Clear Sky Science · en
Long-term risk of irritable bowel syndrome associated with adverse childhood and adulthood experiences: a large-scale prospective cohort study
When Life’s Hard Knocks Hurt the Gut
Irritable bowel syndrome (IBS) is more than a “sensitive stomach.” It brings recurring belly pain, bloating, and unpredictable trips to the bathroom that can disrupt work, relationships, and daily life. This study asks a powerful question that matters to many people: do difficult or traumatic experiences earlier in life, and later on as adults, make it more likely that someone will eventually develop IBS?
What Is IBS and Why Might Stress Matter?
IBS is a common disorder where the gut and brain do not communicate smoothly, leading to pain and changes in bowel habits. Around one in ten people worldwide are affected. Doctors know stress can trigger or worsen symptoms, but the long-term impact of serious adversity at different life stages has been less clear. The authors focused on “adverse experiences” such as neglect and abuse, which can leave lasting emotional and physical scars, and asked whether these events might raise the future risk of IBS.
Tracking Life Experiences in a Large Population
To explore this, researchers used data from more than 126,000 adults in the UK Biobank, a long-term health study in Britain. None of the participants had IBS when they were first enrolled, and their health was tracked for a median of 14.5 years. Participants later answered detailed online questions about difficult events in both childhood (before age 18) and adulthood. These covered five types of adversity: physical neglect, emotional neglect, sexual abuse, physical abuse, and emotional abuse. Using a statistical grouping method, the team sorted people into patterns such as “low adversity,” “high emotional neglect,” or “high abuse,” separately for childhood and adulthood.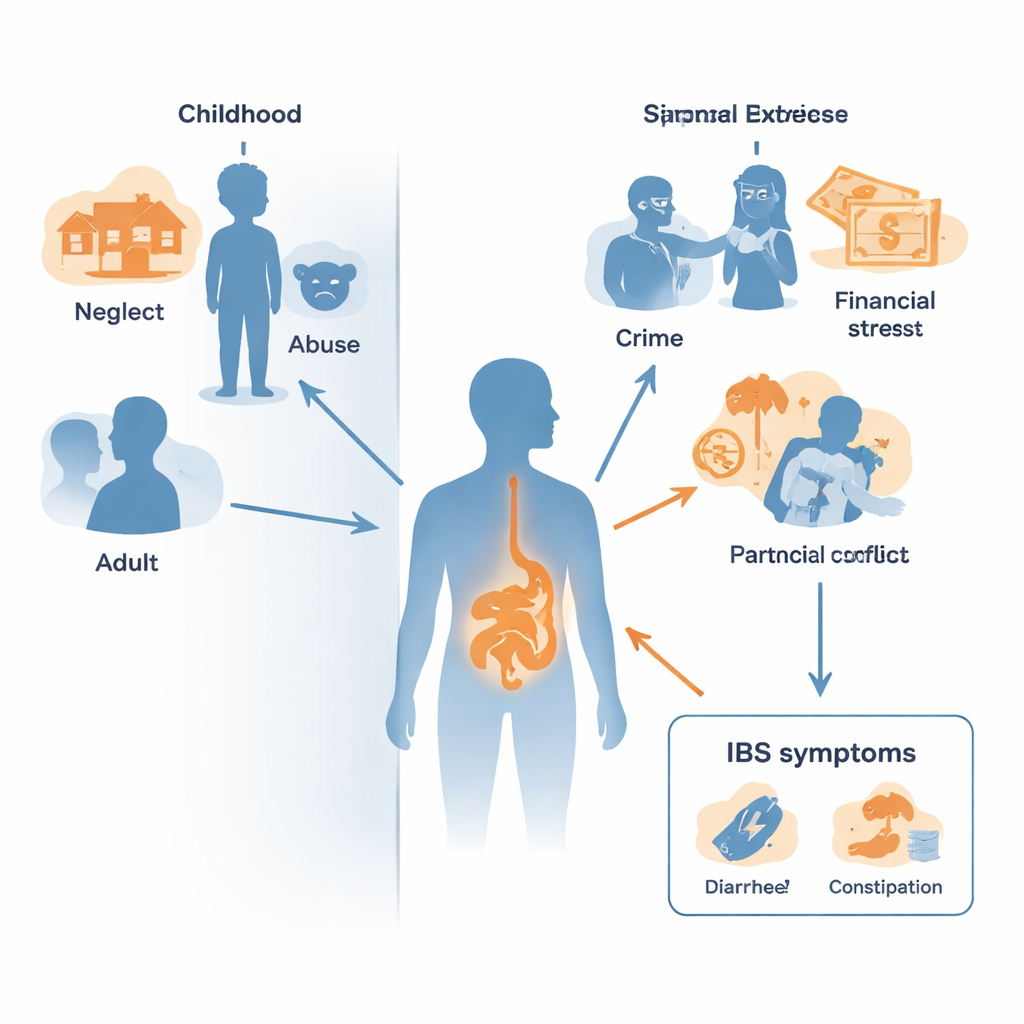
Childhood and Adult Hardship Both Raise IBS Risk
Over the follow-up period, about 2 percent of participants developed IBS. Compared with those who reported little or no childhood adversity, people who had grown up with strong emotional neglect had about a 38 percent higher risk of IBS, and those in the “high abuse” group had about a 64 percent higher risk. Adult experiences told a similar story: people reporting serious physical neglect in adulthood had about a one-third higher risk of IBS, and those with high levels of adult abuse had about a 55 percent higher risk, compared with adults with little or no adversity. In other words, both early-life and later-life hardships independently made IBS more likely to appear years down the line.
