Clear Sky Science · en
Deficiency of exocyst complex component Exoc5 exacerbates the progression of kidney fibrosis
Why Kidney Scarring Matters
Chronic kidney disease affects hundreds of millions of people worldwide, and a major reason it progresses is fibrosis—scar tissue that slowly replaces working kidney tissue. This study explores a lesser-known cellular machine, the exocyst and one of its parts called Exoc5, to ask a practical question: does this protein help kidneys heal cleanly after injury, or does it push them toward scarring and failure?
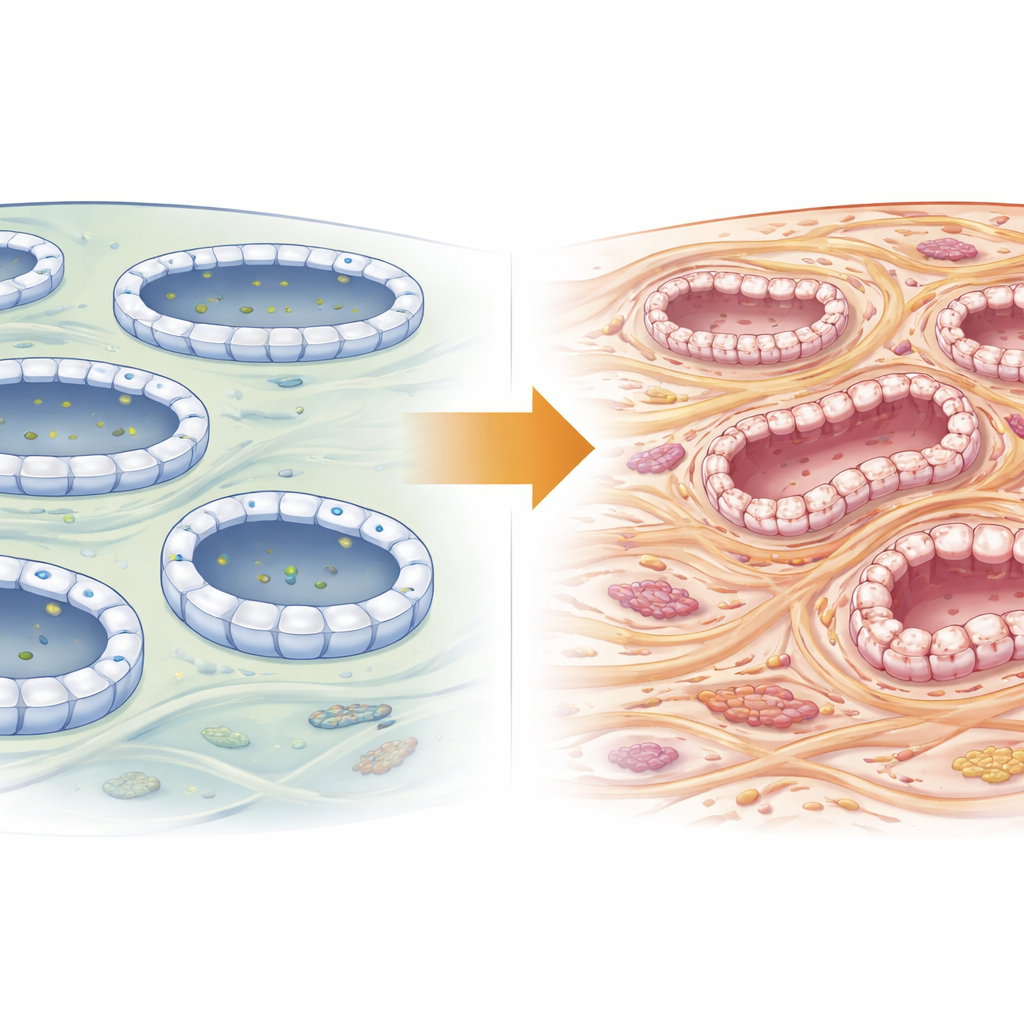
A Cellular Shipping Hub in Kidney Cells
Every kidney tubule cell is a busy logistics center, constantly moving tiny cargo-filled bubbles to precise spots on its surface. This traffic is organized by the exocyst, an eight-part docking complex. Exoc5 sits at the heart of this machine, bridging cargo arriving from inside the cell to the docking site at the outer membrane. Earlier work showed that disrupting Exoc5 harms various organs and that it helps kidney tubule cells maintain their tight, orderly structure. Because disrupted structure is a hallmark of fibrosis, the authors suspected that Exoc5 might quietly decide whether damaged kidneys recover or scar.
Testing Exoc5’s Role in Mouse Kidneys
The researchers engineered mice whose Exoc5 was deleted only in proximal tubule cells—the segments that do most of the kidney’s filtering and reabsorption. Surprisingly, these mice grew normally and had normal kidney structure, transporter placement and function under everyday conditions. To mimic a strong, localized injury that often leads to scarring, the team then tied off one ureter, a standard procedure that causes pressure buildup, inflammation and fibrosis in the affected kidney over a week. In both normal and Exoc5-deficient mice, this obstruction reduced Exoc5 levels, but the knockout animals developed much more severe tubule shrinkage, collagen buildup and invasion by inflammation-related cells.
From Ordered Tubes to Wandering Cells
Healthy tubule cells are tightly connected, with well-defined top and bottom surfaces. During fibrosis they often undergo “epithelial-to-mesenchymal transition,” a shift from an anchored, sheet-like state to a more mobile, fibrous one. The authors found that after obstruction, kidneys lacking Exoc5 showed stronger activation of key EMT drivers and higher levels of proteins typical of migrating, fiber-producing cells, along with greater loss of junction proteins that normally keep tubule cells polarized. They also observed the reappearance of Pax2, a developmental regulator normally switched off once kidney tubules mature. Pax2 came back more strongly in Exoc5-deficient tubules, particularly in stressed cells that were not successfully dividing, suggesting that loss of Exoc5 pushes cells toward a half-repaired, dedifferentiated state prone to scarring.
