Clear Sky Science · en
Minocycline attenuates panicogenic responses in a CO2-induced panic attack model: a translational approach
Why this study matters for people with panic attacks
Panic attacks often seem to strike out of the blue, but for many people they are tightly linked to breathing and sensations of suffocation. This study explores why a simple burst of carbon dioxide (CO₂) in the air can reliably trigger panic, and tests whether an old antibiotic, minocycline, might calm this response in both mice and people with panic disorder. The work connects the immune system inside the brain to the terrifying experience of a panic attack and points to a potential new treatment strategy.
A gas that can spark fear
Doctors have long known that brief inhalation of air rich in CO₂ can provoke panic attacks in vulnerable people. As CO₂ rises, the body interprets this as a threat of suffocation and launches powerful defensive reactions: fast breathing, racing heart, and an overwhelming sense of dread. In mice, high CO₂ causes frantic escape behaviors such as running and jumping. The authors focus on a small blue-gray region deep in the brainstem called the locus coeruleus, or LC, which helps regulate breathing, attention, and the fight-or-flight response. They propose that special brain immune cells called microglia in the LC may sense internal disturbances like extra CO₂ and help drive panic responses.
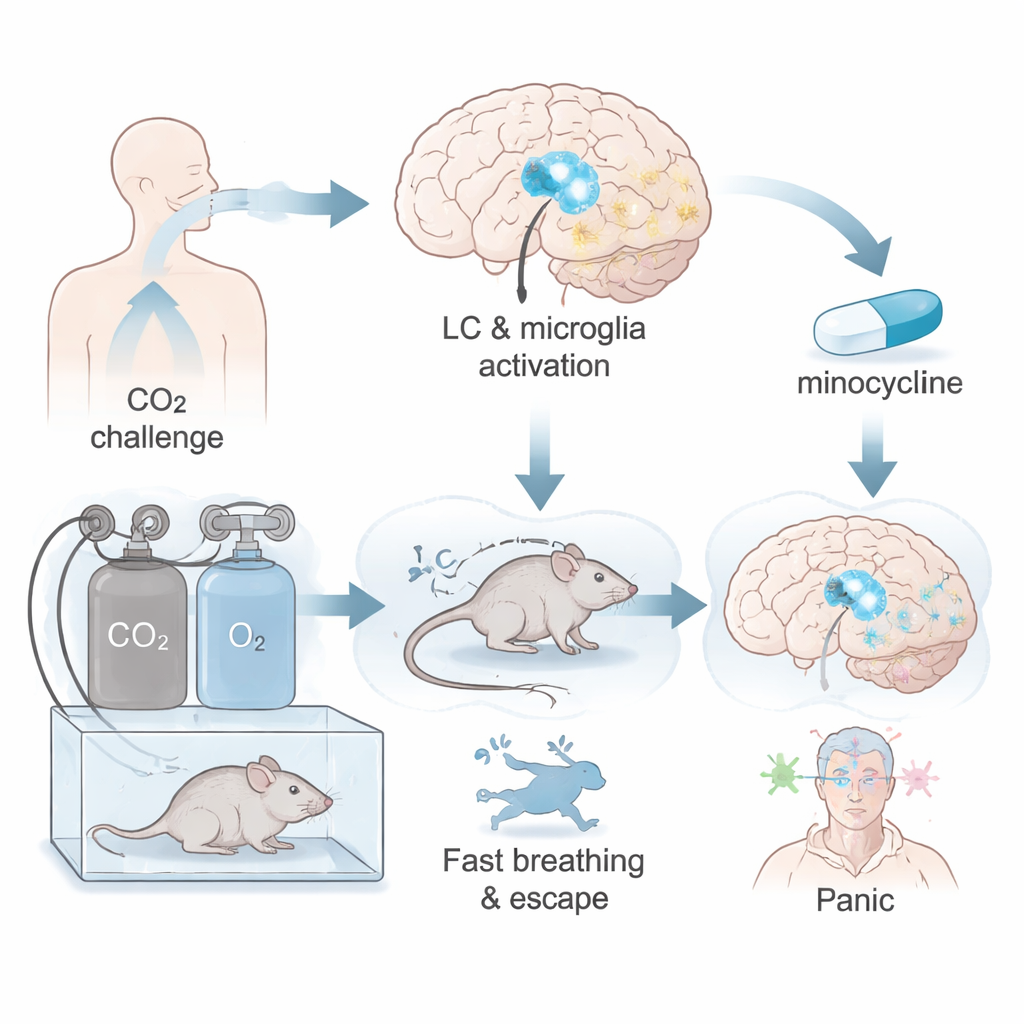
Microglia: the brain’s sentinels under CO₂ stress
To test this idea, the researchers exposed mice to air containing 20% CO₂, a strong “panicogenic” stimulus. They then examined microglia in the LC at different times after exposure. Six hours after breathing high CO₂, these cells had shifted from a resting, branched shape to a more rounded, activated form with fewer branches, lower density, and greater spacing between neighboring cells—hallmarks of a cell that has detected a threat and changed its behavior. At the same time, mice showed robust panic-like reactions: hyperventilation, frequent jumps, and running episodes, while standard movement in the cage remained normal. This suggests the response was not simple agitation but a specific escape pattern similar to a panic attack.
Testing minocycline and clonazepam in mice
The team next asked whether minocycline, known to dampen microglial activation, could blunt CO₂-driven panic-like behavior, and how it compared to clonazepam, a commonly prescribed anti-panic benzodiazepine. Mice received either minocycline or clonazepam for two weeks before the CO₂ challenge. Both drugs reduced the frantic escape reactions: clonazepam nearly abolished jumping and also reduced running, while minocycline cut the number of jumps by about 40% without making animals sluggish at baseline. Minocycline also slightly lowered normal breathing rate and appeared to moderate the tendency to overbreathe during CO₂ exposure, without compromising overall ventilation. Interestingly, despite its anti-inflammatory reputation, minocycline did not clearly change levels of several key immune signaling molecules in the LC or blood of mice, suggesting that its behavioral effects might depend on more subtle immune shifts or direct actions on nerve cells.