More Adversity, Higher Risk
The study also looked at how the number and type of adverse events added up. Each additional kind of serious negative experience in childhood or adulthood increased IBS risk by roughly 16–17 percent. People who had four or five types of childhood adversity had about double the risk of IBS compared with those who reported none; a similar, though slightly smaller, pattern appeared for adult experiences. All types of adversity—neglect and abuse, physical and emotional—were linked to higher IBS risk, with emotional neglect and emotional abuse in childhood and physical and emotional abuse in adulthood standing out as especially important.
When Troubles Pile Up Across a Lifetime
The most striking findings came from looking at childhood and adult experiences together. People who had both heavy abuse in childhood and serious abuse in adulthood had more than double the risk of IBS compared with those reporting low adversity at both stages. Combinations of emotional neglect in childhood with neglect or abuse in adulthood also raised risk substantially. The authors found that childhood and adult hardships did not just act separately; they appeared to work together in a way that amplified the overall impact on the gut. Although the study did not test mechanisms directly, prior research suggests that long-lasting changes in stress systems, brain development, gut bacteria, inflammation, and coping behaviors may all play a role.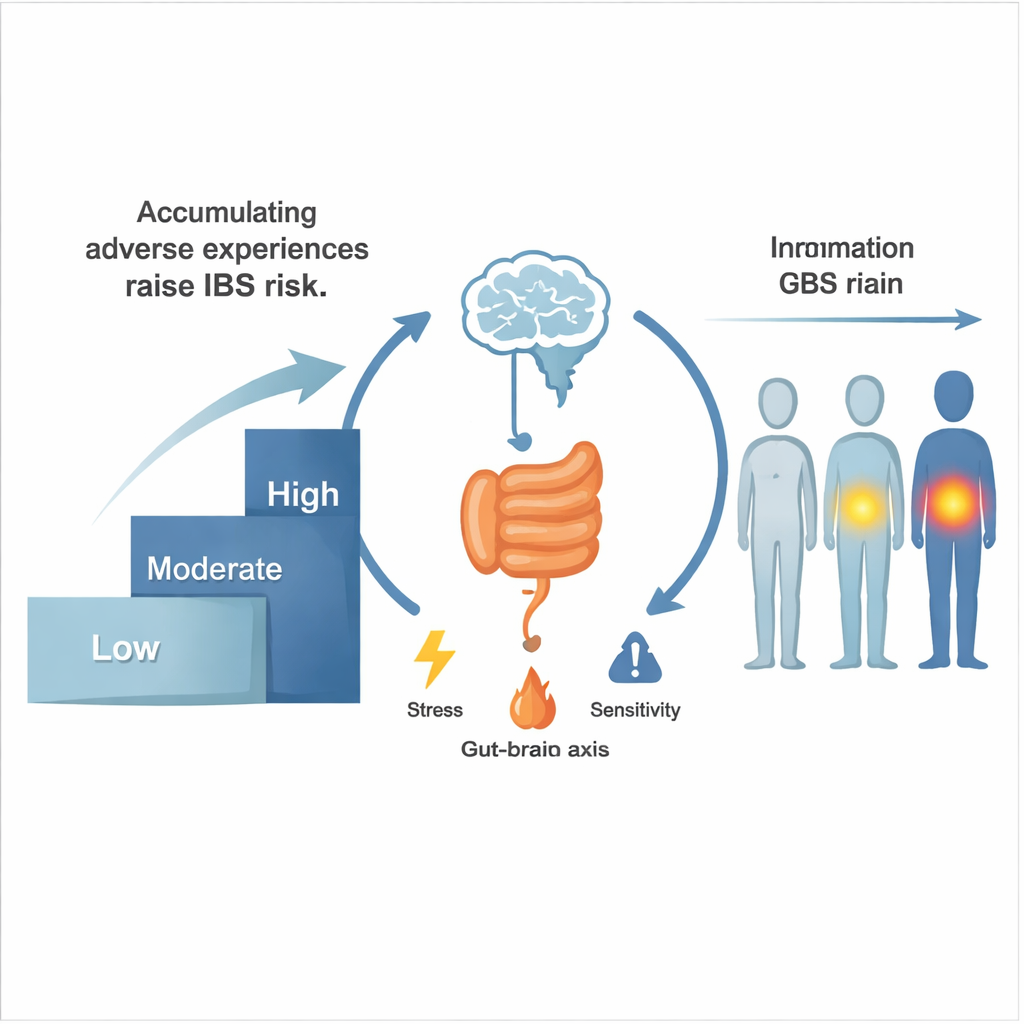
What This Means for People and for Care
For a lay reader, the main message is clear: serious emotional or physical hardship—whether in childhood, adulthood, or both—can leave an imprint that shows up later as IBS, not just as emotional distress. This does not mean IBS is “all in the head,” but that the brain and gut are tightly linked, and life experiences shape both. The authors argue that health care should pay attention to a person’s whole life story, not only their current symptoms. Screening for past adversity in people with IBS—and offering psychological support as well as digestive care—could help identify those at highest risk and open the door to more effective, compassionate treatment.
Citation: Zhou, Y., Liu, S., Xie, S. et al. Long-term risk of irritable bowel syndrome associated with adverse childhood and adulthood experiences: a large-scale prospective cohort study. Transl Psychiatry 16, 70 (2026). https://doi.org/10.1038/s41398-026-03833-w
Keywords: irritable bowel syndrome, adverse childhood experiences, trauma and gut health, stress and digestion, gut–brain axis