Clear Sky Science · en
Interferon regulatory factor 5 involves the pathogenesis of emphysema through NLRP3 and Ly6C expressing cells
Why this lung study matters
Chronic obstructive pulmonary disease (COPD) and emphysema rob millions of people of their breath, often long after they quit smoking. Current medicines can help open the airways, but they do little to calm the smoldering inflammation that keeps eating away at the lungs. This study uncovers a molecular "ringleader" of that damage, suggesting a new way to protect fragile air sacs and slow the decline in lung function.
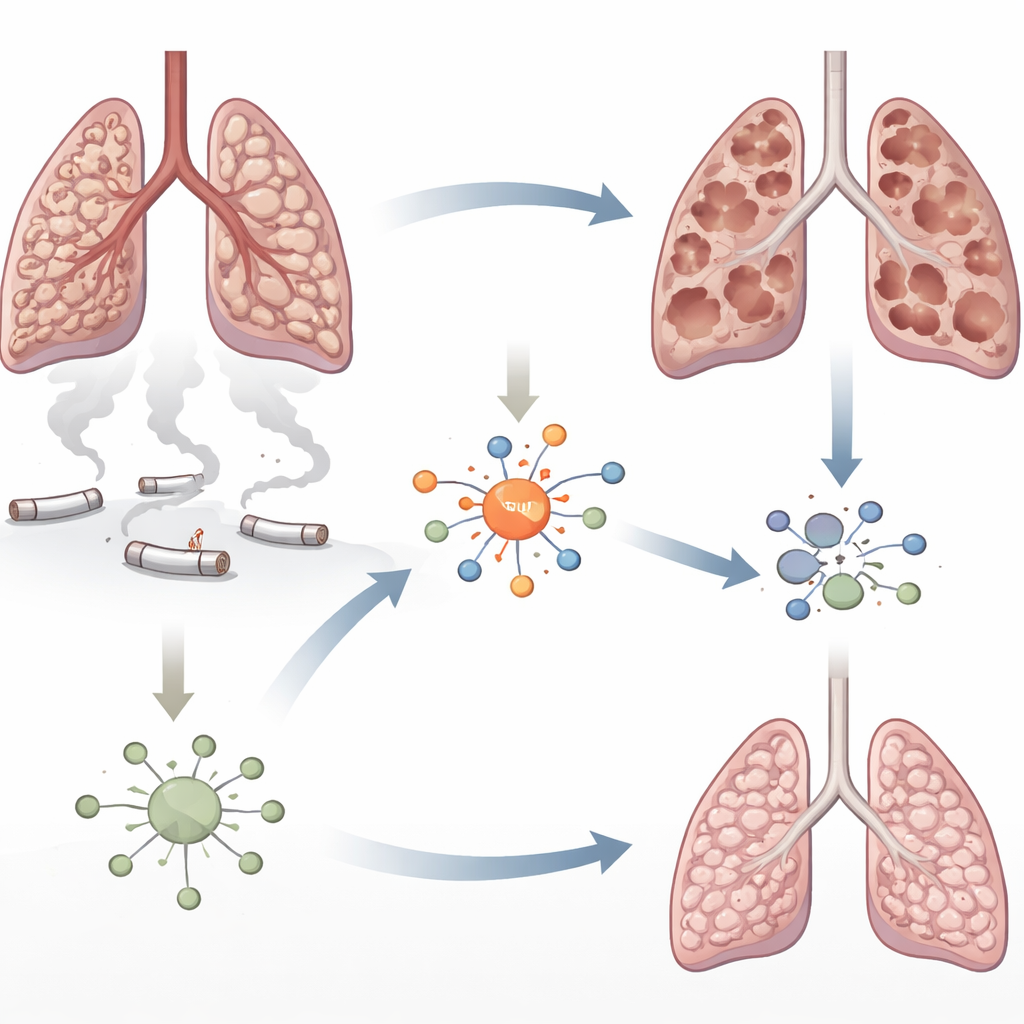
A closer look at smoke-damaged lungs
Emphysema is marked by the gradual breakdown of the tiny air sacs that exchange oxygen and carbon dioxide. Cigarette smoke bathes the lungs in toxic particles that injure cells and summon waves of immune cells. The authors focused on a protein called interferon regulatory factor 5 (IRF5), known to drive inflammation in autoimmune diseases but not well studied in COPD. Earlier work had hinted that IRF5 levels rise in smoke-exposed lungs. Here, the researchers set out to ask whether IRF5 simply tags along with inflammation or actually helps cause the destruction of lung tissue.
Shutting off a key switch in mice
To probe IRF5’s role, the team engineered mice that completely lack the gene for this protein. They then exposed normal and IRF5‑deficient animals to cigarette smoke for several weeks and compared the condition of their lungs. In normal mice, smoke caused clear signs of emphysema: the walls between neighboring air sacs were lost, leaving behind large, overinflated spaces. In contrast, mice without IRF5 were largely protected from this structural damage, even though smoke still brought immune cells into the air spaces and boosted many inflammatory molecules. This pointed to IRF5 as a crucial link between smoke exposure and the actual tearing down of lung architecture.
