Clear Sky Science · en
Spatiotemporal profiling reveals distinct dynamics and checkpoint regulations of CAR-T and CAR-NKT cells against solid tumors
Why this research matters for future cancer care
Many people have heard of CAR-T cells, a cutting-edge treatment in which a patient’s own immune cells are engineered to hunt down cancer. These therapies work remarkably well in blood cancers but have struggled against solid tumors such as ovarian, lung, or pancreatic cancer. This study asks a simple but crucial question: is there a better kind of immune cell for the job? By comparing traditional CAR-T cells with a different engineered cell type called CAR-NKT cells, the researchers map out how each behaves inside the body over time and suggest how to make next-generation, off-the-shelf cell therapies safer and more effective for solid tumors.
Two custom-built cancer-fighting cell types
The team created two therapies that recognize the same tumor marker, mesothelin, commonly found on ovarian and other solid tumors. Conventional CAR-T cells were made from adult blood T cells, similar to those used in current clinical products. CAR-NKT cells, by contrast, were grown from cord-blood stem cells into a specialized immune subset called invariant natural killer T cells, then equipped with both a tumor-targeting receptor and a built-in supply of the growth factor IL-15. While CAR-T cells mainly attack via their engineered receptor, CAR-NKT cells can kill in several ways at once: through the CAR, through their natural T-cell receptor, and through powerful natural killer–like receptors. In lab dishes, CAR-NKT cells destroyed a wide range of ovarian cancer cell lines, including those with little or no mesothelin, whereas CAR-T cells were largely limited to tumors that displayed the target strongly.
Stronger tumor control with fewer systemic side effects
When tested in mice bearing human ovarian tumors, the contrast became even clearer. Both therapies were injected into the abdominal cavity, where the tumors grew. CAR-T cells initially slowed tumor growth but eventually spread widely throughout the body and expanded explosively, causing graft-versus-host–like disease and death in all treated animals. CAR-NKT cells, however, homed efficiently to the tumors, expanded in a controlled way, cleared the cancer, and then gradually contracted while remaining detectable for more than 100 days. They largely stayed confined to the tumor region instead of flooding healthy organs, and the mice did not develop the severe toxicities seen with CAR-T cells. The authors also showed that adding IL-15 to CAR-T cells boosted their power but made their side effects far worse, whereas IL-15–engineered CAR-NKT cells gained persistence without triggering dangerous inflammation.
How location, metabolism, and memory set CAR-NKT cells apart
To understand why these two therapies behave so differently, the researchers profiled hundreds of thousands of individual cells taken from tumors, blood, spleen, and liver over several weeks. CAR-NKT cells had a “stay-put” chemokine receptor pattern that favored remaining in inflamed tissues and tumors, rather than recirculating through lymph nodes. Inside tumors, they settled into durable effector and memory-like states with relatively low signs of exhaustion, and maintained robust energy pathways such as oxidative phosphorylation and stable amino acid metabolism. CAR-T cells, in contrast, showed more erratic shifts between proliferating, attacking, and exhausted states, especially in tumors and spleen, and their metabolic programs were less stable. Overall, CAR-NKT cells moved more slowly along the path toward terminal exhaustion and kept more flexibility to continue fighting.
