Clear Sky Science · en
Bladder management for adults with spinal cord injury in the acute hospital setting: A retrospective study
Why hospital bladder care after spinal cord injury matters
When someone experiences a spinal cord injury, the first days and weeks in the hospital are filled with visible concerns like surgery, breathing, and movement. Less visible—but just as crucial—is how the bladder is managed. Poor bladder control can quietly damage the kidneys, trigger dangerous spikes in blood pressure, and lengthen hospital stays. This study looks at how hospitals actually manage bladder care for adults with spinal cord injury and how those choices relate to how long patients remain in the hospital.
Different ways to help the bladder drain
After a spinal cord injury, the nerves that tell the bladder when to fill and empty may no longer work properly. Doctors can support bladder emptying in several ways. One common method is an indwelling urinary catheter, a tube that stays in the bladder and continuously drains urine into a bag. Another approach, called clean intermittent catheterization, uses a catheter only a few times a day to empty the bladder and then removes it, allowing the bladder to fill in between. Some patients use both methods at different points during a single hospital stay, and others are able to urinate on their own without any catheter. Each method has trade-offs, including comfort, infection risk, and practicality when a patient is very sick.
How the researchers studied real-world hospital care
The research team reviewed electronic health records from a large U.S. health system, looking at adults with spinal cord injury admitted to acute-care hospitals between late 2021 and late 2023. They included 1,169 people and 1,652 hospital admissions. For every admission, they used recorded urine outputs and doctors’ orders to determine how the bladder was managed: indwelling catheter only, intermittent catheter only, both methods during the stay, or no catheter at all. They then measured how long each patient stayed in the hospital and used statistical models to see how bladder management and type of spinal cord injury—neck (cervical) versus lower back (thoracolumbar)—were linked to length of stay.
What hospitals are doing now
Nearly half of all admissions in this study—about 50 percent—did not use a catheter at all, suggesting many patients could still urinate without a tube or used other noninvasive strategies. About 19 percent of admissions relied only on an indwelling catheter, while smaller portions used intermittent catheterization alone or a mix of both methods. Most patients, more than 80 percent, stayed on a single bladder strategy for their entire hospital stay. When catheters were used, indwelling catheters typically stayed in place for around five days, and intermittent catheter stretches tended to last only a few days at a time. In the group that used both indwelling and intermittent methods, many patients had more than one trial of intermittent catheterization, suggesting that teams were testing whether a less invasive approach would work.
Bladder choices and extra days in the hospital
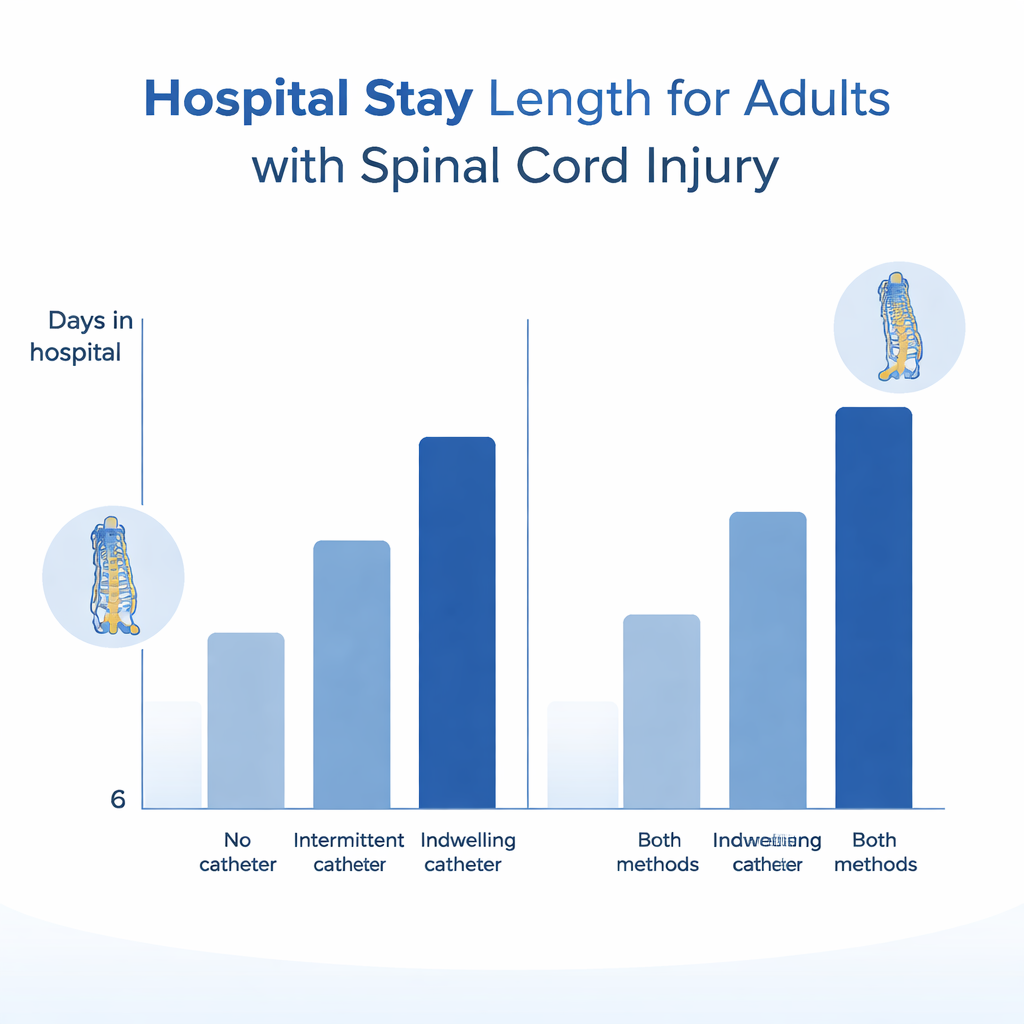
Bladder management was closely tied to how long patients remained in the hospital. Overall, the average stay was about nine days. After accounting for age, sex, race, type of injury, and repeat admissions, people managed only with an indwelling catheter stayed in the hospital about three days longer than those with no catheter. Those who used both indwelling and intermittent catheters had the longest stays—nearly 15 extra days compared with patients without catheters. Among this mixed-method group, patients with neck-level injuries had especially long hospital stays, adding roughly 11 more days than patients with lower-back injuries who used the same bladder strategies. These patterns likely reflect both the medical complexity of these patients and the challenges of safely changing bladder methods during recovery.
What this means for patients and care teams
For people with spinal cord injury and their families, this study shows that how the bladder is managed in the hospital is more than a comfort issue—it is closely linked to how long they remain in the hospital and may flag patients with more complicated recoveries. While many patients can avoid catheters, careful planning is needed when catheters are used or when switching between methods, especially for those with neck injuries. The authors suggest that clearer guidance, better teamwork among specialists, and decision-support tools could help hospitals choose and adjust bladder strategies more confidently. In simple terms, thoughtful bladder care early on may help prevent complications and support safer, possibly shorter hospital stays for people living with spinal cord injury.
Citation: Hon, E., He, M., Xu, L. et al. Bladder management for adults with spinal cord injury in the acute hospital setting: A retrospective study. Spinal Cord Ser Cases 12, 4 (2026). https://doi.org/10.1038/s41394-026-00730-8
Keywords: spinal cord injury, bladder management, urinary catheter, neurogenic bladder, hospital length of stay