Clear Sky Science · en
Immediate and long-term effects of orbitofrontal cortex stimulation on EEG microstates in schizophrenia
Why tuning brain rhythms could help treat schizophrenia
Schizophrenia can be deeply disabling, and many people do not respond well to standard medications or are overwhelmed by their side effects. Scientists are therefore searching for gentler ways to nudge faulty brain circuits back toward healthy function. This study explores whether a noninvasive brain stimulation technique, paired with sensitive brain‑wave measurements, can both improve symptoms and reveal early signs of who is most likely to benefit.
Noninvasive pulses to a key decision-making hub
The researchers focused on a small region just above the eyes called the orbitofrontal cortex, which helps us weigh rewards, make decisions, and regulate emotions. They used repetitive transcranial magnetic stimulation (rTMS), a method that delivers brief magnetic pulses through the scalp, to gently alter the activity of this region without surgery or drugs. Eighty‑seven people experiencing their first episode of schizophrenia were randomly assigned to receive either real rTMS to the right orbitofrontal cortex or a sham procedure that mimicked the experience without effectively stimulating the brain. Everyone received 20 daily sessions, while continuing on standard antipsychotic medication. A separate group of 51 healthy volunteers received a single real rTMS session to allow the team to compare how healthy and affected brains respond.
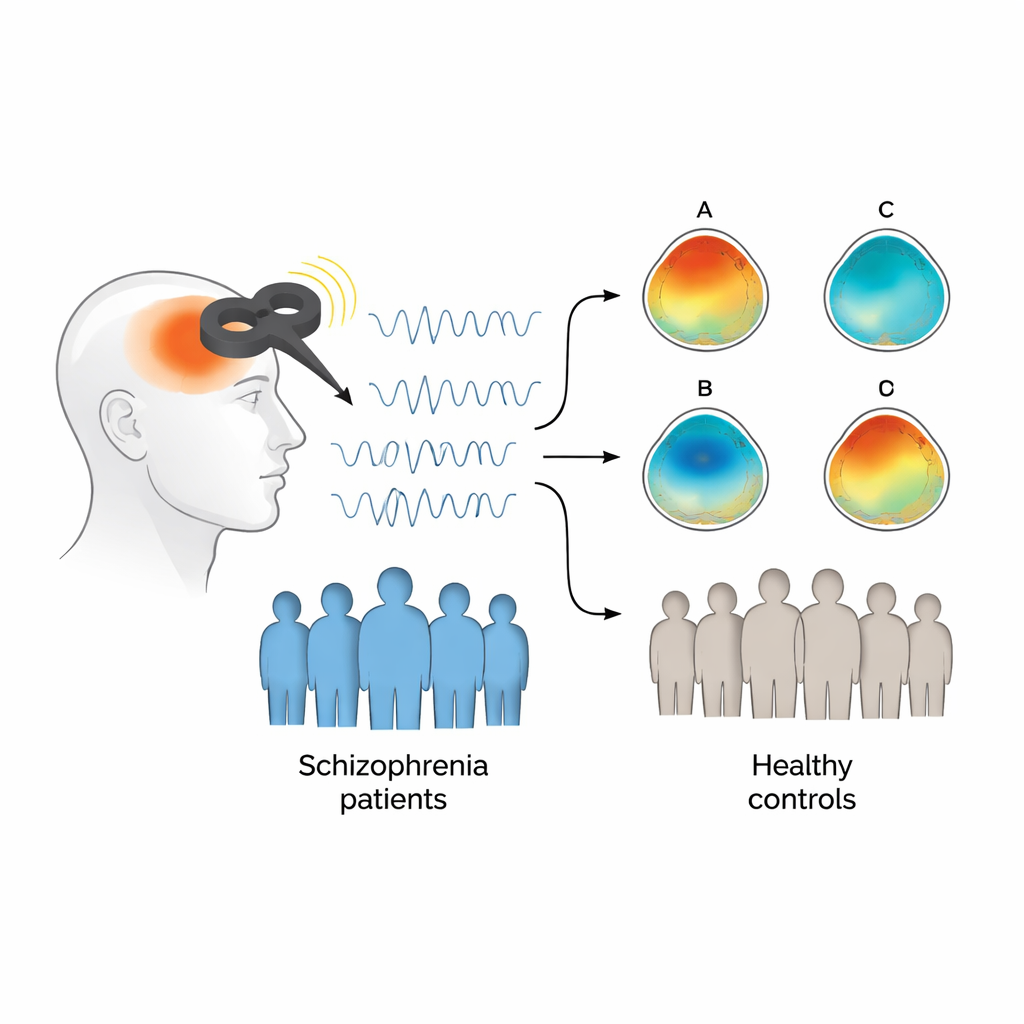
Reading the brain’s fleeting “states” from EEG
To track how brain activity changed, the team recorded resting‑state electroencephalography (EEG), which measures tiny electrical signals at the scalp. Rather than focusing on overall power or simple rhythms, they used a method called microstate analysis that looks at how the brain flips through brief but stable patterns of activity, each lasting only a fraction of a second. Across many studies, four recurring patterns, labeled A through D, have been linked to different large‑scale networks, including systems for detecting important events and shifting attention. Earlier work has shown that people with schizophrenia tend to spend more time in one pattern, called microstate C, and less time in another, microstate D, suggesting an imbalance between networks that flag salient events and those that support controlled attention.