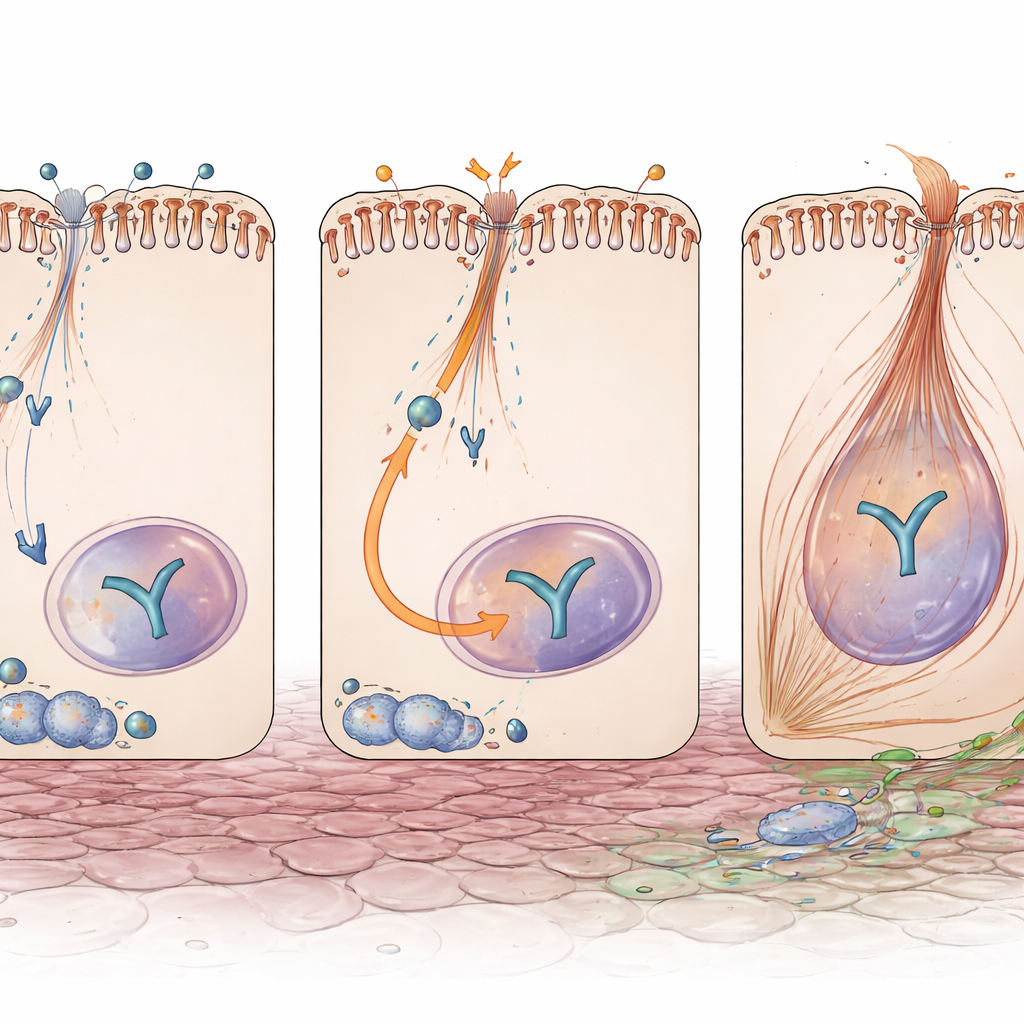
A Switch Linking Injury to Scarring Signals
Another central player in fibrosis is YAP, a signal-responsive protein that moves into the nucleus to turn on genes for growth and matrix production. Even without injury, tubules lacking Exoc5 had higher YAP protein levels. After obstruction, YAP was more strongly activated and concentrated in cell nuclei in these kidneys, and its downstream products—molecules known to drive fibrotic remodeling—were elevated. Importantly, this did not come from extra YAP gene activity, implying that Exoc5 normally restrains YAP at the protein or trafficking level. In cultured human kidney tubule cells, dialing down EXOC5 by RNA interference boosted YAP and Pax2, and made cells respond more strongly to the fibrotic signal TGF-β, with greater EMT-like changes and more cells acquiring contractile fibers typical of myofibroblasts.
What This Means for Future Treatments
Taken together, the findings portray Exoc5 as a quiet guardian: under stress, it helps tubule cells maintain their organized identity and keeps pro-scarring signals like YAP and Pax2 in check. When Exoc5 levels fall—whether through genetic loss or injury—tubule cells more readily lose their polarity, slip into a developmental-like state and feed the fibrotic process. Because deleting Exoc5 in proximal tubules did not harm healthy kidneys but clearly worsened scarring after injury, the work points to Exoc5 and its signaling partners as promising targets for therapies aimed at slowing or reversing kidney fibrosis before it progresses to kidney failure.
Citation: Lim, H.J., Han, Y.K., Noh, M.R. et al. Deficiency of exocyst complex component Exoc5 exacerbates the progression of kidney fibrosis. Exp Mol Med 58, 681–695 (2026). https://doi.org/10.1038/s12276-026-01649-8
Keywords: kidney fibrosis, Exoc5, epithelial-to-mesenchymal transition, YAP signaling, chronic kidney disease