Clear Sky Science · en
Towards accurate malnutrition identification in individuals with Spinal Cord Injury: a qualitative investigation
Why nutrition is tricky after spinal cord injury
For people living with a spinal cord injury, eating well is about much more than counting calories. Their bodies change in ways that can make it hard to tell who is truly undernourished, who is getting too much, and who is doing fine. This study listened closely to dietitians around the world to understand how they identify malnutrition in people with spinal cord injury, what gets in the way, and how care could be improved so that fewer patients slip through the cracks.
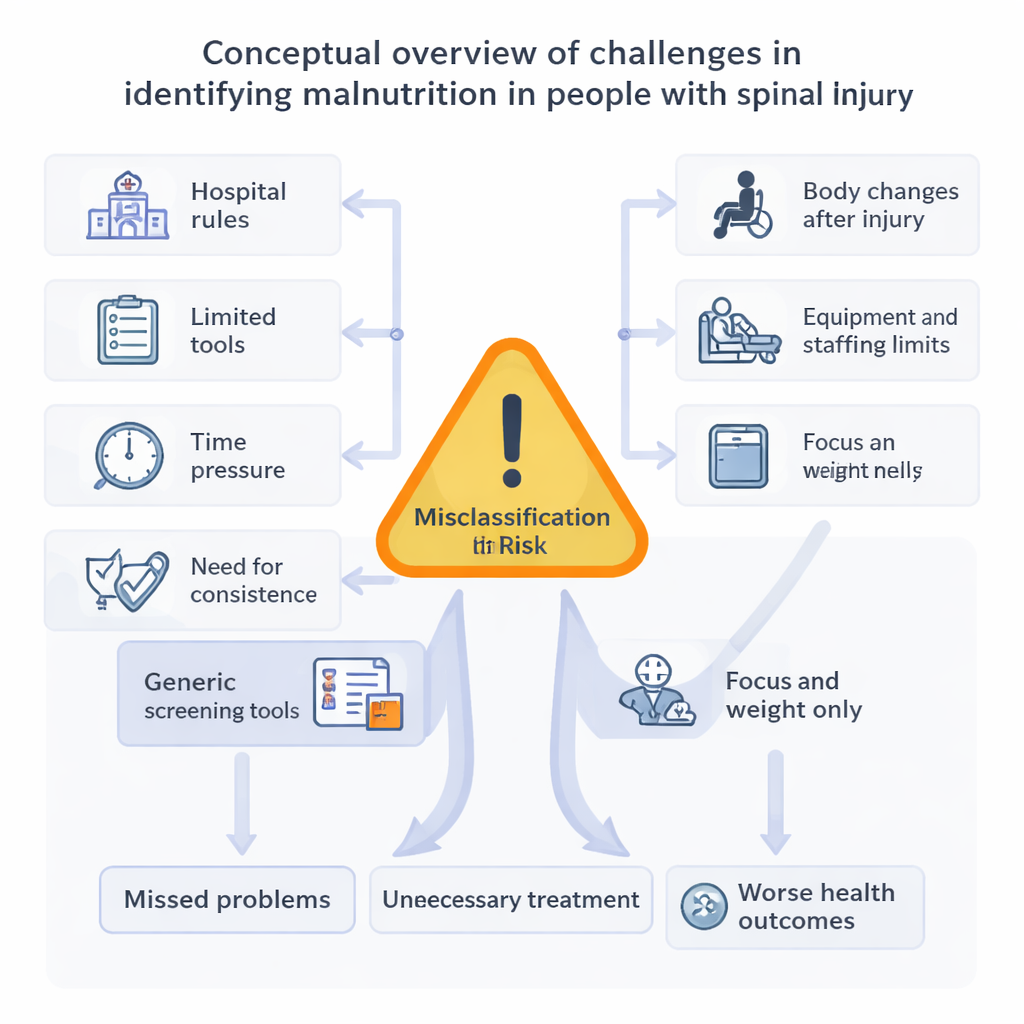
How dietitians actually work in real clinics
The researchers interviewed 12 experienced dietitians from hospitals, rehabilitation units, and community services across six countries. These clinicians described a common reality: they mostly use general hospital screening tools, such as brief checklists about weight loss and appetite, because those tools are built into hospital policy and electronic systems. Yet many felt these tools were a poor fit for people with spinal cord injury. They worried that the tools overemphasize body weight and do not capture key issues like level of paralysis, skin problems, or mental health. Some dietitians tried to compensate by relying on their own observations and more detailed questions, but this made practice highly variable from one clinician or service to another.
Everyday obstacles to getting reliable information
Dietitians also described practical hurdles that would surprise many outsiders. Getting a simple body weight can be difficult when patients have unstable spines, need hoists or special scales, or are often off the ward for surgery or therapy. Equipment may be missing, broken, or require multiple staff to use. Busy nurses may not have time to complete screening forms correctly, leading to scoring errors and missing data. While some participants responded with extra training sessions and creative workarounds, they stressed that these problems are built into the system: without enough staff, proper equipment, and institutional support, even the best-designed tool will not work well in day‑to‑day care.
Normal body changes versus true malnutrition
One of the most important insights from the interviews is that weight loss after spinal cord injury is not always a warning sign. After injury, people often lose muscle below the level of the damage, so the scale almost always goes down, even if they are eating enough. Generic tools treat any recent weight loss as a red flag, which can trigger unnecessary nutrition interventions and even overfeeding. At the same time, focusing on thinness overlooks another serious problem: many people with spinal cord injury gain too much fat over time because they move less and their energy needs fall. Dietitians described using a mix of clues – such as skin condition, infections, rehabilitation progress, blood tests, and detailed diet histories – to judge risk, but noted that no single number or lab value reliably separates expected body change from true malnutrition.