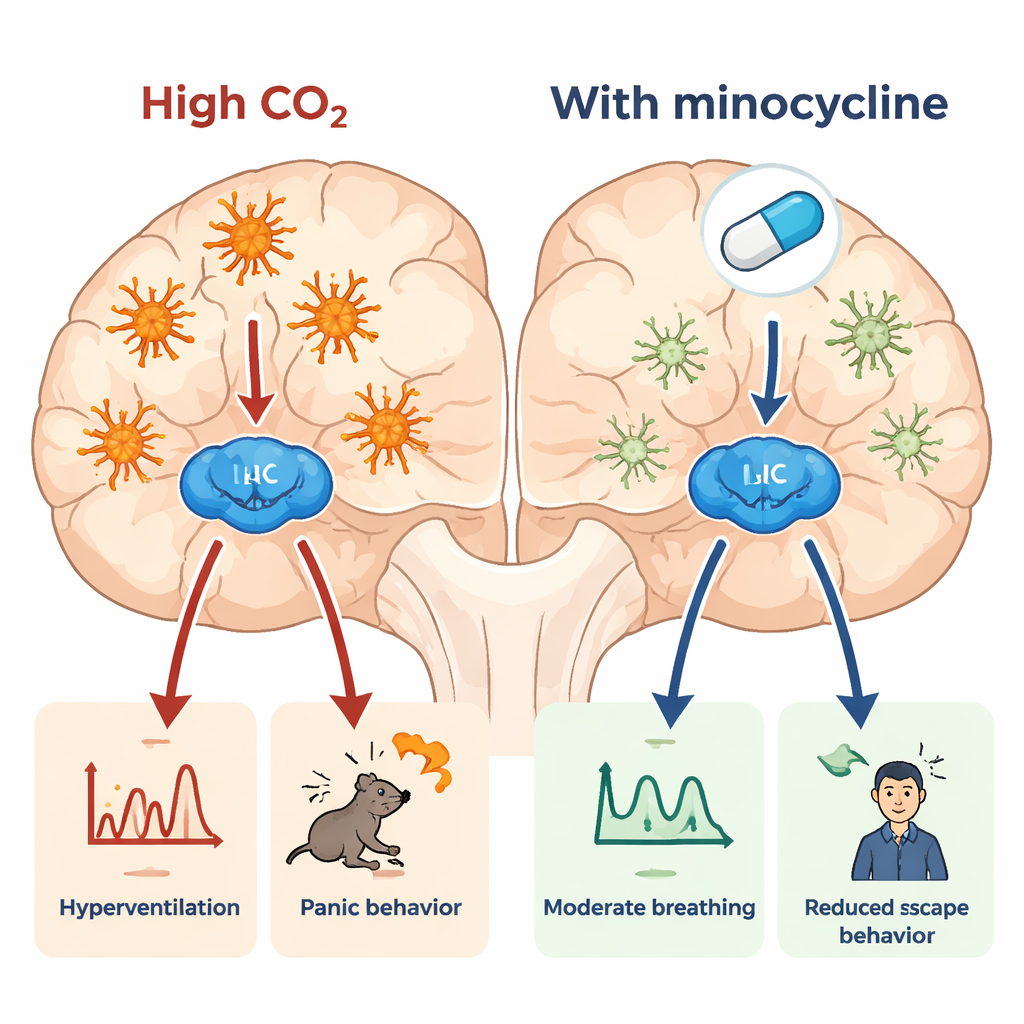
From mice to patients with panic disorder
In a companion clinical trial, 49 adults with panic disorder were randomly assigned to take either minocycline (100 mg/day) or clonazepam (0.5 mg/day) for seven days before undergoing a standard laboratory CO₂ inhalation test. Both groups showed meaningful reductions in the severity of CO₂-induced panic attacks and in overall panic and anxiety ratings, with no clear winner between the two drugs in this relatively small sample. However, their immune profiles in the blood told an interesting story. Before treatment, patients tended to show higher levels of a pro-inflammatory receptor marker (IL-2sRα) and lower levels of the anti-inflammatory molecule IL-10, consistent with previous hints of immune activation in panic disorder. After treatment, both minocycline and clonazepam lowered IL-2sRα and increased IL-10, but the changes were more pronounced in the minocycline group, which also showed shifts in other cytokines such as IL-6 and TNFα.
What this could mean for future treatments
Taken together, these findings suggest that high CO₂ not only activates nerve circuits that control breathing and fear, but also engages microglia in a key brainstem region, helping to shape panic-like responses. By calming microglia and possibly acting directly on neurons, minocycline reduced panic-related behavior in mice and attenuated CO₂-induced panic attacks in patients to a degree similar to clonazepam, while nudging the immune system toward a more anti-inflammatory profile. Although this antibiotic is not yet ready to replace standard treatments, and larger, longer trials are needed, the study opens the door to tackling panic disorder by targeting brain inflammation and microglial activity—offering a fresh angle on a condition that still leaves many patients only partially relieved by existing drugs.
Citation: de Oliveira, B.F.G., Quagliato, L.A., Frias, A.T. et al. Minocycline attenuates panicogenic responses in a CO2-induced panic attack model: a translational approach. Transl Psychiatry 16, 100 (2026). https://doi.org/10.1038/s41398-026-03836-7
Keywords: panic disorder, carbon dioxide challenge, microglia, minocycline, neuroinflammation