Clear Sky Science · en
Cancer neuroscience: signaling pathways and new therapeutic strategies for cancer
Why Nerves Matter in Cancer
Cancer is usually described as a disease of genes and rogue cells, but this review argues that we have been missing a major player: the nervous system. Nerves do not just sense pain or control muscles; they send chemical and electrical messages that can feed tumors, shape their environment, and even help them spread. Understanding this hidden dialogue between nerves and cancer could open up an entirely new class of treatments that complement surgery, chemotherapy, radiotherapy, and immunotherapy.
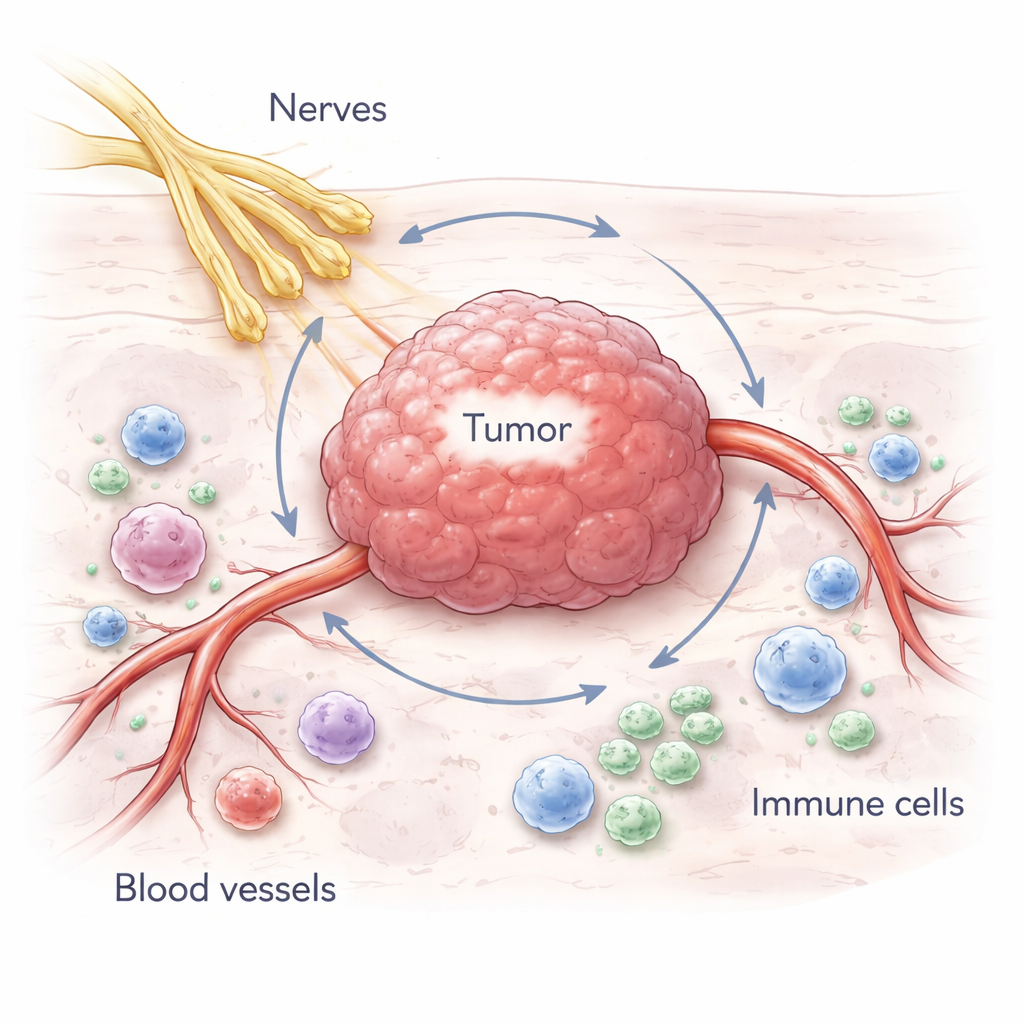
A Two-Way Conversation Between Tumors and Nerves
The authors describe “cancer neuroscience” as the study of how nervous-system activity and cancer influence each other. Nerves reach nearly every organ, and tumors can grow along these fibers or draw new ones into the cancerous tissue. In brain cancers such as gliomas, tumor cells form direct, synapse-like structures with neurons and tap into the brain’s own electrical networks to drive their growth and invasion. Outside the brain, in cancers of the prostate, pancreas, breast, stomach, and others, tumors attract and remodel nearby nerve fibers, using them as both growth signals and potential highways for spread. This two-way traffic means that nerves can stimulate cancer, and cancer can reshape nerves.
