Clear Sky Science · en
Parathyroid hormone–related protein is a therapeutic target in idiopathic pulmonary fibrosis
Why Lung Scarring Matters
Idiopathic pulmonary fibrosis (IPF) is a devastating lung disease in which delicate air sacs gradually turn into stiff scar tissue, making every breath feel like hard work. Current drugs can slow this scarring but cannot stop or reverse it. This study uncovers a previously underappreciated culprit in that process: a small hormone-like protein made by airway lining cells, called parathyroid hormone–related protein (PTHrP), and shows that blocking its action could offer a new way to treat IPF.
A Hidden Messenger in the Airways
IPF has long been linked to overactive fibroblasts—cells that normally help repair tissue but, in this disease, go into overdrive and lay down excessive collagen, the main ingredient of scar. Many studies have focused on signals from immune cells and the deepest air sac cells, but this work looks higher up in the bronchial tree, at the tubes that carry air into the lungs. By reanalyzing large genetic datasets from people with and without IPF, the researchers found that a gene called PTHLH, which encodes PTHrP, was consistently switched on at higher levels in IPF lungs. Microscopic imaging of human lung samples confirmed that the PTHrP protein was much more abundant in patients with IPF and was concentrated in the bronchial epithelial cells that line the airways.
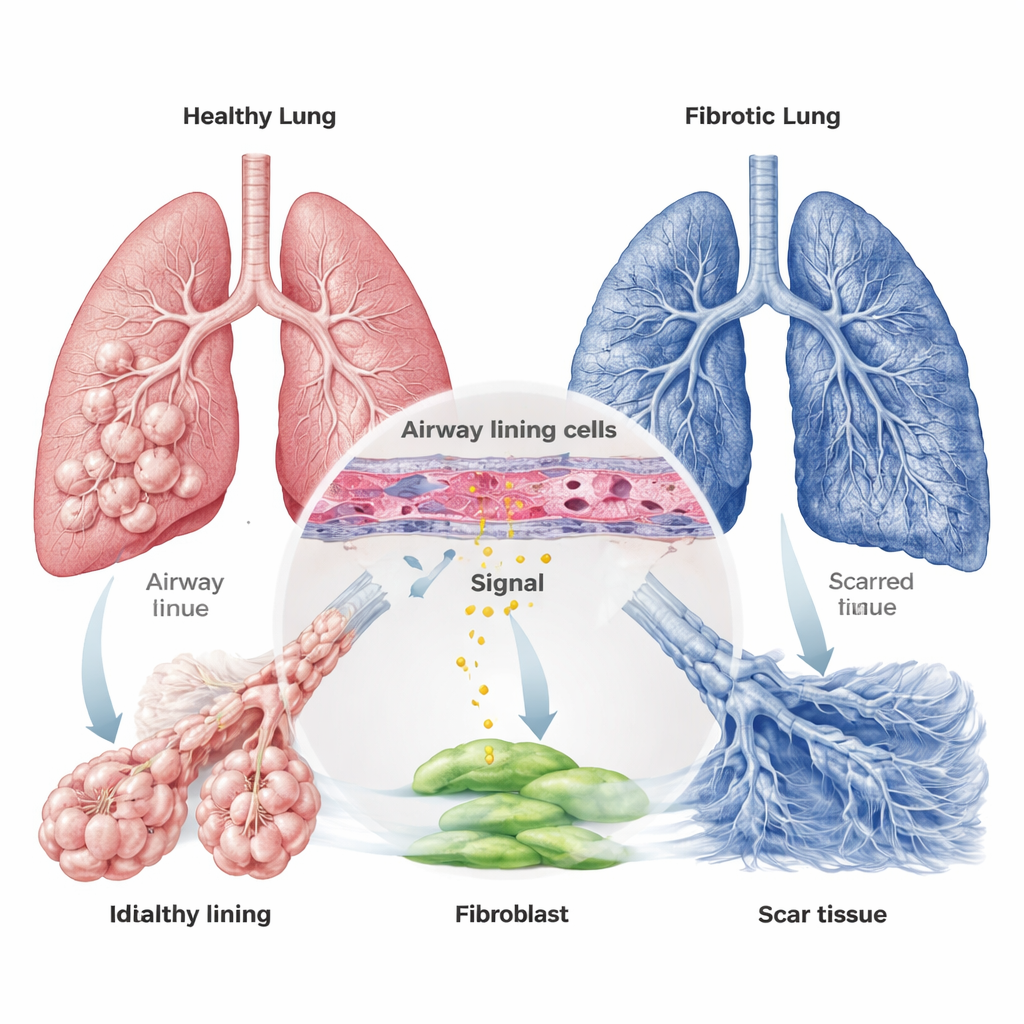
From Airway Signal to Scar-Building Cells
PTHrP is produced as a larger protein that can be cut into several smaller pieces. The team focused on one fragment, PTHrP1-34, known to activate a receptor on certain cells. They showed that bronchial epithelial cells under stress—such as low oxygen or exposure to the chemotherapy-like drug bleomycin, often used to model lung injury in animals—release more PTHrP1-34 into their surroundings. At the same time, they found that the matching receptor, called PTH1R, is mainly present not on the air sac lining cells but on fibroblasts and smooth muscle cells. This sets up a communication line: damaged airway cells send PTHrP1-34, and nearby fibroblasts are tuned to receive it.
