Clear Sky Science · en
ULK1 promotes metastatic progression in experimental models of epithelial ovarian cancer
Why this research matters
Epithelial ovarian cancer is often discovered only after it has quietly spread through the abdomen, making it one of the deadliest cancers affecting women. A key step in this spread is the formation of tiny clusters of tumor cells, called spheroids, that float in abdominal fluid, survive chemotherapy, and seed new tumors. This study asks a focused question with big implications: does a cellular “survival switch” called ULK1 help these clusters endure and spread, and could turning it off open new ways to treat advanced ovarian cancer?
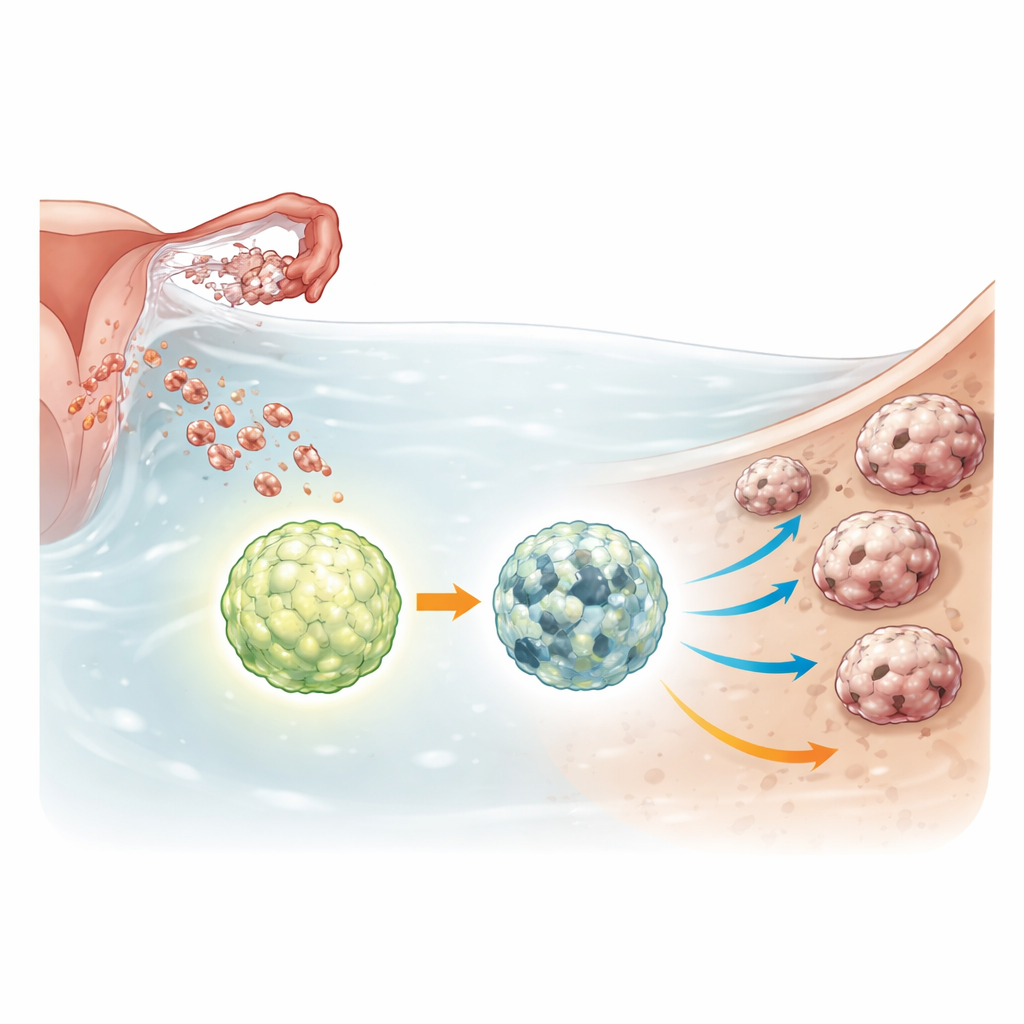
A survival switch inside cancer cell clusters
Ovarian cancer spheroids endure harsh conditions: low nutrients, lack of attachment, and exposure to chemotherapy. To cope, they ramp up a recycling process known as autophagy, which breaks down and repurposes internal components to keep cells alive under stress. ULK1 is a master switch that turns this recycling system on. The researchers used gene-editing tools to completely remove ULK1 from several ovarian cancer cell lines and from a noncancerous fallopian tube cell line that represents early, pre-cancer stages. They then compared how normal and ULK1-deficient cells behaved when grown as free-floating spheroids or as three-dimensional mini-tumors called organoids.
