Clear Sky Science · en
Antiviral drug discovery and development: challenges and future directions
Why We Still Need Better Virus-Fighting Drugs
The COVID-19 pandemic showed how quickly a new virus can upend everyday life—and how much we still rely on good medicines when vaccines are not enough. This review article looks back over 60 years of antiviral drug development and asks: how can we build faster, smarter, and broader defenses against future viral threats? It explains, in accessible terms, how researchers discover, design, and deliver antiviral drugs, what they learned from COVID-19, and how tools like artificial intelligence and nanotechnology may change the game.
From the First Antivirals to Today’s Arsenal
Antiviral medicine is a relatively young field. The first approved drug, idoxuridine in the 1960s, showed that tweaking the building blocks of DNA could slow viral replication, but it also harmed healthy cells and had to be used only on the eye. Later came acyclovir, a landmark herpes drug that is activated mainly inside infected cells, making it both powerful and safe. In the 1980s, zidovudine became the first treatment for HIV, opening the door to modern combination therapies that now turn HIV into a manageable chronic condition. Over the decades, better chemistry and computer-aided design helped bring forward more precise drugs against influenza, hepatitis B and C, HIV, and most recently SARS‑CoV‑2. The review traces this timeline and shows how each breakthrough introduced a new way to outsmart viruses.
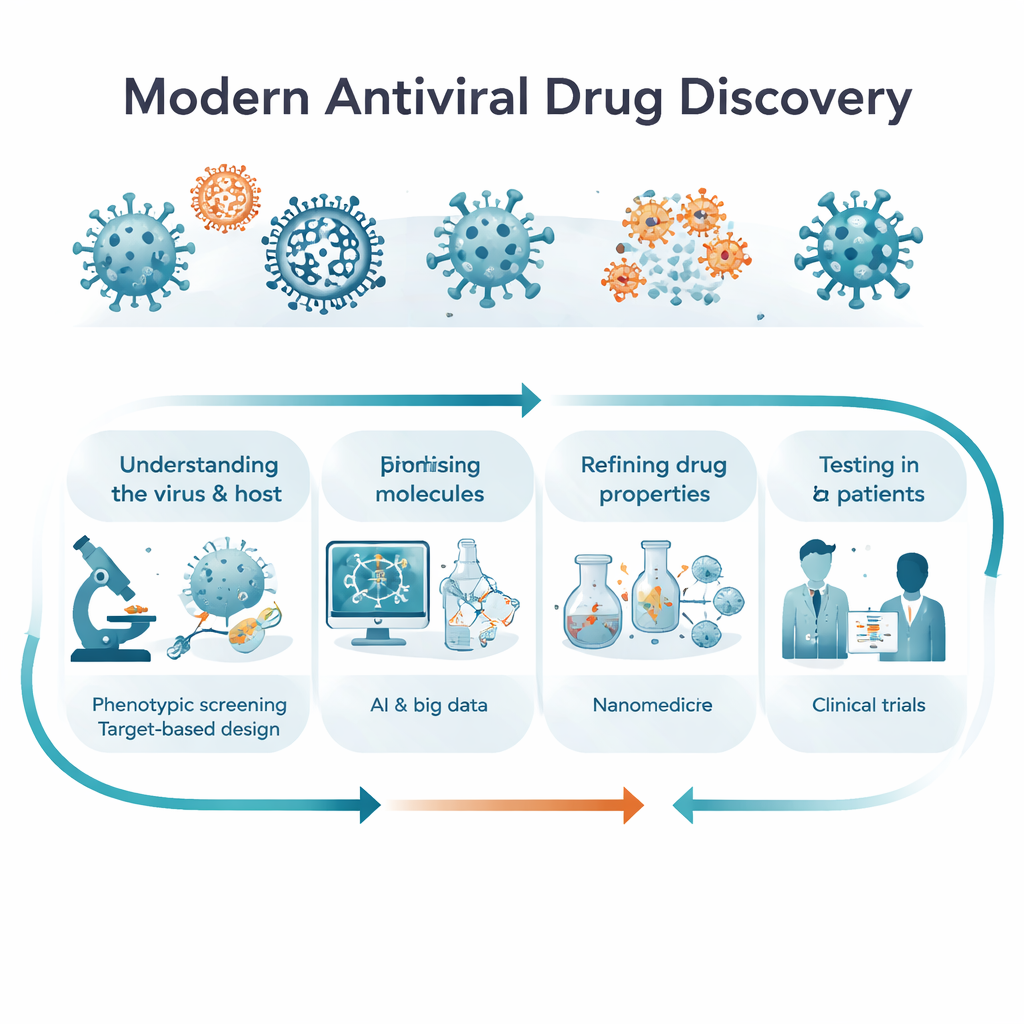
Two Ways to Find a Good Drug: Watching Cells vs. Aiming at Targets
Researchers generally follow two complementary paths to new antivirals. In “phenotypic” discovery, they do not start with a specific protein; instead, they expose infected cells or model organisms to thousands of molecules and simply ask: which ones keep the virus in check and the cells alive? This can reveal surprising, first-in-class drugs, including ones that act on more than one pathway. In “target-based” discovery, scientists first identify a viral or human protein that is