Clear Sky Science · en
Regulation of allergies across the body by microbial metabolites
Why the Tiny Tenants in Our Bodies Matter
Allergic diseases such as eczema, hay fever, food allergy and asthma are rising worldwide, especially in children. This review article explains how the trillions of microbes living in our gut, skin and lungs help shape whether our bodies quietly tolerate pollen and peanuts—or overreact with rashes, wheezing and anaphylaxis. The authors focus on small chemicals made by these microbes, called metabolites, and show how they can either calm the immune system or fan the flames of allergy. Understanding these hidden chemical conversations could open safer, longer‑lasting ways to prevent and treat allergies through diet, probiotics and targeted microbial products.
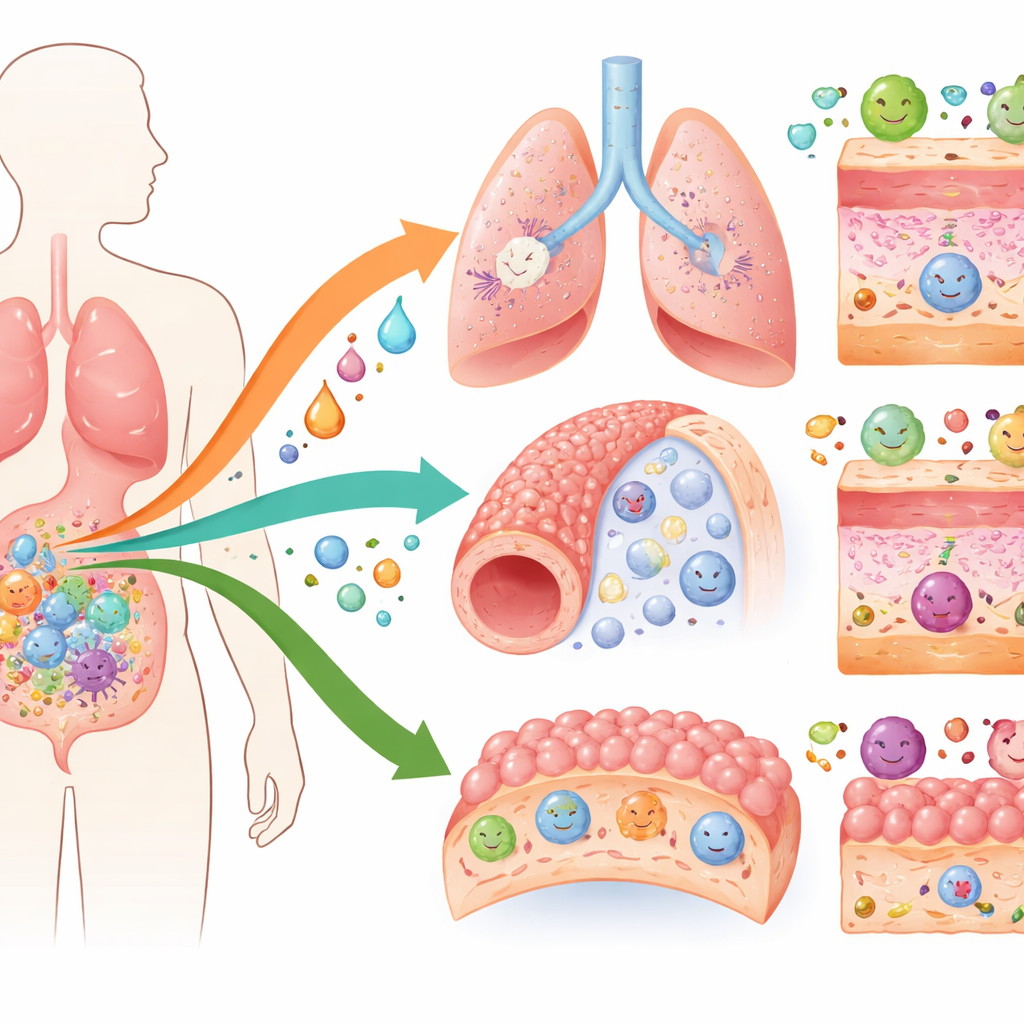
From Friendly Passengers to Chemical Factories
At birth, a baby’s gut and lungs are only beginning to be colonized by microbes. Over the first few years of life, this living community expands and diversifies, training the developing immune system. Children who grow up with a rich, balanced mix of microbes are more likely to develop strong immune tolerance; those whose microbial communities remain skewed or sparse are more prone to allergies later on. Microbes turn components of our diet—fibers, proteins and cholesterol—into a wide range of metabolites. Among the most important are short‑chain fatty acids made from fiber, indole compounds derived from the amino acid tryptophan, and transformed bile acids made from cholesterol. These products do not just float idly in the gut: they feed cells, switch genes on and off, and signal through dedicated receptors on immune and barrier cells throughout the body.
