Clear Sky Science · en
Gut microbiota modulation via repeated donor fecal transplantation improves motor and gastrointestinal symptoms in drug-naïve Parkinson’s disease: a randomized phase 2 trial
Why the Gut Matters in a Brain Disease
Parkinson’s disease is usually thought of as a brain disorder that causes tremors, stiffness, and slow movement. Yet many people with Parkinson’s also struggle with years of constipation and other gut troubles. This study asks a bold question with real-world relevance for patients and families: if the gut and its resident microbes are involved in Parkinson’s, can carefully transferring healthy microbes from donors ease symptoms without using standard Parkinson’s drugs?
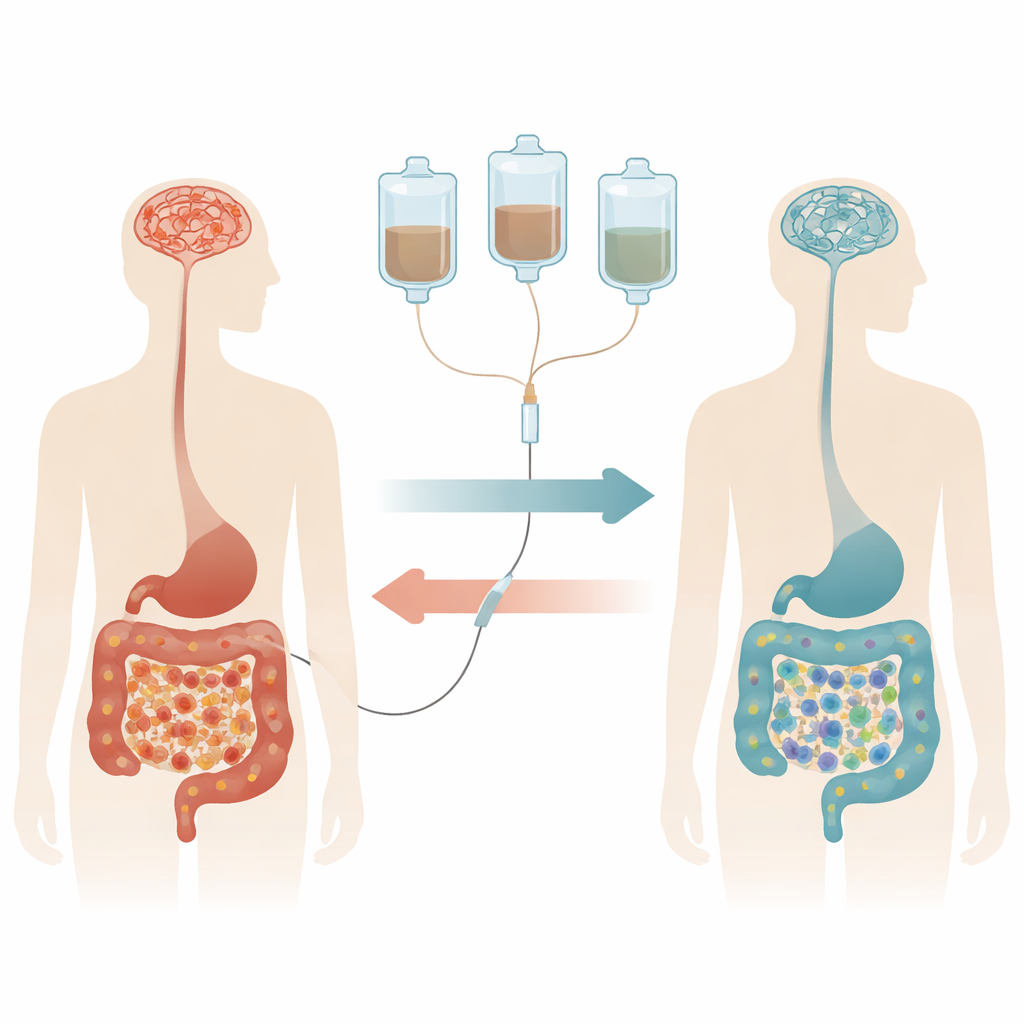
Rethinking Parkinson’s from the Inside Out
Growing evidence suggests that Parkinson’s may begin, at least in part, in the gut. Some researchers propose that a misfolded protein linked to the disease forms in the intestine and then travels to the brain along nerve pathways. People with Parkinson’s often have an unhealthy mix of gut bacteria, a leaky intestinal barrier, and chronic gut inflammation. These changes may contribute to both bowel problems and damage in the brain regions that control movement. If this is true, then improving the gut environment early in the disease might offer a new, non-drug way to slow or soften symptoms.
Testing Microbe Transfer in Newly Diagnosed Patients
To put this idea to the test, the researchers ran a 35-week, randomized, double-blind clinical trial in 72 people with newly diagnosed Parkinson’s who had never taken Parkinson’s drugs. Half received repeated fecal microbiota transplantation (FMT) from healthy donors, delivered directly into the lower gut through a thin tube placed during colonoscopy. The other half received the same procedure but using their own stool, serving as a placebo comparison. Treatments were given in three cycles over several months, and neither patients nor doctors knew who received donor material.
Improvements in Movement and Bowel Habits
By the end of the study, those who received donor microbes showed clearer benefits than those who received their own. On a standard movement rating scale widely used in Parkinson’s research, the donor group improved by nearly four points on average, while the placebo group did not change. Almost half of the donor-treated patients reached a level of improvement considered noticeable in everyday life for early Parkinson’s. Constipation and other gut symptoms improved even more strikingly in the donor group, and patients reported better quality of life related to digestion and daily activities. These gains emerged within the first few months and, for many measures, persisted through week 35.
