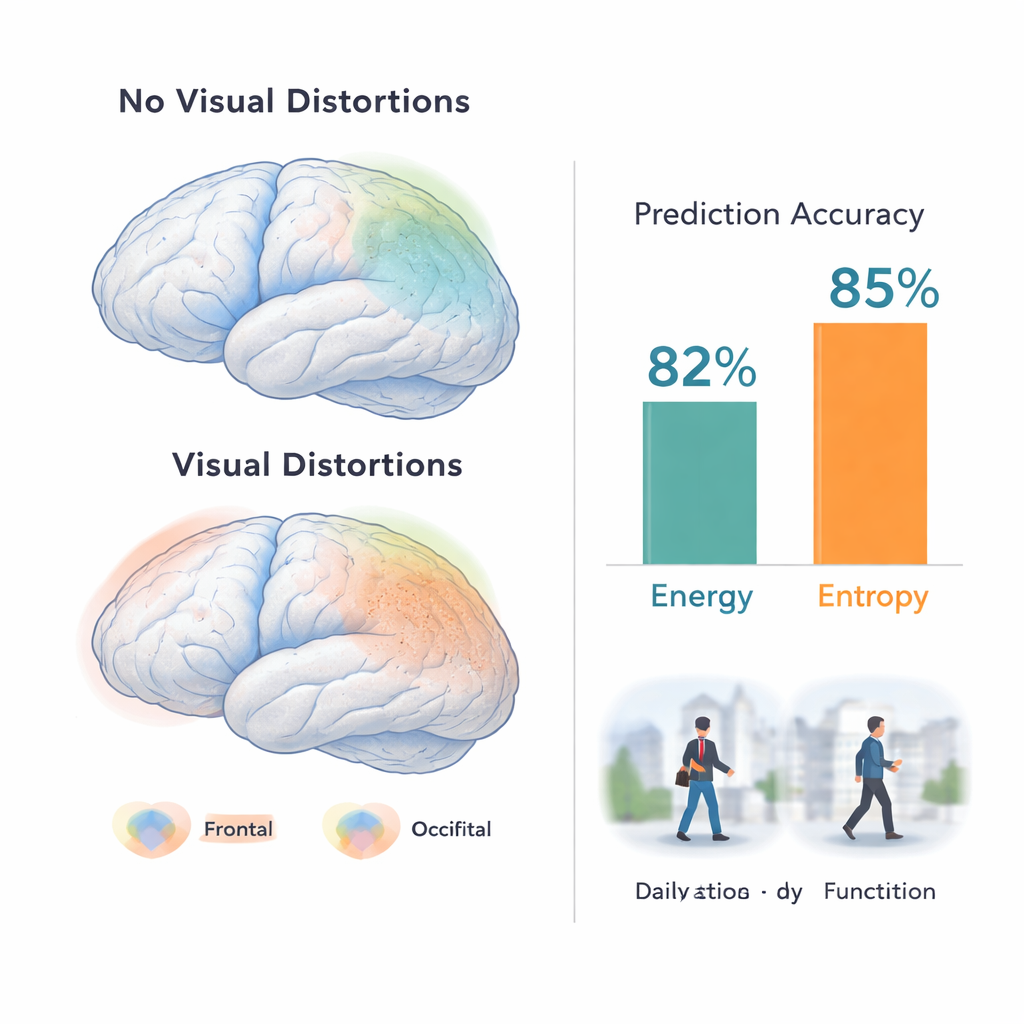
Using advanced machine-learning models, the researchers trained algorithms to classify participants as having visual dysfunctions or not, based only on their brain texture maps. In recent-onset psychosis, models that focused on “energy” (a measure of smoothness and regularity in the image) reached balanced accuracies above 80% in training and around 70% in an independent test group. In people at clinical high risk, models based on “entropy” (a measure of randomness and complexity) achieved comparable performance. The most informative brain areas included frontal and temporal lobes, as well as visual regions and deep structures involved in movement and integration of sensory information. Interestingly, when the models were tested in patients with recent-onset depression, they still picked up visual dysfunctions above chance level, suggesting that these brain patterns are not confined to classic psychotic disorders.
Linking Brain Patterns to Daily Life
Texture changes were not just mathematical curiosities; they were tied to how people felt and functioned. In psychosis and depression patients with visual problems, lower energy—meaning smoother but more abnormal brain texture—was associated with more severe positive symptoms (such as unusual thoughts), greater disorganization, and lower social and role functioning at baseline. It also predicted less favorable changes over nine months, particularly in disorganized thinking. In the high-risk group, higher entropy in certain clusters of patients related to how psychotic and depressive symptoms evolved over time, pointing to a more complex and heterogeneous brain–symptom relationship. Overall, people without visual distortions showed more varied and less clearly interpretable brain texture patterns than those with them.
What This Means for Early Detection
To a lay reader, the message is that tiny, fine-grained differences in how brain tissue is organized—too subtle to see on a standard MRI picture—can help flag who is experiencing disturbing visual distortions at the beginning of serious mental illness. These microtexture signatures differ between recent psychosis and high-risk states, but both relate to how symptoms and everyday functioning unfold over time. While this work is still at the proof-of-concept stage, it suggests that future brain-based tools might one day help clinicians identify people whose altered perception of the visual world marks a higher-risk, harder-to-recover pathway—and tailor monitoring and treatment before full-blown illness takes hold.
Citation: Lencer, R., Sprenger, A., Meyhöfer, I. et al. Brain texture alterations predict subtle visual perceptual dysfunctions in recent onset psychosis and clinical high-risk state. Transl Psychiatry 16, 113 (2026). https://doi.org/10.1038/s41398-026-03840-x
Keywords: visual perception, psychosis, brain MRI, radiomics, early detection