When Microbial Balance Tips Toward Allergy
In people with eczema, food allergies and respiratory allergies, the makeup of the microbiome is often altered, a state known as dysbiosis. Beneficial bacteria that normally produce protective metabolites are reduced, while harmful or inflammatory species expand. On the skin of children destined to develop eczema, for example, protective microbes lag behind while Staphylococcus aureus overgrows, weakening the skin barrier and disturbing lipid balance. In the gut of children with food allergy or asthma, helpful producers of fiber‑derived fatty acids and other soothing metabolites are often depleted, while other groups flourish in ways that do not support tolerance. These shifts change the pool of metabolites reaching the skin, lungs and intestine, nudging local immune cells toward allergic, rather than peaceful, behavior.
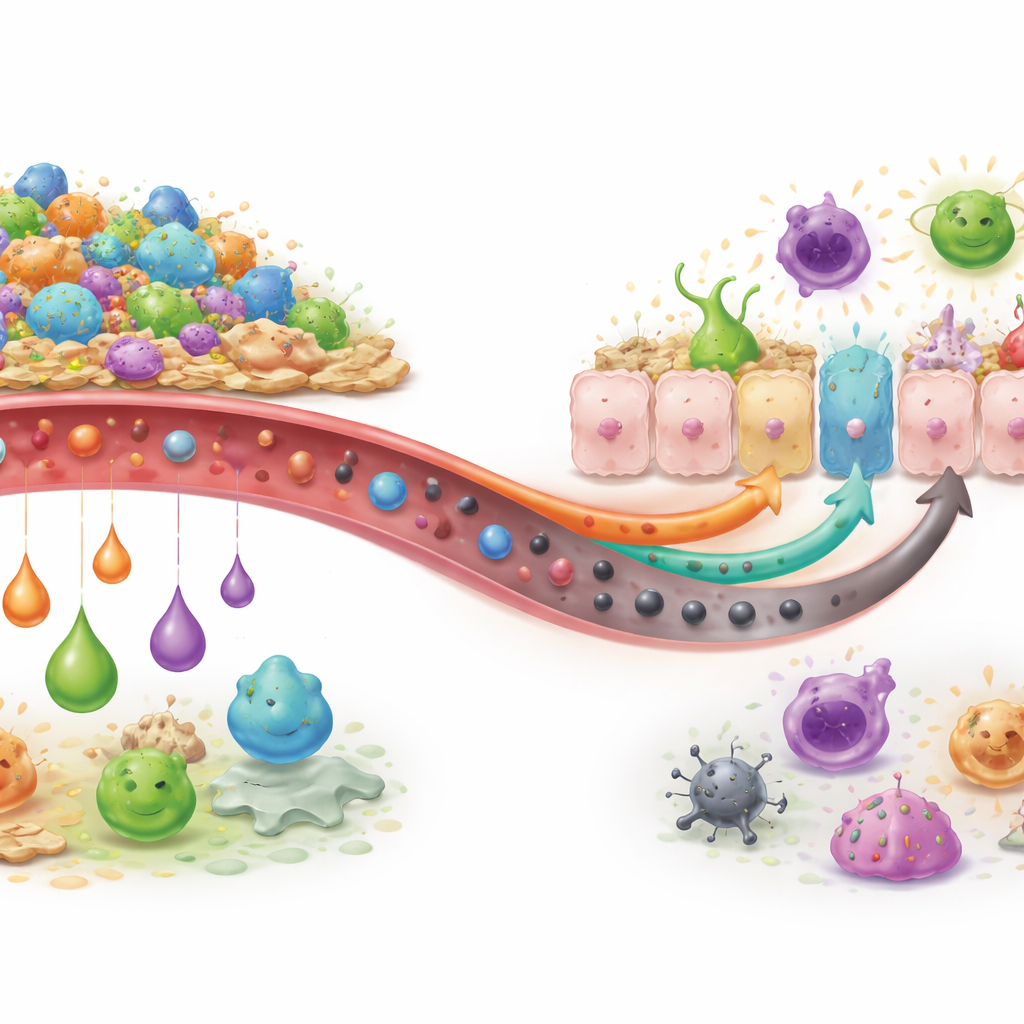
How Microbial Molecules Steer the Immune System
The review describes in plain terms how different metabolite families affect key tissues. Short‑chain fatty acids from fiber strengthen skin and gut barriers, fuel cell metabolism and dampen excessive inflammation. They encourage the growth of regulatory T cells that teach the immune system to live with everyday exposures, and they can directly restrain allergic troublemakers such as mast cells and certain innate lymphoid cells. Indole compounds from tryptophan act through a sensor in cells that helps shift responses away from classic allergy‑driven pathways. Bile acids, originally made to digest fats, are reshaped by gut microbes into variants that can either soothe or worsen inflammation, depending on their structure. Together, these signals influence whether epithelial barriers stay tight or leaky, whether antibody responses favor harmless IgA or allergy‑linked IgE, and whether cells in the skin, lungs and gut react calmly or hyperactively to the same allergens.
Different Organs, Shared Microbial Messages
