Clear Sky Science · en
Cytoskeleton reorganization induced by a novel K6-K14 keratin fusion promotes cancer stemness and cellular plasticity via cGAS-STING selection
How Shape-Shifting Cancer Cells Outsmart Their Surroundings
Cancer cells don’t just grow uncontrollably; they also learn to bend and twist their own inner “skeleton” to survive, hide, and spread. This study reveals how a specific structural glitch inside head and neck cancer cells can break their nuclei, trigger a built-in danger alarm, push them into a dormant state, and ultimately help them return as more aggressive, invasive, stem cell–like cells. Understanding this mechanical route to cancer evolution could open new ways to block relapse and metastasis.
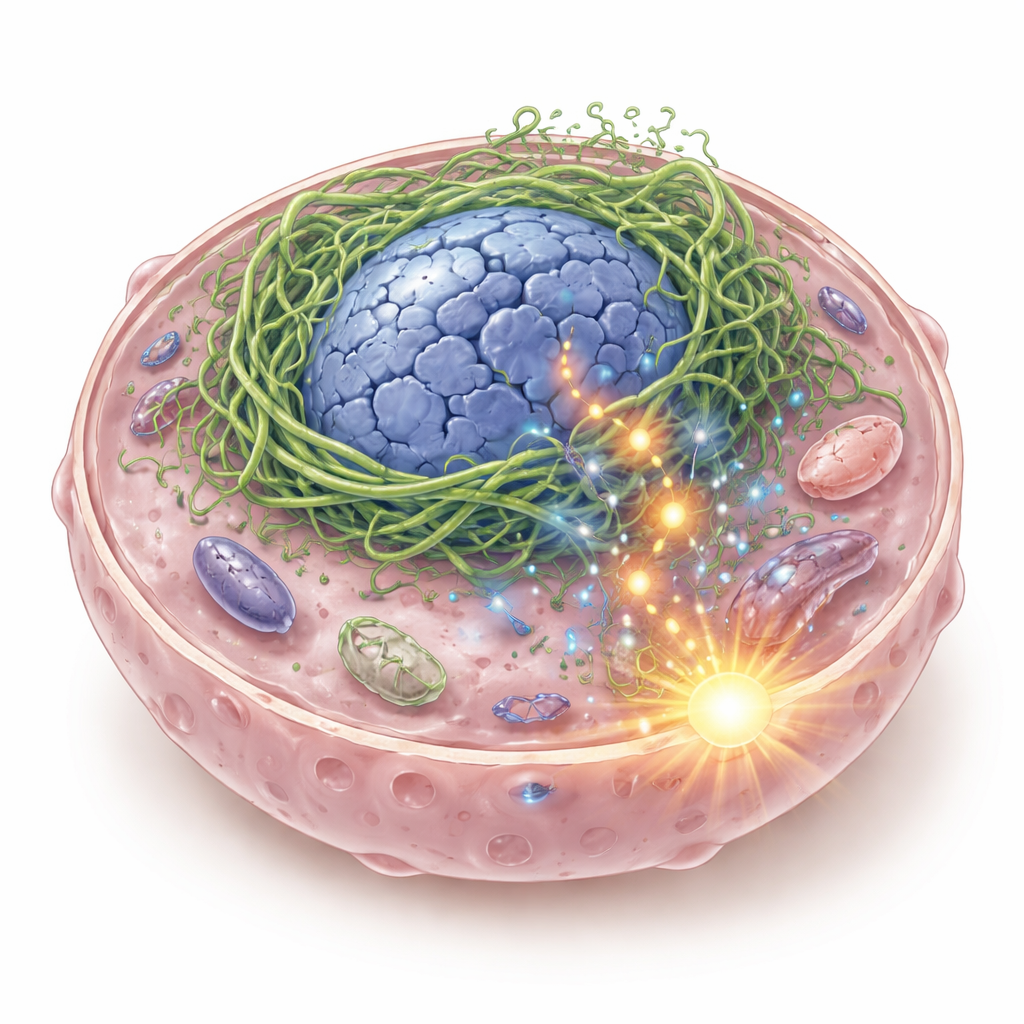
A Broken Inner Scaffold with Dangerous Consequences
Inside every cell is a flexible scaffold made of protein filaments that keeps the cell and its nucleus in shape and helps it sense physical forces. The authors focused on keratins, a family of scaffold proteins common in epithelial tissues, including those lining the mouth and throat. In some head and neck squamous cell cancers, they discovered a hybrid keratin called K6-K14/V5, formed when two keratin genes fuse together. When this fusion protein is switched on in cancer cells, it doesn’t form a smooth supporting network. Instead, it clumps tightly around the nucleus, distorting it into hollow, misshapen structures and causing DNA breaks. Pieces of DNA leak into the cell fluid, where they are detected by an immune-sensing system called cGAS–STING, which normally sounds the alarm when viral DNA is present.
From Cell Death Pressure to Hidden Survival
The immediate effect of this nuclear damage is harmful to the cancer cells: their growth slows, and many die. However, a fraction manages to endure. These survivors are strongly influenced by their physical surroundings. On standard flat plastic dishes they gradually disappear, but when grown within a soft collagen gel—closer to the texture of real tissue—they persist and re-emerge as a new population, called 3D-V5 cells. Gene activity analyses show that these cells respond to the ongoing DNA damage alarm by switching on autophagy, a self-cleaning program that recycles damaged parts, especially faulty mitochondria. This response helps them enter a dormant, low-activity state that allows them to endure stress instead of being eliminated.
