Clear Sky Science · en
Exploring the intricate interplay between metabolic abnormalities and multidimensional cognitive impairment in stable schizophrenia patients
Why Heart Health Matters for the Mind
People with schizophrenia often struggle not only with hallucinations or delusions, but also with everyday thinking skills like memory, concentration, and mental speed. At the same time, they face high rates of physical health problems such as high blood pressure and abnormal cholesterol. This study asks a question that matters to families, clinicians, and patients alike: can treating these “body” problems also protect the mind? By examining hundreds of stable patients across ten hospitals in China, the researchers map out how specific metabolic problems may quietly shape thinking ability and day-to-day functioning.
A Large-Scale Look at Brain and Body
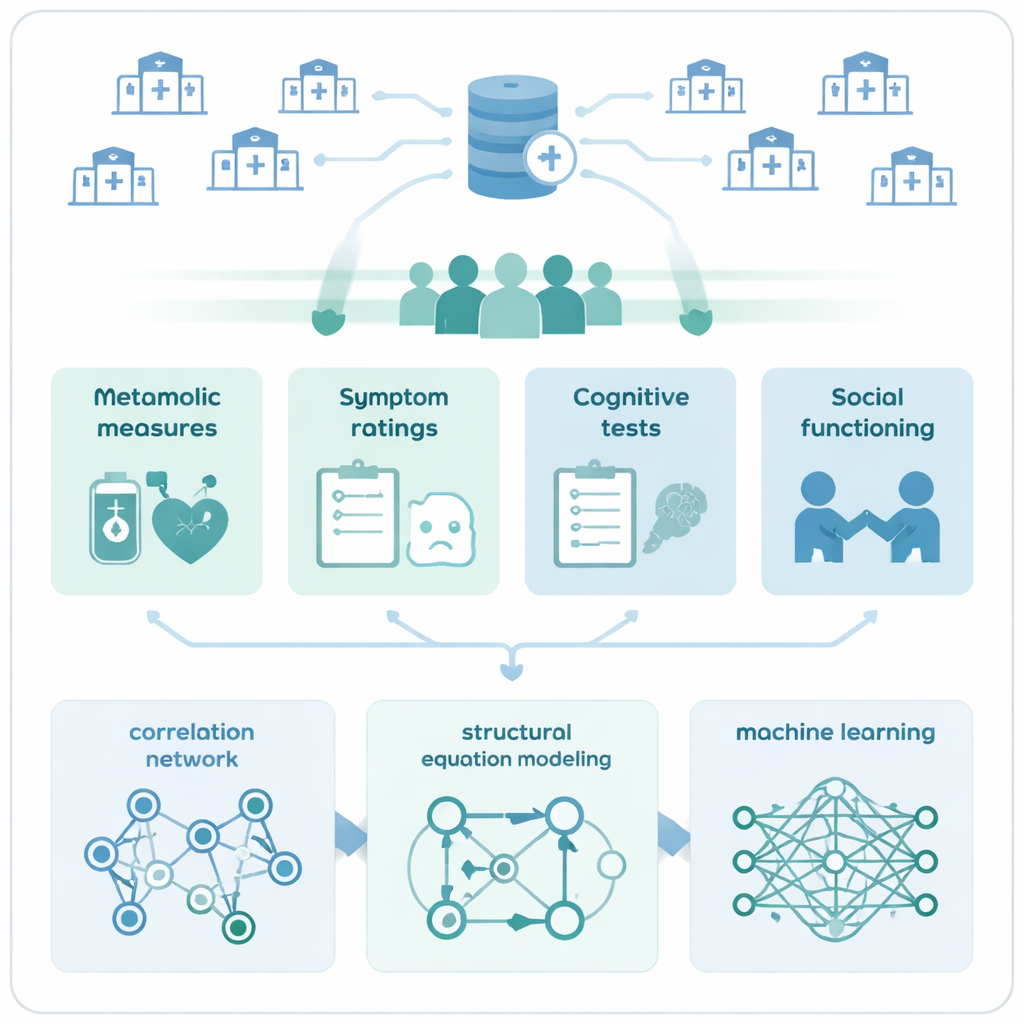
To explore these links, the team recruited 727 adults with stable schizophrenia from ten psychiatric hospitals. All participants were on steady doses of medication and were not in an acute crisis, making it easier to focus on longer-term patterns rather than short-term symptom flare-ups. Each person completed a brief, culturally adapted set of thinking tests that measured mental speed, attention, and short-term memory. They also answered questions about their physical and emotional health. At the same time, doctors collected detailed information on blood pressure, blood sugar, weight, and blood fats such as cholesterol and triglycerides—key ingredients of what doctors call metabolic syndrome.
Which Metabolic Problems Matter Most?
Past research often treated metabolic syndrome as a single bundle, which made it hard to see whether all its pieces were equally important for thinking. This study took a more fine-grained approach, separating out high blood pressure, abnormal blood fats, high blood sugar, and obesity. The results showed that not all components were created equal. High blood pressure and abnormal blood fats—especially what doctors call dyslipidemia—were most clearly linked to poorer performance on several thinking tests. Patients with high blood pressure tended to have slower mental processing, weaker attention, and worse working memory. Those with abnormal blood fats also showed differences in mood and thinking, although in some cases they performed unexpectedly better on certain attention and memory tasks, highlighting how complex these relationships can be.