crucial for infection—such as a polymerase, protease, or immune signal—and then design molecules to block or tune that target. The article explains how these strategies differ, why they each matter at different stages of research, and how future projects are likely to blend them, moving smoothly from broad observation to precise molecular understanding.
Hitting the Virus—and Its Support System—Where It Hurts
Modern antivirals do far more than just clog a single viral enzyme. The review walks through the viral life cycle, from entry into the cell to genome copying and release, and highlights drug types that interfere at each step. Some compounds bind viral enzymes or structural proteins directly. Others work by targeting host factors that viruses depend on—such as cell-surface receptors, key metabolic enzymes, or innate immune pathways like interferons and toll-like receptors. By acting on host “helper” proteins, these drugs can reduce the chance that a rapidly mutating virus will escape. The authors also describe emerging ideas such as small molecules that disrupt membraneless “droplets” inside cells where viruses assemble, or that selectively degrade viral proteins and RNAs instead of simply blocking them.
Designing Better Molecules: Shape, Properties, and Delivery
Turning an initial “hit” into a useful medicine means more than maximizing potency. Chemists adjust the shape and charge of molecules so they fit their targets like keys in locks, often guided by high-resolution protein structures and simulations. They also tweak water solubility, stability, and metabolism to ensure the drug reaches the right tissue, stays active long enough, and avoids undue toxicity. The article gives examples of how small changes—like adding a side chain or forming a salt—can boost activity against resistant HIV or coronavirus strains while improving safety. It also explains prodrugs, which are inactive or less active forms designed to be converted inside the body, and targeted delivery systems such as liver‑seeking sugar tags and lipid nanoparticles that safely ferry fragile mRNA or nucleic acid drugs into cells.