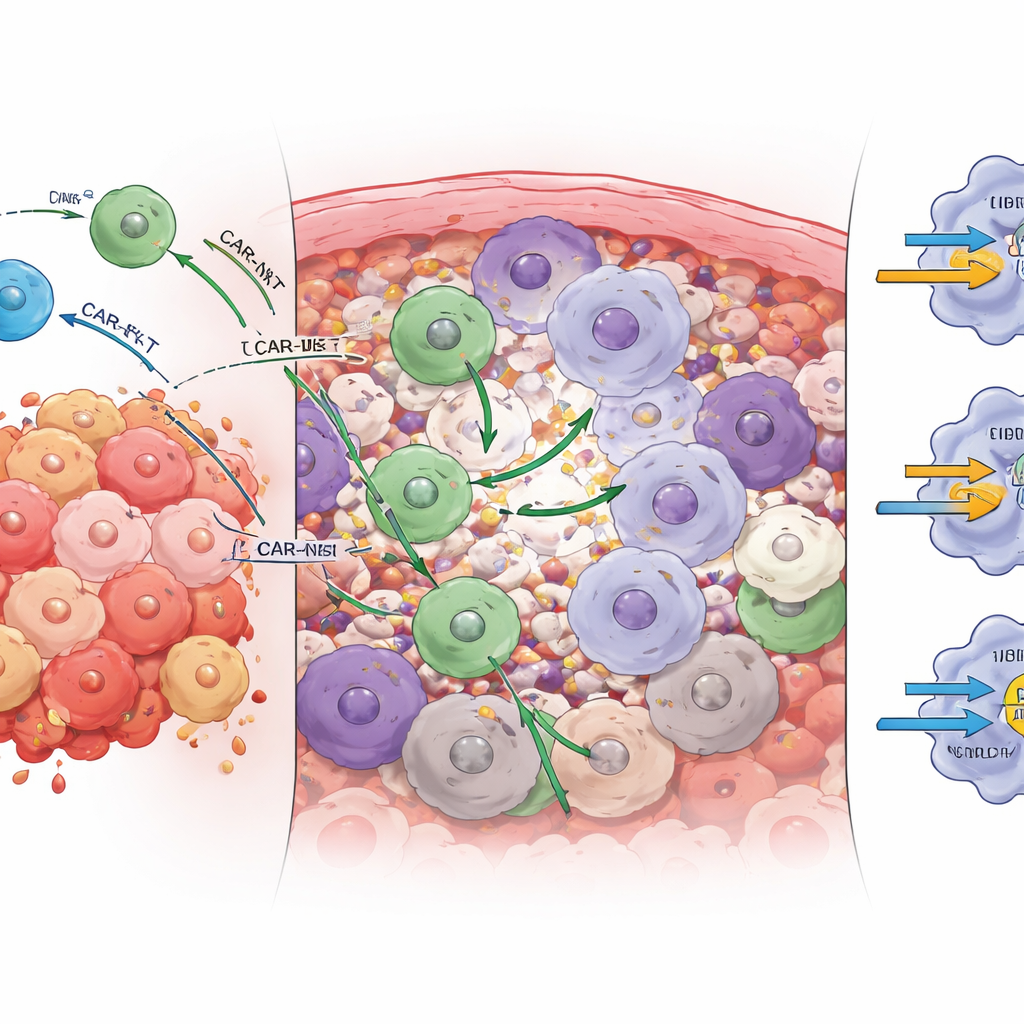
Different “brakes” control each cell therapy
The tumor microenvironment uses so-called immune checkpoints—molecular brakes on immune cells—to dampen attacks. By analyzing how engineered cells and tumor cells talk to each other through receptor–ligand pairs, the study found that the dominant brakes are not the same for CAR-T and CAR-NKT cells. For CAR-T cells, a key inhibitory interaction involved the receptor TIGIT on the immune cells binding to its partner on tumor cells. In mice, blocking TIGIT significantly improved CAR-T tumor control and survival. CAR-NKT cells, however, were most strongly restrained by a related receptor called CD96. Blocking CD96—not TIGIT—boosted CAR-NKT cell numbers, activation, and tumor clearance. Traditional PD‑1/PD‑L1 blockade, which has disappointed in many solid tumor trials, had little effect in this model, consistent with low PD‑L1 levels on the ovarian tumors studied.
What this means for next-generation cancer therapies
To a lay reader, the take-home message is that not all engineered immune cells are created equal. CAR-NKT cells, especially when produced from stem cells as standardized off-the-shelf products, showed broader tumor-killing ability, better tumor homing, stronger long-term memory, and fewer dangerous side effects than classic CAR-T cells in these solid tumor models. Just as importantly, the study reveals that each cell type is governed by its own dominant checkpoints—TIGIT for CAR-T and CD96 for CAR-NKT—pointing to more tailored drug combinations rather than one-size-fits-all approaches. Together, these insights make a strong case that CAR-NKT cells could form the backbone of safer, more versatile cell therapies for hard-to-treat solid cancers.
Citation: Li, YR., Li, M., Chen, Y. et al. Spatiotemporal profiling reveals distinct dynamics and checkpoint regulations of CAR-T and CAR-NKT cells against solid tumors. Sig Transduct Target Ther 11, 92 (2026). https://doi.org/10.1038/s41392-026-02602-x
Keywords: CAR-NKT cell therapy, CAR-T cells, solid tumors, immune checkpoints, cellular immunotherapy