What happens when the switch is turned off
When ULK1 was deleted in ovarian cancer cells, their ability to perform autophagy inside spheroids was strongly impaired, as shown by changes in key recycling proteins. These ULK1-lacking spheroids contained fewer living cells and showed increased signs of programmed cell death, indicating that the cancer clusters could no longer weather stressful conditions as effectively. Interestingly, removing ULK1 from the noncancerous precursor cells did not shut down their recycling system to the same degree, suggesting that cancer cells are more dependent on ULK1 than their healthy counterparts. This cancer-specific reliance makes ULK1 an attractive therapeutic target.
Slowing spread and weakening tumor outposts
Beyond survival in suspension, spheroids must attach to and invade the smooth lining of the abdominal cavity to form new tumors. Using lab models that mimic this early step of metastasis, the team showed that ULK1-deficient spheroids were markedly worse at pushing aside and invading a layer of mesothelial cells, which normally coat abdominal organs. When grown as organoids embedded in a gel-like matrix, ULK1-lacking cancer cells also formed smaller, less robust tumor structures. In mouse models where human ovarian cancer cells were injected into the abdominal cavity, loss of ULK1 led to fewer tumor deposits and less fluid buildup, both hallmarks of advanced disease, even though overall survival of the animals did not improve.
Weakening key signals and boosting targeted drug effects
To understand how ULK1 supports cancer beyond recycling, the researchers mapped protein changes in spheroids lacking ULK1. They found that major growth and survival routes inside the cell—especially the MEK–MAPK and PI3K–AKT–mTOR pathways—were disturbed. These pathways normally help cancer cells resist death and continue dividing. When the team treated ULK1-deficient spheroids with drugs that block MEK or mTOR, the cancer clusters became much more vulnerable, with sharply reduced viability and reattachment ability. By contrast, removing ULK1 did not make standard chemotherapy drugs like carboplatin, paclitaxel, or the PARP inhibitor olaparib work any better, and in some conditions appeared to blunt their benefit.
