Clear Sky Science · en
The association between steatotic liver disease and chronic kidney disease: a meta-analysis and Mendelian randomization study highlighting metabolic comorbidities
Why Your Liver and Kidneys Matter Together
Doctors have long noticed that people with fatty liver disease often also develop chronic kidney disease, but it has been unclear whether one actually causes the other. This study pulls together results from millions of people and uses genetic data to ask a deeper question: is fatty liver itself harming the kidneys, or are shared problems like obesity, high blood pressure, and unhealthy cholesterol the real culprits? The answer matters for how we screen, treat, and advise the growing number of people with fatty liver.
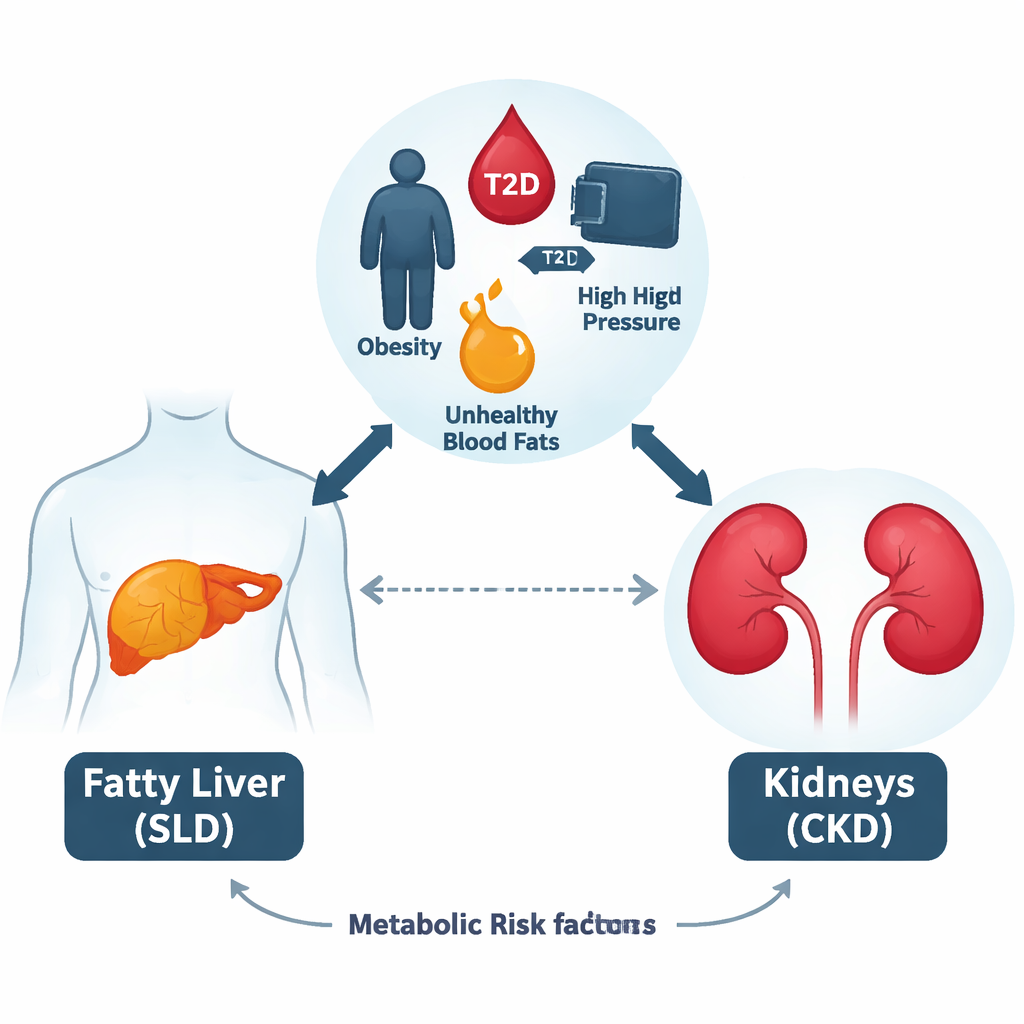
A Closer Look at Two Common Health Problems
Chronic kidney disease, in which the kidneys slowly lose their ability to filter blood, affects almost one in eleven people worldwide and is projected to become a leading cause of death in coming decades. At the same time, steatotic liver disease—an umbrella term that includes older labels such as nonalcoholic fatty liver disease (NAFLD), metabolic-associated fatty liver disease (MAFLD), and metabolic dysfunction-associated steatotic liver disease (MASLD)—has become the most common chronic liver condition. These liver diagnoses all describe excess fat in the liver, but the newer terms explicitly build in metabolic problems, such as obesity, type 2 diabetes, high blood pressure, and abnormal blood lipids, as defining features.
What Observational Studies Have Shown
The authors first updated a large meta-analysis, combining 34 observational studies that followed more than 3.7 million adults over time. Across different study designs, countries, and ways of diagnosing disease, people with fatty liver consistently had higher rates of chronic kidney disease. For example, those with MAFLD or NAFLD were about 30–60% more likely to already have, or later develop, kidney disease than those without these liver conditions. This pattern held in Asian and Western populations, in younger and older adults, and regardless of whether liver fat was detected by ultrasound, blood-based liver fat scores, or medical records.