Too little, too much, and everything in between
Clinicians in this study saw malnutrition as a spectrum, not just a matter of being too thin. Psychological distress, low mood, and shock after injury can suppress appetite and interest in food. Hospital food may feel unappealing or unfamiliar, especially over long stays, and patients without family or friends bringing in extra meals may eat less. After discharge, limited income, trouble shopping and cooking, and ongoing bowel or bladder problems can disrupt eating patterns. On the other side, overnutrition and weight gain are common and can contribute to pressure injuries, heart disease, and metabolic problems. Dietitians were concerned that current tools pay too little attention to this side of the problem, even though it is widespread and harmful.
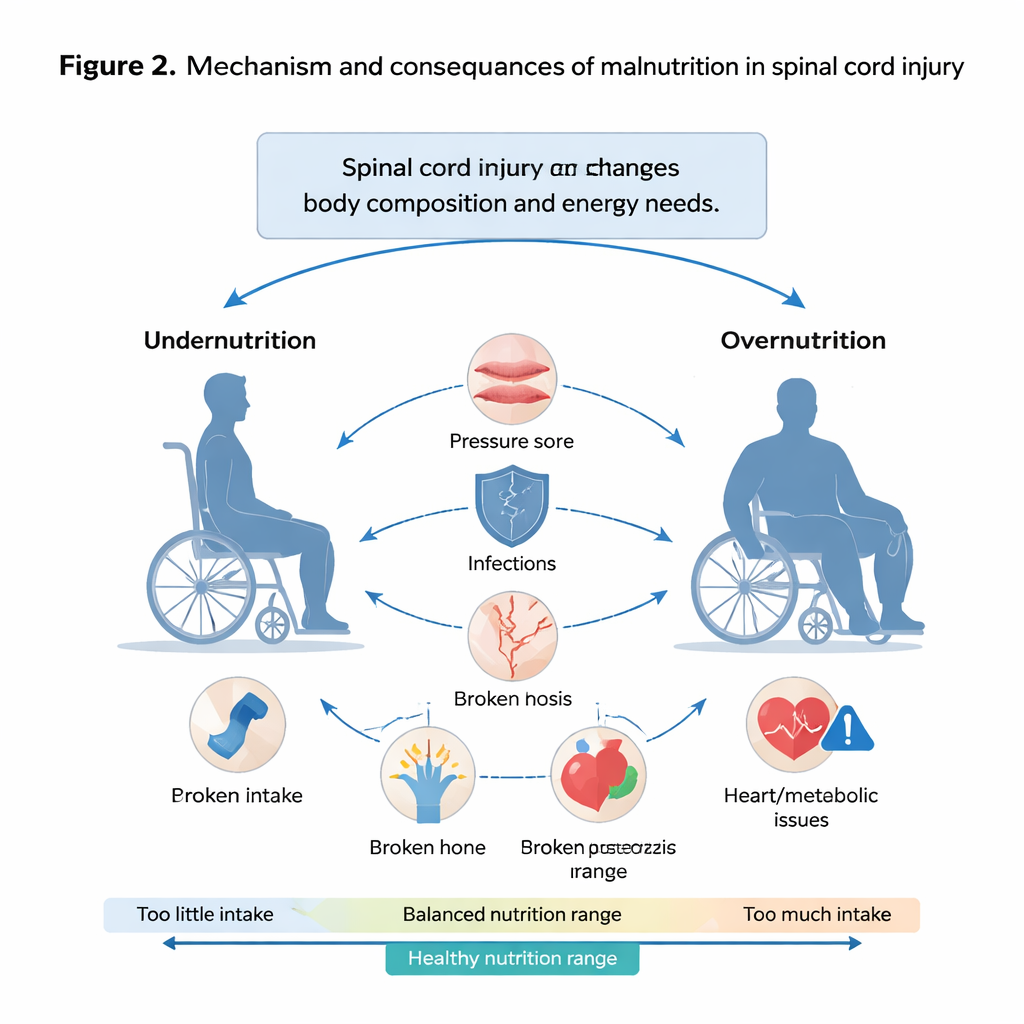
What needs to change to protect patients
The study concludes that a "weight‑centric" approach is not enough for people with spinal cord injury and can mislabel both undernutrition and overnutrition. The authors argue for tailored guidelines and tools that give more weight to function, clinical signs, body composition, and psychosocial factors, while still being practical in busy services. One existing spinal cord injury‑specific screening tool shows promise, but is not widely used and may increase workload. The authors suggest building on familiar frameworks and tools, adapting them for spinal cord injury, and pairing them with better staff training, appropriate weighing equipment, and supportive policies. For patients and families, the key message is that good nutrition care after spinal cord injury requires looking beyond the scale to the whole person, so that the right people get the right help at the right time.
Citation: Keenan, S.J., Gunter, S.I., Meewathurage, D.C. et al. Towards accurate malnutrition identification in individuals with Spinal Cord Injury: a qualitative investigation. Spinal Cord Ser Cases 12, 1 (2026). https://doi.org/10.1038/s41394-026-00727-3
Keywords: spinal cord injury, malnutrition, nutrition screening, dietitian practice, rehabilitation