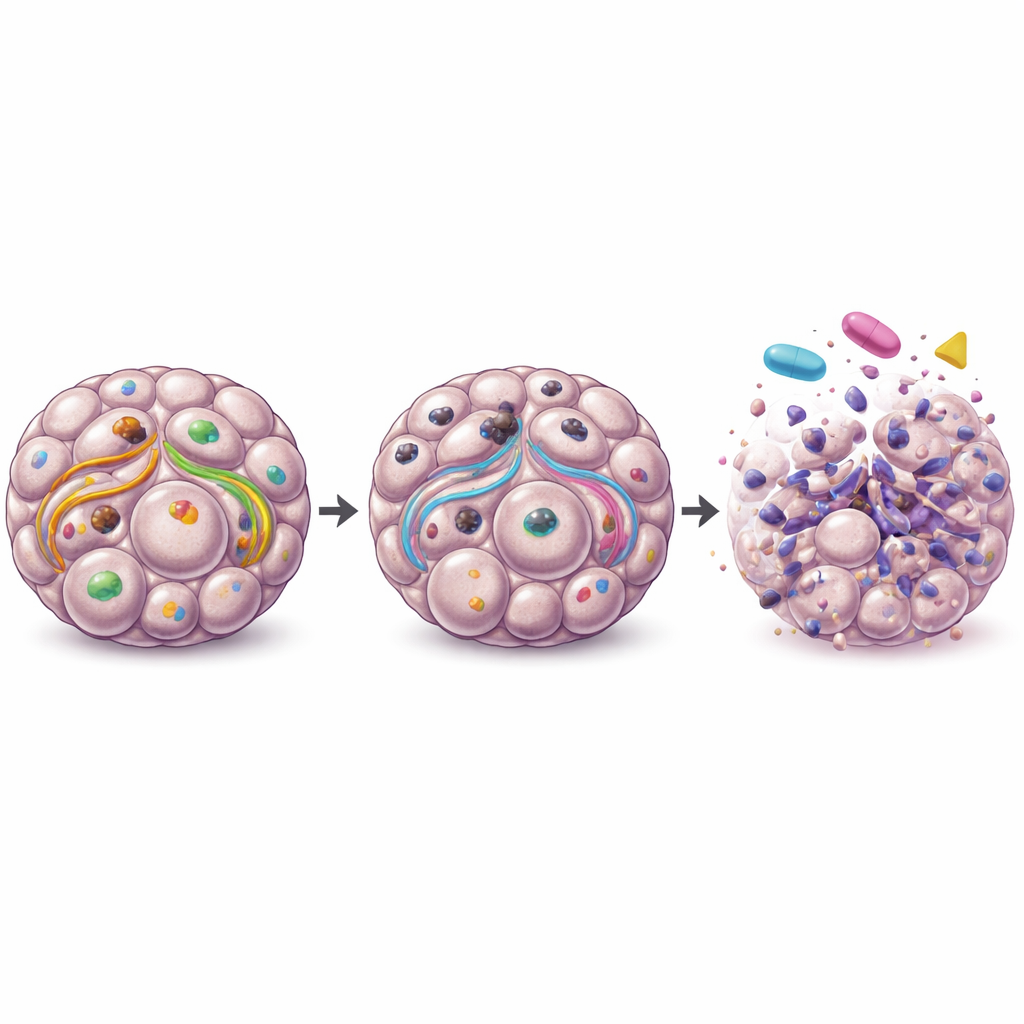
Clues from patient tumors and miniature patient models
Looking at large public datasets of ovarian tumors, the authors found that higher ULK1 gene activity was linked to poorer long-term survival and was especially elevated in metastatic samples compared with primary tumors and normal tissue. To move closer to the clinic, they tested a clinical ULK1-blocking pill, DCC-3116, on patient-derived organoids grown from metastatic tumor samples. In a subset of these patient models, blocking ULK1 alone, or using MEK or mTOR drugs alone, reduced organoid survival, although combining the agents did not consistently add further benefit. Other patient organoids were resistant to all treatments, underscoring how diverse ovarian cancers can be and the need for biomarkers to identify who might benefit.
What this means for future care
Taken together, the findings paint ULK1 as a central helper of ovarian cancer spread: it powers the internal recycling that keeps spheroid clusters alive, supports their ability to invade new sites, and helps maintain powerful growth signals. Turning ULK1 off weakens these processes, shrinks experimental tumors, and makes cancer cell clusters more sensitive to certain targeted drugs, though not to standard chemotherapy. For patients, this work suggests that ULK1 could become part of a precision-medicine strategy—especially for those with ULK1-high, metastatic disease—where targeted inhibitors of ULK1 are combined with MEK or mTOR blockers to limit tumor growth and spread, provided that careful testing can identify which tumors are most likely to respond.
Citation: Webb, J.D., Buensuceso, A., Tomas, E.J. et al. ULK1 promotes metastatic progression in experimental models of epithelial ovarian cancer. Oncogene 45, 1111–1127 (2026). https://doi.org/10.1038/s41388-026-03702-2
Keywords: ovarian cancer, metastasis, autophagy, ULK1, targeted therapy