Using Genetics to Ask What Really Causes What
However, observational studies can be misleading because people with fatty liver almost always have other health problems that also strain the kidneys. To untangle this, the researchers turned to Mendelian randomization, a method that uses natural differences in our genes as a kind of genetic “trial.” They used genetic variants linked to fatty liver and to several metabolic traits—body mass index, waist size, type 2 diabetes, blood pressure, triglycerides, and HDL (“good”) cholesterol—and tested how these variants related to kidney disease in large genetic databases. This approach helps separate true causal effects from simple associations driven by lifestyle or medical differences.
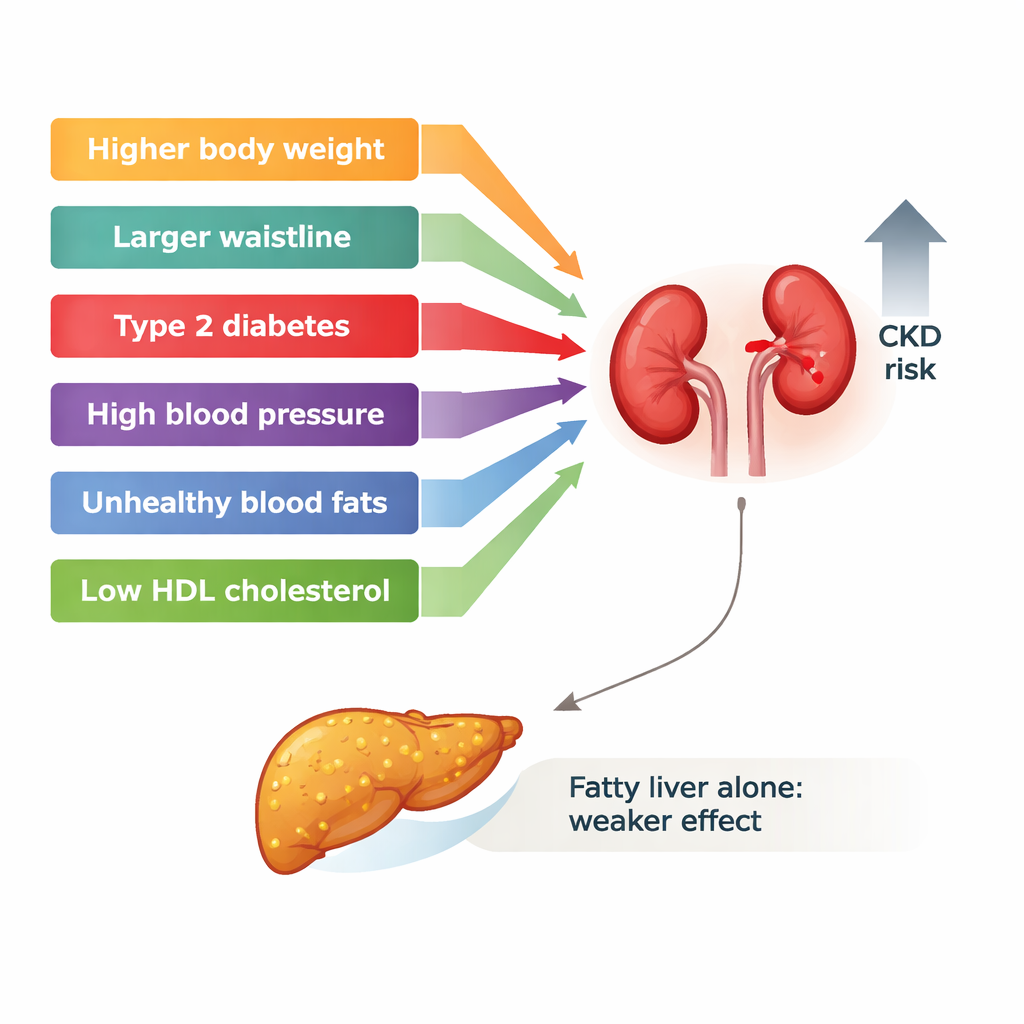
Metabolic Health, Not Fatty Liver Alone, Drives Kidney Risk
When they used this genetic lens, the story changed. Variants that predispose people to fatty liver did not clearly increase the risk of chronic kidney disease. In contrast, genetic tendencies toward higher body weight and waist circumference, higher systolic and diastolic blood pressure, higher triglycerides, and lower HDL cholesterol all raised kidney disease risk. The results suggest that the metabolic disturbances that often accompany fatty liver—excess weight, high blood pressure, and disordered fats and sugars—are the true engines pushing kidney damage, while liver fat itself may be more of a warning sign than a direct attacker.
What This Means for Everyday Health
For someone told they have fatty liver, this study implies that the greatest threat to their kidneys does not come from the liver alone, but from the same underlying metabolic problems affecting both organs. That makes early detection and treatment of high blood pressure, obesity, type 2 diabetes, and unhealthy cholesterol especially important in people with steatotic liver disease. Rather than viewing fatty liver and kidney disease as a simple cause-and-effect chain, the authors argue they should be seen as twin outcomes of broader metabolic trouble. Improving diet, increasing physical activity, managing weight, and controlling blood pressure and blood sugar may therefore protect both the liver and the kidneys at the same time.
Citation: Ji, X., Jiang, J., Liu, Y. et al. The association between steatotic liver disease and chronic kidney disease: a meta-analysis and Mendelian randomization study highlighting metabolic comorbidities. Nutr. Diabetes 16, 4 (2026). https://doi.org/10.1038/s41387-026-00412-2
Keywords: fatty liver disease, chronic kidney disease, metabolic health, obesity, high blood pressure