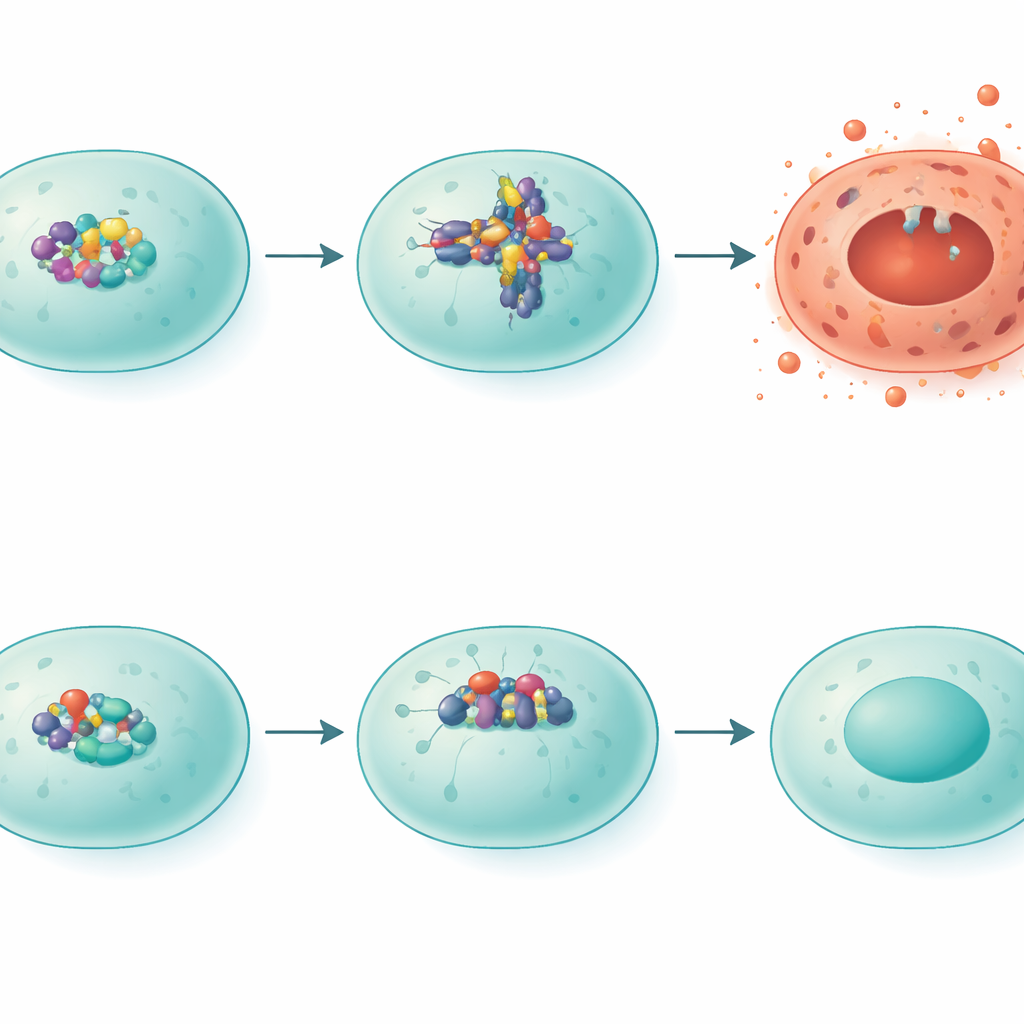
How IRF5 pushes cells toward fiery death
The researchers then zoomed in on a particular form of violent cell death called pyroptosis, which blows holes in cell membranes and spills inflammatory contents into surrounding tissue. A protein complex known as NLRP3 sits at the heart of this process. In smoke-exposed normal mice, NLRP3 levels rose, and patterns of another protein, gasdermin D, matched a pyroptosis-like state. In IRF5‑deficient mice, NLRP3 levels were much lower and gasdermin D was cut into alternative forms associated with less destructive outcomes. When the team artificially increased IRF5 in lung-related cells in the lab, NLRP3 levels climbed, confirming that IRF5 acts as a transcriptional switch that turns on this damaging pathway.
Protective immune cells step into the picture
IRF5 also reshaped the makeup of immune cells in the lung. In mice lacking IRF5, there was a marked rise in a subset of blood-derived cells strongly marked by a surface molecule called Ly6C. These Ly6C‑high cells included both monocytes and T cells and appeared in larger numbers after smoke exposure. When the scientists purified Ly6C‑high cells from IRF5‑deficient mice and infused them into ordinary smoke-exposed animals, the recipients developed less air sac destruction and showed reduced NLRP3 levels in the lung. Additional experiments revealed that IRF5 directly dampens the activity of the Ly6C gene, suggesting that when IRF5 is present, fewer of these potentially protective cells are produced or maintained.
Human lungs confirm the signal
To test whether these findings might matter for people, the authors examined lung tissue from patients undergoing surgery for lung cancer. They compared samples from individuals with good gas-exchange capacity to those with significant emphysema. IRF5 protein levels were substantially higher in lungs from the emphysema group. While this study was not large enough to tie IRF5 precisely to symptom severity or flare-ups, the pattern matched the mouse findings: more IRF5 in diseased lungs, less in healthier ones.
What this could mean for future treatments
Taken together, the work paints IRF5 as a central coordinator of smoke-driven lung injury. It boosts a cell-death engine centered on NLRP3 and steers immune cells away from Ly6C‑high populations that seem to help preserve air sac structure. For patients, the implication is straightforward: a drug that tones down IRF5 activity could, in theory, reduce the most destructive forms of inflammation without shutting the immune system off entirely. While such therapies do not yet exist for COPD, this study provides a clear molecular target and a biologically plausible path toward treatments that do more than open narrowed airways—they might actually protect the lung’s delicate scaffolding.
Citation: Heo, SH., Park, S.Y., Kim, N.H. et al. Interferon regulatory factor 5 involves the pathogenesis of emphysema through NLRP3 and Ly6C expressing cells. Exp Mol Med 58, 425–435 (2026). https://doi.org/10.1038/s12276-025-01632-9
Keywords: emphysema, COPD, inflammation, lung immunity, cell death