How the Signal Turns Fibroblasts Aggressive
In laboratory dishes, adding PTHrP1-34 to human and mouse lung fibroblasts made them adopt a more aggressive, scar-forming state. They increased production of alpha-smooth muscle actin (a hallmark of so-called myofibroblasts) and key collagen genes, and they moved more readily—features associated with progressive scarring. Molecular tests showed that this happens through a specific internal route: PTHrP1-34 binds PTH1R on the fibroblast surface, boosts a messenger molecule called cAMP, and activates an enzyme named PKA, which then turns on “fibrosis genes” in the cell nucleus. Blocking the receptor or inhibiting PKA sharply reduced this response. Importantly, airway and air sac epithelial cells did not respond in the same way, highlighting that this hormone fragment acts very selectively on fibroblasts.
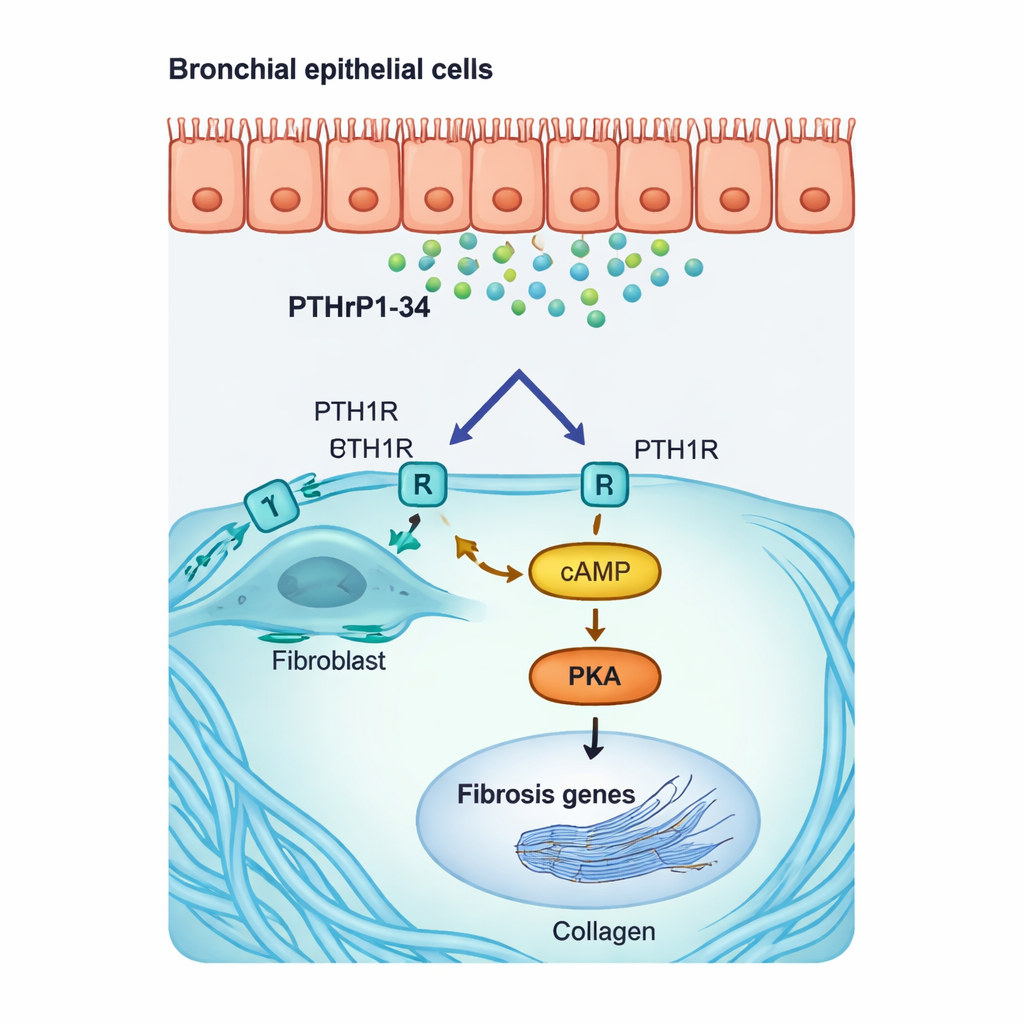
Proof in Diseased Lungs and New Treatment Angles
To see whether this pathway matters in whole lungs, the researchers turned to mouse models of lung injury caused by bleomycin. As the animals’ lungs progressed from early inflammation to dense scarring, PTHrP1-34 levels rose markedly in the airways and lung tissue but not in the bloodstream, suggesting a local, lung-specific surge. Directly delivering PTHrP1-34 into the airways nudged the lungs toward a fibrotic state and, when combined with bleomycin, greatly worsened scarring and collagen buildup. The team then tested three ways to interrupt this harmful signal: a neutralizing antibody that soaks up PTHrP1-34, a short peptide that blocks its receptor (PTHrP7-34), and a gene-silencing approach that lowers PTHrP production in airway cells. In each case, mice developed less lung scarring, had lower collagen levels, and maintained better body weight, with effects that matched or exceeded those of nintedanib, an approved IPF drug.
What This Means for Future Care
For non-specialists, the key message is that the bronchial lining is not just a passive conduit for air; it can actively drive lung scarring by sending out powerful chemical messages. This study identifies PTHrP1-34 as one of those messages and shows that blocking its conversation with fibroblasts can slow or even reverse fibrosis in animal models. While more work is needed to confirm safety and effectiveness in people, targeting the PTHrP1-34/PTH1R pathway could add an entirely new class of treatment for IPF, aiming not just to slow the disease but to tackle one of its root drivers.
Citation: Fang, XQ., Lim, S., Lee, YM. et al. Parathyroid hormone–related protein is a therapeutic target in idiopathic pulmonary fibrosis. Sig Transduct Target Ther 11, 67 (2026). https://doi.org/10.1038/s41392-026-02578-8
Keywords: idiopathic pulmonary fibrosis, lung fibrosis, parathyroid hormone-related protein, fibroblast activation, bronchial epithelium