Clear Sky Science · en
DUSP6 ablation restores CAR T-cell fitness impaired by tumor CD58 loss through invigoration of AP-1 signaling
Why Supercharging Cancer-Fighting Cells Matters
Engineered immune cells called CAR T cells have transformed treatment for certain blood cancers, yet many patients still relapse because their tumors learn how to evade attack. This study uncovers a hidden weakness in some tumors that quietly disables CAR T cells from the inside—and shows how a precise genetic tweak can restore these cells’ stamina, energy supply, and killing power. For readers, it’s a glimpse into how next‑generation cell therapies may become more durable and effective for more people.
A Missing Handle on Tumor Cells
CAR T cells need a firm handshake with their target to work well. Many tumor cells display a surface molecule called CD58 that serves as a “handle” for immune cells, helping them latch on and form a tight contact zone. Earlier work showed that when cancers lose CD58, CAR T cells struggle to form this contact and become less effective. In this study, the researchers asked a deeper question: beyond this mechanical handshake problem, how does CD58 loss rewire the internal biology of CAR T cells to blunt their performance over time?
Shorted Wiring Inside CAR T Cells
By comparing CAR T cells exposed to normal tumors with those facing CD58‑deficient tumors, the team found that a key control hub inside the T cells—called AP‑1—was selectively weakened, while other major signaling routes stayed largely intact. AP‑1 is a group of proteins that turn on genes involved in activation and survival. When AP‑1 activity sagged, CAR T cells showed telltale signs of an internal energy crisis: fewer and smaller mitochondria (their power plants), reduced ability to consume oxygen and use sugar, and a loss of the electrical charge across mitochondrial membranes. At the same time, harmful reactive oxygen molecules built up. Together, these changes pushed CAR T cells toward a self‑destruct program based on damage within their own mitochondria, even without external death signals.
Turning Off an Internal Brake
To understand why AP‑1 was so dampened, the researchers looked upstream for molecular “brakes” that might be overactive. They found that CAR T cells confronted with CD58‑negative tumors ramped up several phosphatases—enzymes that shut down signaling pathways—particularly one called DUSP6. Using drugs and then precise gene editing to block these enzymes, they discovered that removing DUSP6 most strongly revived AP‑1 activity. DUSP6‑edited CAR T cells expanded better, formed more mitochondria, burned fuel more efficiently, produced more cancer‑killing molecules, and were less prone to apoptosis, especially when challenged repeatedly by CD58‑deficient tumor cells.