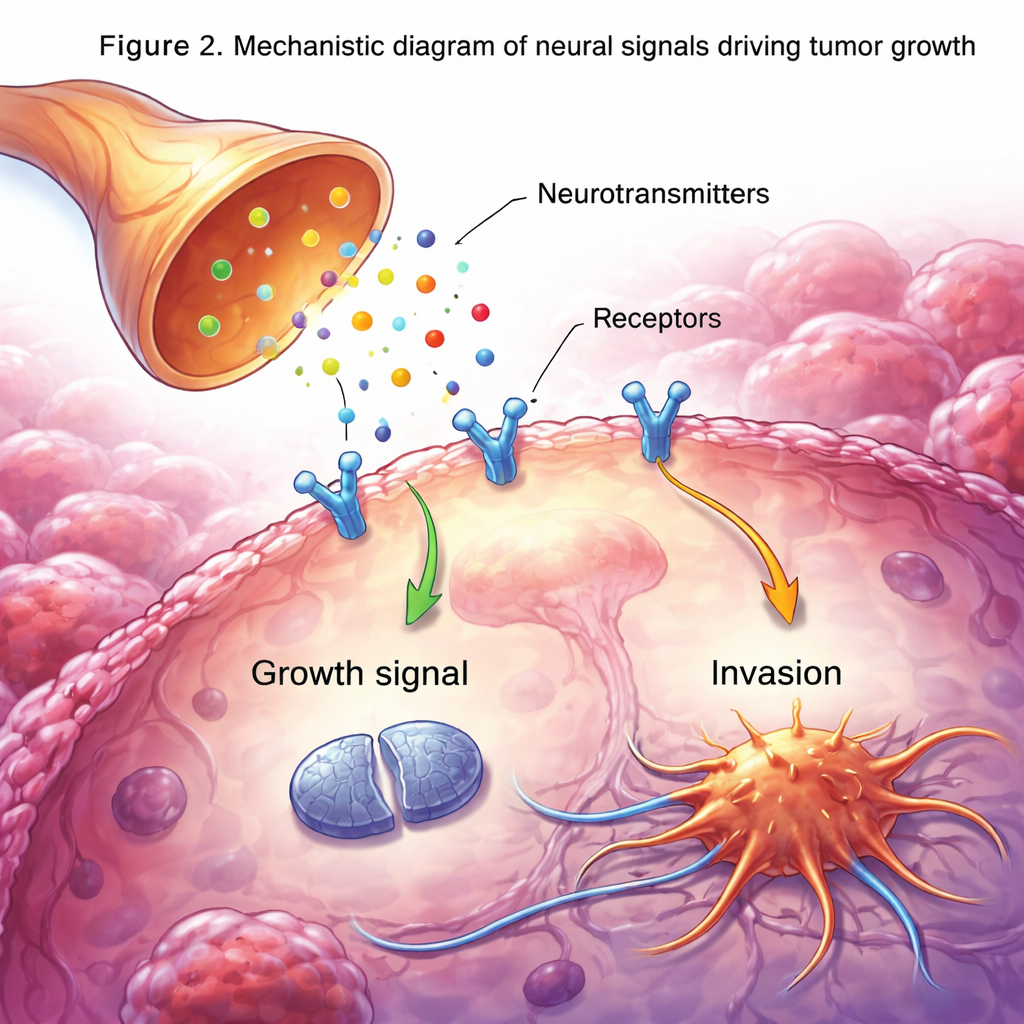
Chemical Messages That Push Cancer Forward
Nerves communicate using substances such as neurotransmitters, neuropeptides, and growth factors, and many of these same molecules turn out to be powerful cancer signals. In brain tumors, neuronal proteins like neuroligin-3 and brain-derived neurotrophic factor (BDNF) can greatly speed up tumor cell division. In the gut and pancreas, substances such as serotonin, acetylcholine, and noradrenaline help cancer stem cells survive, encourage new blood vessels to form, and promote invasion along nerves. Even everyday experiences—stress, smell, pain—can change nerve activity and the mix of these chemicals, indirectly nudging tumors toward more aggressive behavior.
Immune Cells in a Nerve-Controlled Tumor Neighborhood
Cancer does not grow in isolation. It sits in a busy “microenvironment” of immune cells, connective tissue cells, blood vessels, and nerves, all talking to each other. This review highlights how neural signals often push this environment toward a pro-cancer state. Stress hormones and nerve-derived transmitters can blunt the activity of cancer-killing T cells, boost immune-suppressive cells, and coax tumor-associated macrophages and fibroblasts into helping the tumor grow, invade, and escape detection. At the same time, immune cells and even gut microbes can feed signals back to the nervous system, creating complex loops that link mood, inflammation, and cancer progression.
New Treatment Ideas From the Brain–Tumor Link
Because nerves are so deeply wired into tumors, they offer many new points of attack. The authors describe several strategies already being tested: blocking nerve input with drugs such as beta-blockers; cutting or chemically disabling specific nerve branches in highly innervated tumors; using drugs originally designed for neurological diseases (for example, anti-epileptic agents or receptor blockers) to disrupt synapse-like contacts between neurons and cancer cells; and targeting neural signaling molecules or their RNA blueprints with next-generation RNA-based therapies. Early clinical and animal studies suggest that combining such approaches with standard treatments can slow tumor growth, reduce metastasis, and make cancers more sensitive to radiotherapy and immunotherapy.
What This Means for Patients
To a lay reader, the central message is that nerves are not bystanders in cancer; they are active partners that tumors learn to exploit. This emerging field of cancer neuroscience shows that electrical activity in the brain, stress pathways, pain fibers, and even sleep and mood can all feed into how a tumor behaves. By learning how to interrupt these nerve–cancer conversations—whether with existing nerve-targeting drugs, carefully designed RNA medicines, or future therapies that reshape neural circuits—doctors may be able to make current cancer treatments work better and develop entirely new ones. While many of these ideas are still in the research stage, they point toward a future in which treating the nervous system becomes a standard part of treating cancer.
Citation: Zhang, S., Yuan, L., Lin, P. et al. Cancer neuroscience: signaling pathways and new therapeutic strategies for cancer. Sig Transduct Target Ther 11, 66 (2026). https://doi.org/10.1038/s41392-025-02364-y
Keywords: cancer neuroscience, nerve–tumor crosstalk, tumor microenvironment, stress and cancer, neuro-immune interactions