Dormant Cells Rewire and Prepare to Move
While dormant, these surviving cells quietly rewrite their internal programs. They change the mix of keratin proteins and adopt a “partial” epithelial–mesenchymal transition (pEMT) state—an in-between identity that keeps some epithelial traits but gains flexibility and motility. They become much better at forming spheres and seeding new cell clusters, a hallmark of cancer stemness. Over time, their mechanical properties recover: they stiffen their nuclei again, rebuild strong actin fibers, and develop long protrusions that probe and grip the surrounding matrix. They also ramp up enzymes called matrix metalloproteinases (MMPs), which chew through the extracellular mesh and open paths for invasion.
Talking to Neighbor Cells to Build a Supportive Niche
These reprogrammed cancer cells do not act alone. The team observed that 3D-V5 cells release large numbers of tiny packages called extracellular vesicles into their surroundings. When these vesicles bathe nearby oral fibroblasts—connective tissue cells—the fibroblasts change their own gene activity, becoming more like cancer-associated fibroblasts that support tumor growth. Many of the signals exchanged revolve around the FGF–FGFR axis, a family of growth factors and their receptors known to drive cell proliferation, plasticity, and resistance. In both lab cultures and mouse tumors, blocking FGFR activity reduced this growth advantage. In animals, tumors formed from 3D-V5 cells were poorly differentiated, more invasive, rich in stem cell markers, and more likely to spread beyond the injection site.
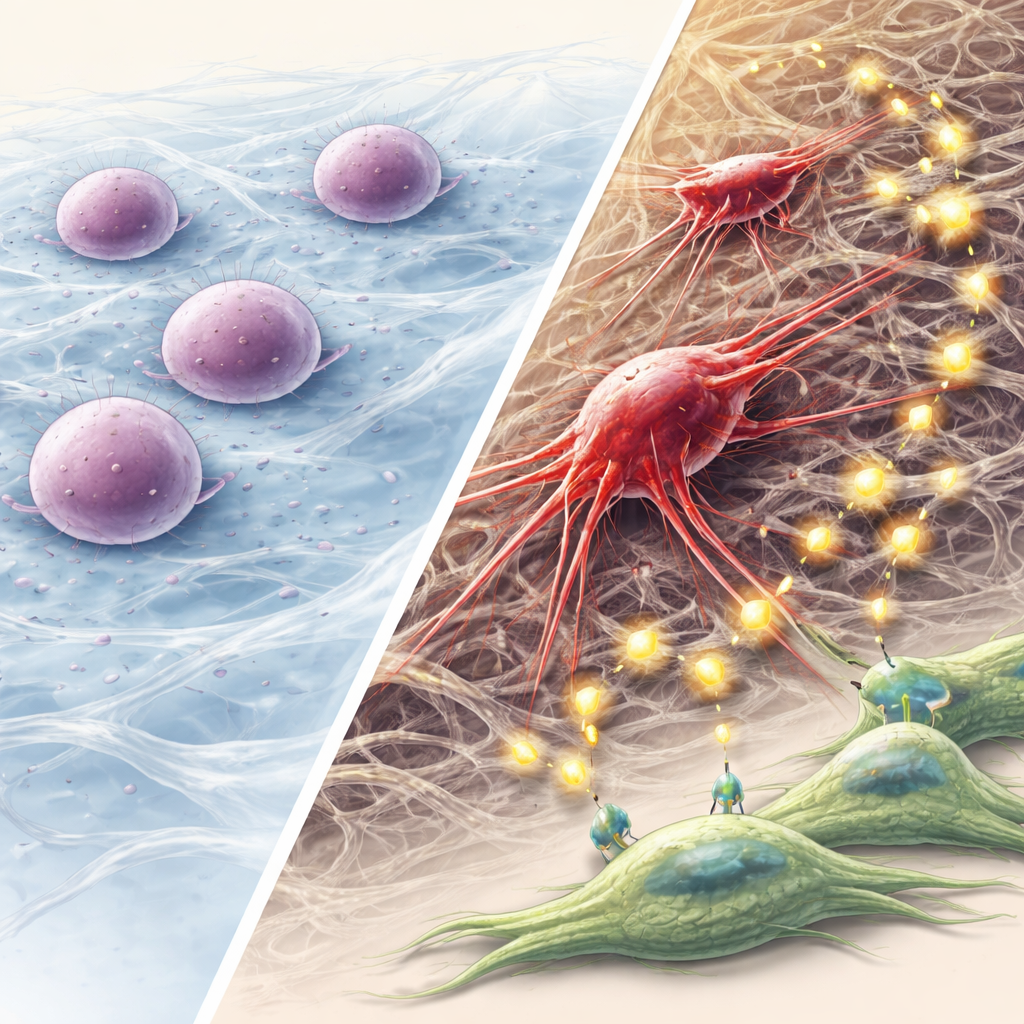
Why This Mechanical Pathway to Aggressive Cancer Matters
This work proposes a stepwise model: a keratin fusion disrupts the cell’s inner scaffold, crushes the nucleus, and triggers a DNA damage alarm; autophagy then allows a few cells to enter dormancy rather than die; over time, these survivors reorganize their skeleton, gain stem-like and invasive traits, and reshape their environment through vesicles and FGF signaling. For non-specialists, the key message is that physical forces and structural proteins inside cells can be just as important as genes and chemicals in driving cancer evolution. Targeting this mechanical stress–autophagy–FGF pathway, especially in head and neck cancers with keratin fusions, may offer new strategies to prevent dormant tumor cells from reawakening and spreading.
Citation: Chen, IH., Ravichandran, S., Lai, MT. et al. Cytoskeleton reorganization induced by a novel K6-K14 keratin fusion promotes cancer stemness and cellular plasticity via cGAS-STING selection. Oncogenesis 15, 5 (2026). https://doi.org/10.1038/s41389-026-00598-1
Keywords: cancer stemness, cell cytoskeleton, tumor dormancy, head and neck cancer, mechanotransduction