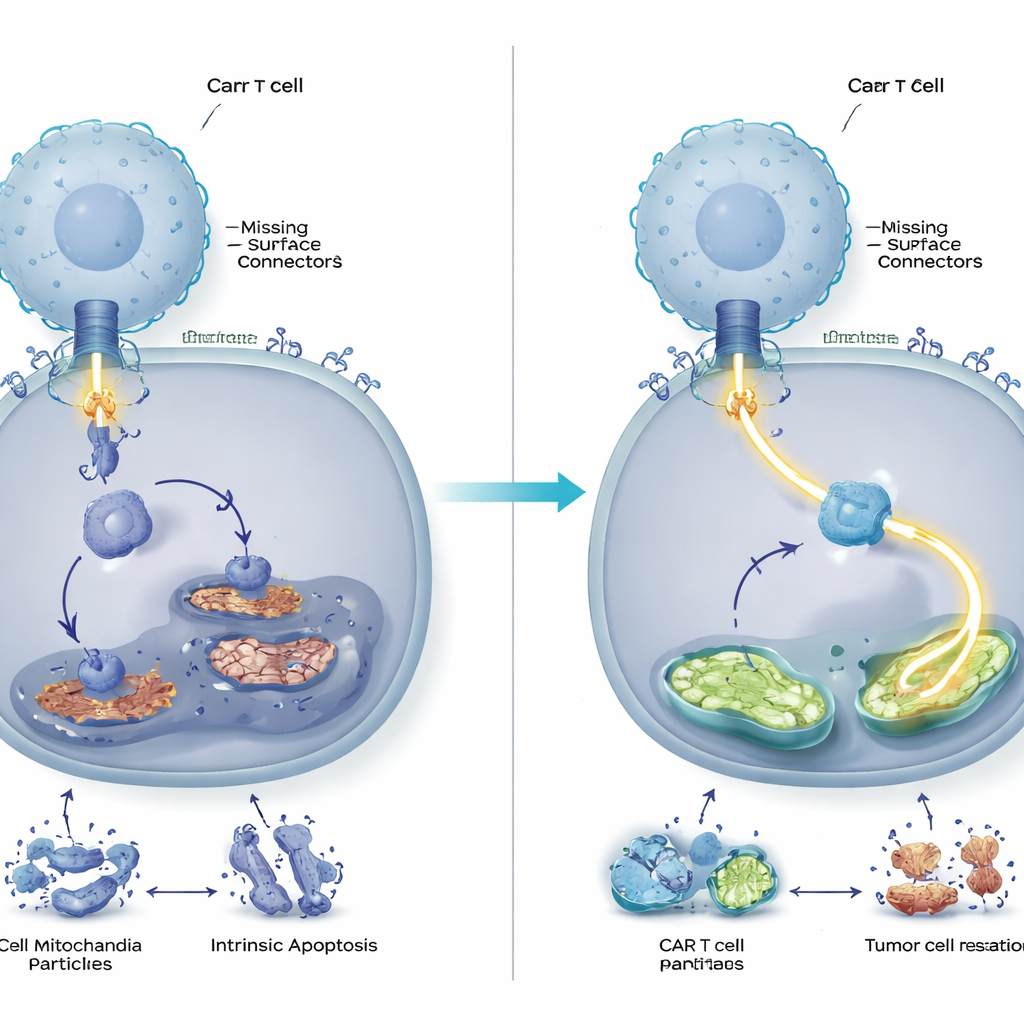
Stronger, Longer‑Lasting Tumor Control in Animals
The team then tested whether this molecular tune‑up mattered in living systems. In mice carrying human blood cancer cells that either had or lacked CD58, DUSP6‑deficient CAR T cells cleared tumors more effectively and kept them at bay longer than conventional CAR T cells. The engineered cells multiplied more robustly, showed fewer markers of exhaustion, and secreted higher levels of key immune messengers. Notably, the benefits of DUSP6 removal were seen not only when tumors lacked CD58 but also when they retained it, suggesting that this modification could broadly enhance CAR T‑cell therapies rather than serving as a narrow fix for a rare tumor subtype.
Hints from Patient Data
To explore relevance in humans, the researchers examined gene‑expression data from people treated with CAR T cells or with immune‑checkpoint drugs. In patients with diffuse large B‑cell lymphoma receiving a dual‑target CAR T therapy, lower DUSP6 levels in CD8 T cells before or shortly after infusion were linked with higher complete‑response rates. In a separate skin cancer cohort treated with anti‑PD‑1 antibodies, exhausted CD8 T cells from non‑responders tended to express more DUSP6 than those from responders. Together, these observations suggest that DUSP6 acts as a negative marker of T‑cell fitness across different immunotherapies and that dialing it down could improve outcomes.
What This Means for Future Cancer Therapies
To a lay reader, the message is that some tumors escape CAR T‑cell attack not just by hiding from recognition but by sabotaging the cells’ internal engines. Losing the CD58 “handle” on tumor cells quietly lowers AP‑1 signaling in CAR T cells, draining their mitochondria, raising toxic by‑products, and nudging them toward early death. By removing the DUSP6 brake, scientists can restore this lost signaling, repair mitochondrial health, and give CAR T cells greater endurance and killing strength, even against resistant tumors. While more safety and clinical testing is needed, DUSP6 ablation emerges as a promising engineering strategy to make living cancer drugs more powerful, longer‑lasting, and potentially effective for a broader range of patients.
Citation: Ma, X., Zhang, Y., Wang, Y. et al. DUSP6 ablation restores CAR T-cell fitness impaired by tumor CD58 loss through invigoration of AP-1 signaling. Sig Transduct Target Ther 11, 100 (2026). https://doi.org/10.1038/s41392-026-02597-5
Keywords: CAR T cells, CD58, DUSP6, cancer immunotherapy, T-cell metabolism