Immediate changes after a single stimulation session
EEG recordings were taken from patients before treatment, immediately after the first rTMS session, and again after the 20‑day course. Healthy volunteers were scanned before and after their single session. At the outset, patients showed the expected imbalance: they spent more time in microstate C and had shorter episodes of microstate D than healthy individuals. After just one real stimulation session, both patients and healthy volunteers showed a drop in how often microstate C appeared. In patients, this reduction was seen only in the real‑stimulation group; those receiving sham treatment showed no meaningful change. The likelihood of the brain jumping from other patterns into microstate C also decreased, while switches toward microstate D became more common, hinting at a rapid rebalancing of brain networks.
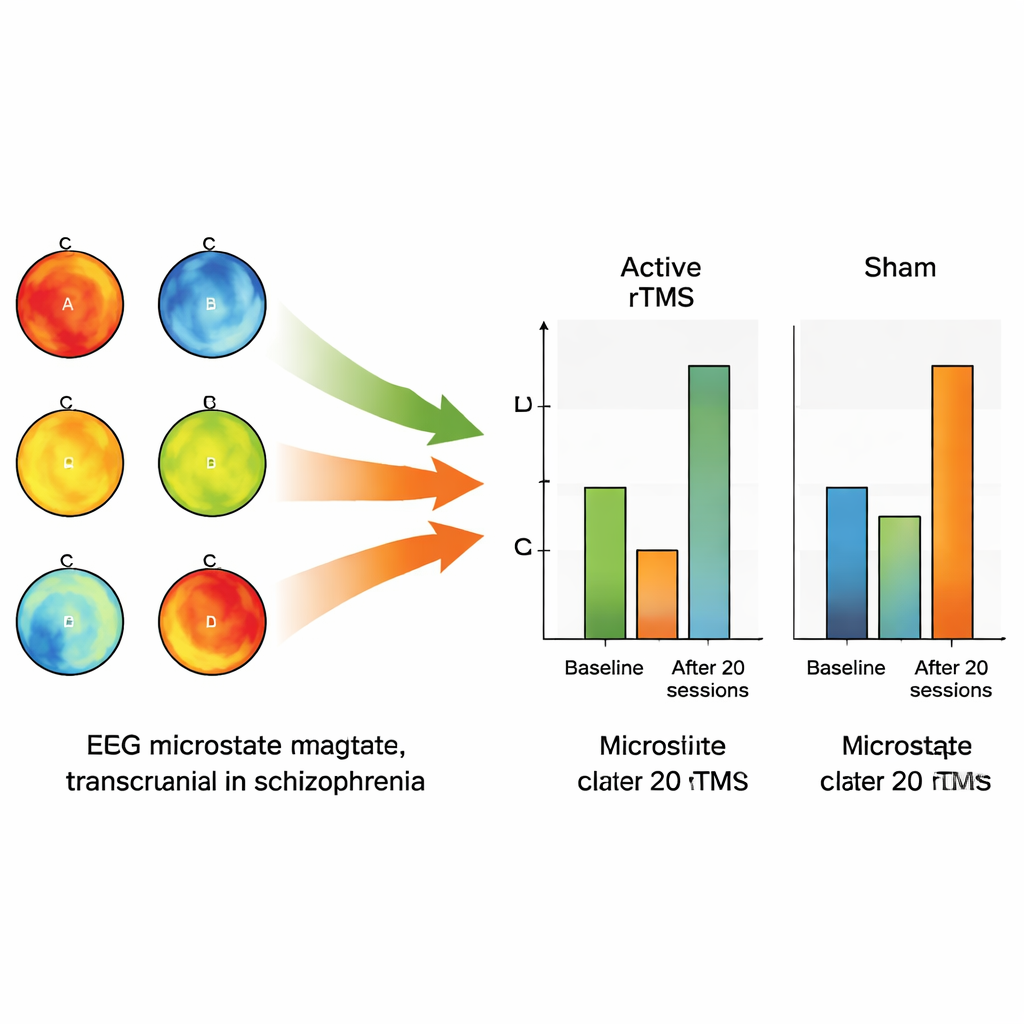
Lasting shifts in brain patterns and links to symptom relief
After 20 sessions, patients who had received real orbitofrontal stimulation showed sustained changes. They spent less overall time in microstate C and more time in microstate D, and transitions into C from other patterns became less frequent, while transitions into D became more common. These shifts were not seen in the sham group, which showed only limited improvement in microstate D that may have been driven by medication alone. Clinically, those receiving real rTMS had a much larger reduction in their symptom scores than the sham group. When the researchers looked more closely, they found that patients who went on to show strong clinical improvement were the ones who had the biggest immediate drop in microstate C right after the first stimulation session, suggesting that early EEG changes may foreshadow who will benefit most.
What this could mean for future treatment
For non‑specialists, the take‑home message is that gentle magnetic pulses to a decision‑making region above the eyes can both ease schizophrenia symptoms and visibly reshape how the brain’s activity patterns unfold over milliseconds. In particular, the treatment appears to dampen an overactive “salience” pattern (microstate C) and strengthen an attention‑related pattern (microstate D), nudging brain dynamics closer to what is seen in healthy people. Just as important, the very first stimulation session already carries clues: a strong early shift in these fast brain states may signal that a person is on track to respond well over the coming weeks. If confirmed in larger studies, this approach could help personalize brain‑stimulation therapies, quickly identifying those most likely to benefit while sparing others from weeks of ineffective treatment.
Citation: Zhang, K., Hu, Q., Zhang, Y. et al. Immediate and long-term effects of orbitofrontal cortex stimulation on EEG microstates in schizophrenia. Transl Psychiatry 16, 56 (2026). https://doi.org/10.1038/s41398-026-03810-3
Keywords: schizophrenia, brain stimulation, EEG microstates, orbitofrontal cortex, rTMS