Although the skin, lungs and intestines look very different, they share common themes in how they respond to microbial metabolites. All three rely on a strong surface barrier and a balanced mix of immune cells to separate the outside world from the bloodstream. When beneficial metabolites are plentiful, barrier cells are well nourished, protective antibodies coat microbes, and calming immune cells keep reactions in check. When dysbiosis reduces these helpful chemicals and increases irritating ones, barrier integrity falters and alarm signals rise. This invites more allergens into contact with immune cells, promotes the growth of type 2 immune responses that drive IgE production, and expands mast cells, eosinophils and other cells central to itching, wheezing and swelling. Over time, repeated allergen encounters in this primed state lead to chronic disease in the skin, lungs or gut.
New Paths to Calmer Immunity
The authors conclude that allergies are not only problems of genes and exposure but also of missing or misplaced microbial chemistry. Early life appears to be a critical window when the microbiome and its metabolites can set the long‑term tone of the immune system. This raises the possibility of steering allergy risk through diet rich in fermentable fibers, carefully chosen probiotics, or even purified microbial metabolites that bolster tolerance instead of reactivity. Such approaches might enhance existing therapies like desensitization shots or tablets, helping the immune system establish more durable peace with everyday allergens. At the same time, the review warns that powerful microbial products can have side effects, underscoring the need for precise dosing and safety testing as this promising new class of “chemical allies” is translated into real‑world allergy treatments.
Citation: Kim, C.H., Baker, J.R. Regulation of allergies across the body by microbial metabolites. Exp Mol Med 58, 396–407 (2026). https://doi.org/10.1038/s12276-026-01642-1
Keywords: microbiome, allergies, short-chain fatty acids, bile acids, immune tolerance