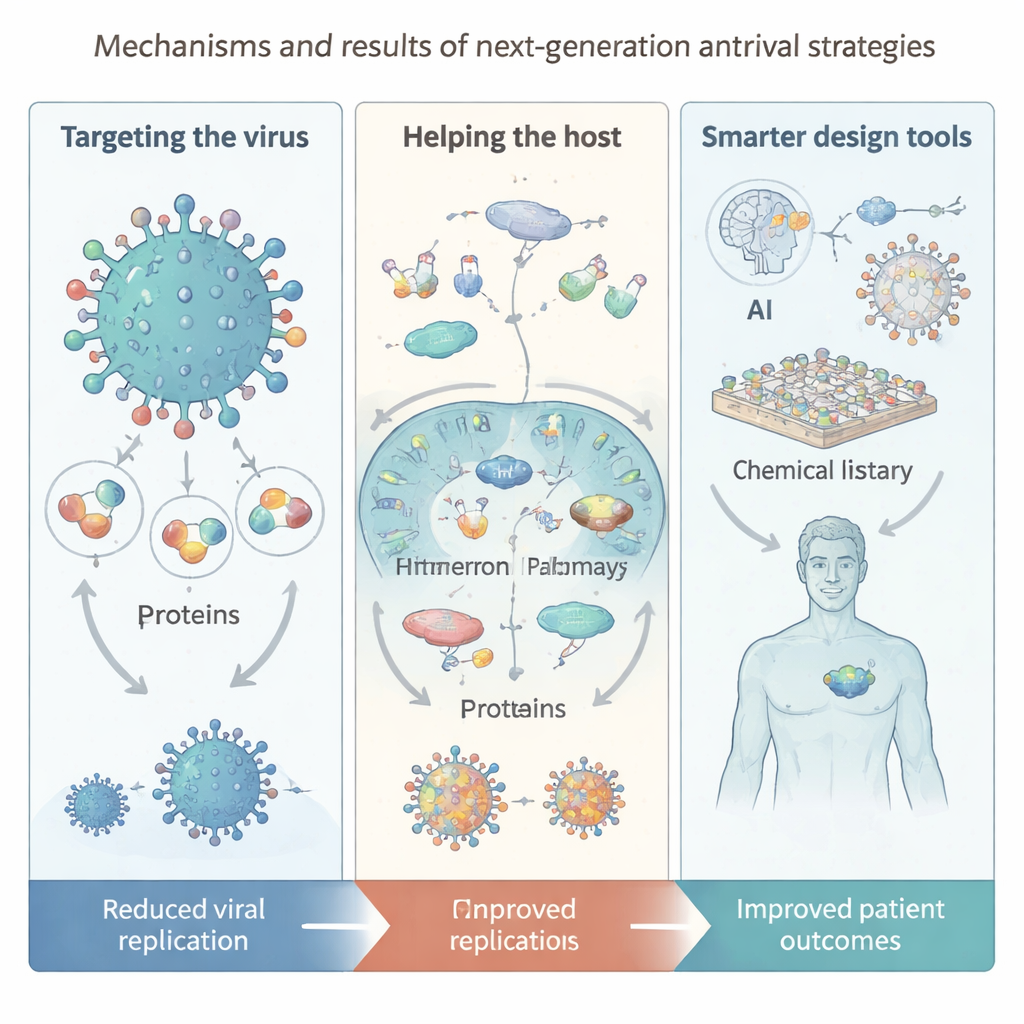
New Tools: Artificial Intelligence, Huge Libraries, and Nanotech
A major theme of the review is how technology is reshaping antiviral discovery. Artificial intelligence now helps predict protein structures, search vast “virtual” libraries containing billions of possible molecules, and propose new compounds or drug combinations. DNA‑encoded libraries and macrocyclic peptide platforms allow ultrafast screening of enormous chemical spaces, while automated synthesis and purification systems speed up the build‑and‑test loop. On the delivery side, nanotechnology provides virus‑like particles, smart polymers, and “nanozymes” that can directly damage viral coats or sharpen immune responses. Yet the authors caution that AI models still depend on high‑quality data, that many generated molecules are hard to make or test, and that issues of safety, fairness, and privacy must be addressed as these tools become more central.
Where Antiviral Drug Discovery Is Headed
For a lay reader, the article’s key message is both sobering and hopeful. Viruses mutate quickly, and no single pill will work forever or against every threat. But by learning from COVID‑19, deepening our understanding of virus–host interactions, and combining smart chemistry, advanced biology, AI, and nanotechnology, scientists are building a more agile antiviral toolbox. Future treatments are likely to be broader in scope, better tolerated, and tailored to hit not just the virus but the vulnerable “weak spots” in the infection process. Continued collaboration across disciplines, industries, and countries will be essential to turn these scientific advances into affordable, practical medicines before the next pandemic arrives.
Citation: Du, S., Hu, X., Li, P. et al. Antiviral drug discovery and development: challenges and future directions. Sig Transduct Target Ther 11, 69 (2026). https://doi.org/10.1038/s41392-025-02539-7
Keywords: antiviral drug discovery, COVID-19 therapeutics, host-targeted antivirals, artificial intelligence in drug design, nanotechnology in medicine