Mapping Hidden Connections in Symptoms and Thinking
The researchers then used modern network methods to visualize how symptoms, thinking skills, social functioning, and metabolic problems were intertwined. They compared patients with at least two metabolic problems to those without. In people with more metabolic difficulties, the web of connections between thinking skills and social functioning looked sparser, suggesting that physical health issues might be overshadowing or cutting off some of the usual links between cognition and everyday life. Across all patients, one test that measures how quickly and accurately people match symbols—a marker of information processing speed—stood out as a central hub, strongly tied to many other abilities. This implies that mental speed may be a key lever for improving overall functioning.
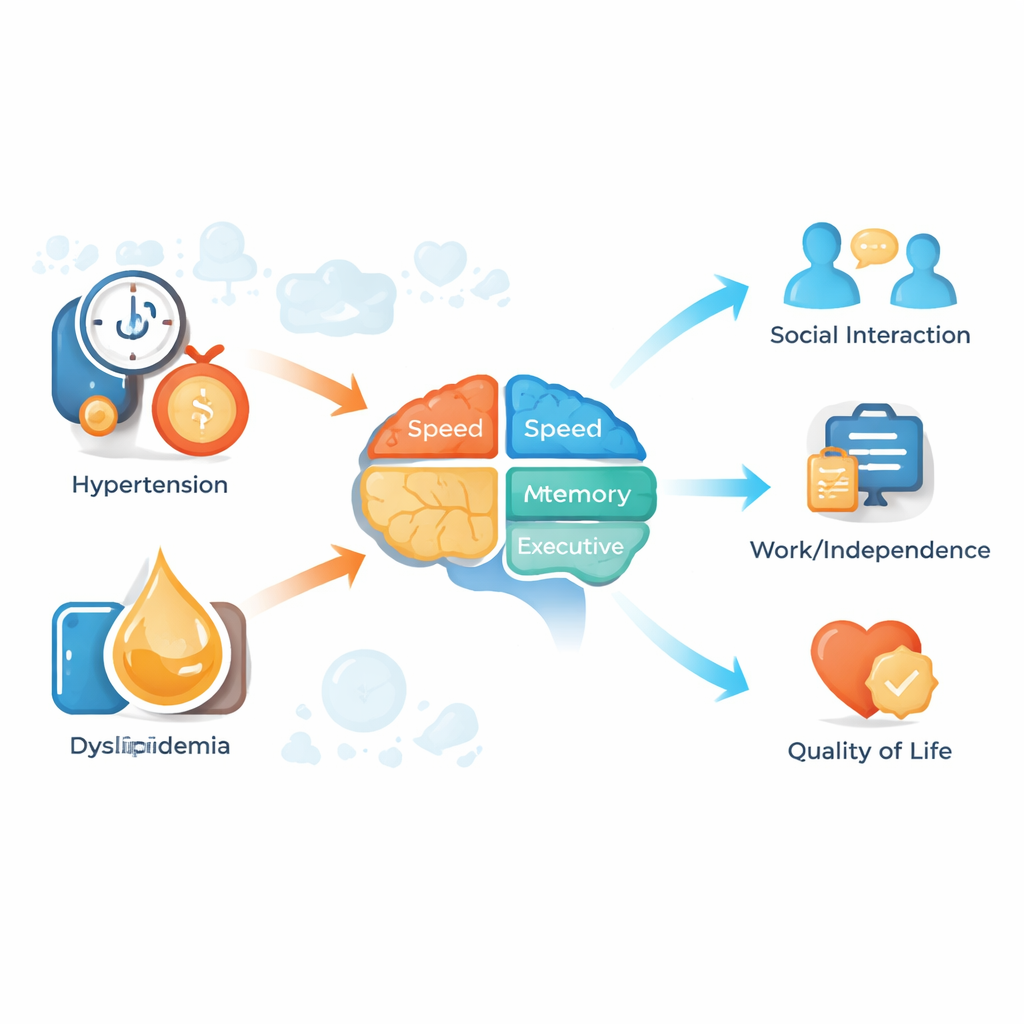
How Blood Pressure and Blood Fats Bridge Mind and Body
Using a technique called structural equation modeling, the team asked whether metabolic problems might act as a bridge between psychiatric symptoms and thinking skills. They found that high blood pressure and abnormal blood fats partly explained how symptom severity translated into cognitive difficulties. In other words, more severe symptoms were linked to worse metabolic health, which in turn predicted poorer performance on tests of speed, attention, and memory. To check how powerful these physical measures were, the authors also trained modern machine learning models to predict thinking test scores from symptom ratings and metabolic data. A transformer-based model—similar in spirit to systems used in language technology—captured these patterns particularly well, suggesting that metabolic indicators carry real predictive value for cognitive outcomes.
What This Means for Everyday Care
For people living with schizophrenia and those who care for them, this work carries a hopeful but practical message. It suggests that monitoring and treating high blood pressure and abnormal blood fats is not just about preventing heart attacks and strokes; it may also help preserve thinking skills that are vital for living independently, holding a job, and maintaining relationships. Rather than viewing mental and physical health as separate worlds, the study argues for integrated care that targets both. While more long-term research is needed to prove cause and effect, the findings point toward a future in which controlling blood pressure and improving metabolic health become central tools for protecting the mind in schizophrenia.
Citation: Wang, X., Dang, J., Yu, X. et al. Exploring the intricate interplay between metabolic abnormalities and multidimensional cognitive impairment in stable schizophrenia patients. Transl Psychiatry 16, 105 (2026). https://doi.org/10.1038/s41398-026-03820-1
Keywords: schizophrenia, cognitive impairment, metabolic syndrome, hypertension, dyslipidemia