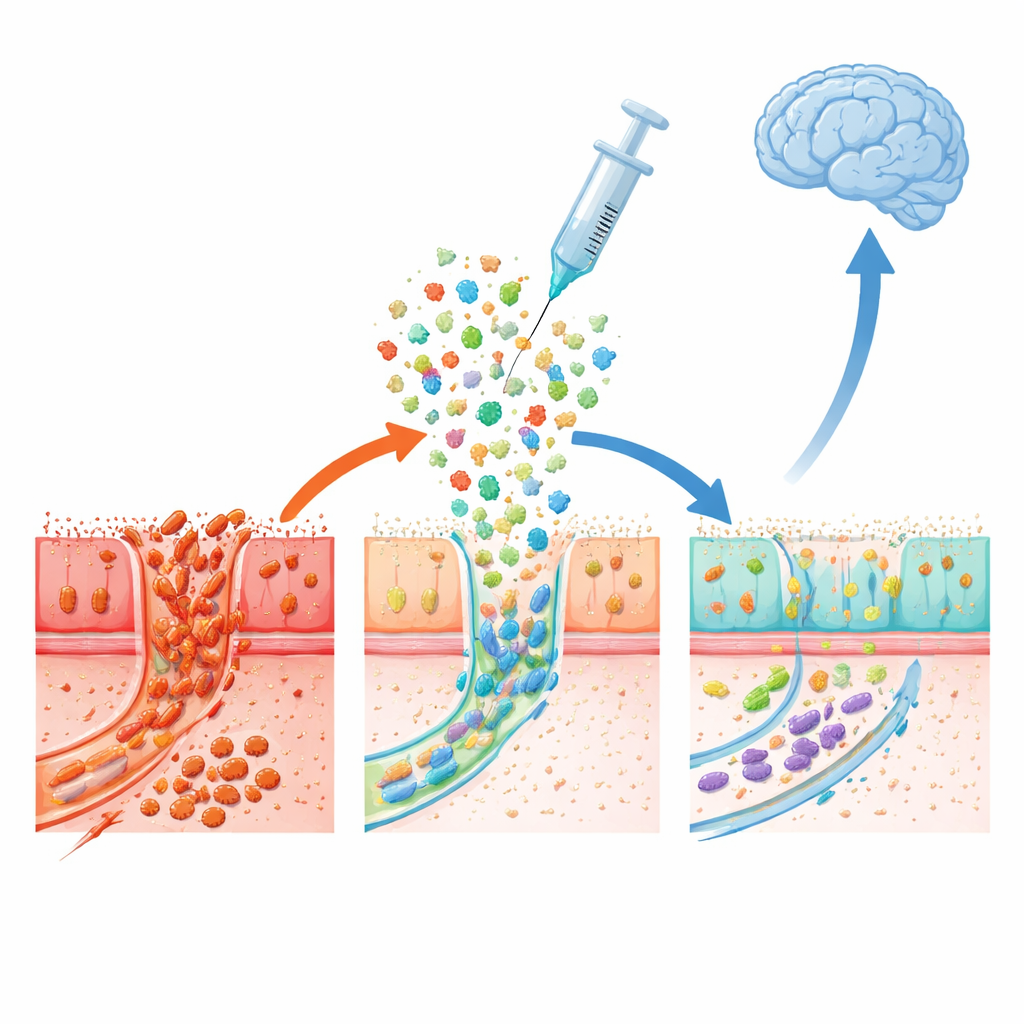
What Changed Inside the Gut
Beyond symptoms, the team examined what was happening biologically. The donor group’s gut communities shifted to more closely resemble those of the healthy donors, with a marked drop in a group of bacteria called Escherichia-Shigella, which has been repeatedly tied to Parkinson’s-related gut imbalance. Reductions in these bacteria were linked to less buildup of the disease-related protein in colon tissue, stronger cell-to-cell connections in the intestinal lining, and higher levels of dopamine-related chemicals in the stool. Together, these findings suggest that the new microbes helped calm gut inflammation, tighten the gut barrier, and reshape the local chemistry in ways that could ease harmful signaling along the gut–brain pathway.
Safety, Limits, and What Comes Next
All treatments were generally well tolerated: side effects like mild stomach pain, bloating, or brief diarrhea were short-lived, and no serious complications were seen. Still, this was a single-center study with a modest number of participants, and the specialized delivery method requires expert care. Larger, multi-center trials will need to confirm how long the benefits last, who is most likely to respond, and whether less invasive approaches can work as well.
What This Means for People with Parkinson’s
For lay readers, the takeaway is that this carefully designed trial offers early but encouraging evidence that adjusting the gut’s microbial community using repeated donor fecal transplants can produce meaningful improvements in both movement and bowel function in people with untreated, early-stage Parkinson’s. The results support the idea that the gut–brain connection is not just an abstract theory but a real target for new therapies. While FMT is not ready to replace standard care, microbiome-based treatments may soon join the toolkit for managing neurodegenerative diseases.
Citation: Zhang, R., Feng, R., Wang, J. et al. Gut microbiota modulation via repeated donor fecal transplantation improves motor and gastrointestinal symptoms in drug-naïve Parkinson’s disease: a randomized phase 2 trial. Sig Transduct Target Ther 11, 94 (2026). https://doi.org/10.1038/s41392-026-02604-9
Keywords: Parkinson’s disease, gut microbiome, fecal microbiota transplantation, gut–brain axis, neurodegeneration